Now Available on Whatsapp:
+1 (888) 687-4420
Online 24/7
- College Essay
- Argumentative Essay
- Expository Essay
- Narrative Essay
- Descriptive Essay
- Scholarship Essay
- Admission Essay
- Reflective Essay
- Nursing Essay
- Economics Essay
Assignments
- Term Papers
- Research Papers
- Case Studies
- Dissertation
- Presentation
- Editing Help
- Cheap Essay Writing
- How to Order
Persuasive Essay Guide
Persuasive Essay About Covid19

How to Write a Persuasive Essay About Covid19 | Examples & Tips
14 min read

People also read
A Comprehensive Guide to Writing an Effective Persuasive Essay
A Catalogue of 300 Best Persuasive Essay Topics for Students
Persuasive Essay Outline - A Complete Guide
30+ Persuasive Essay Examples To Get You Started
Read Excellent Examples of Persuasive Essay About Gun Control
How To Write A Persuasive Essay On Abortion
Learn to Write a Persuasive Essay About Business With 5 Best Examples
Check Out 14 Persuasive Essays About Online Education Examples
Persuasive Essay About Smoking - Making a Powerful Argument with Examples
Are you looking to write a persuasive essay about the Covid-19 pandemic?
Writing a compelling and informative essay about this global crisis can be challenging. It requires researching the latest information, understanding the facts, and presenting your argument persuasively.
But don’t worry! with some guidance from experts, you’ll be able to write an effective and persuasive essay about Covid-19.
In this blog post, we’ll outline the basics of writing a persuasive essay . We’ll provide clear examples, helpful tips, and essential information for crafting your own persuasive piece on Covid-19.
Read on to get started on your essay.
- 1. Steps to Write a Persuasive Essay About Covid-19
- 2. Examples of Persuasive Essay About COVID-19
- 3. Examples of Persuasive Essay About COVID-19 Vaccine
- 4. Examples of Persuasive Essay About COVID-19 Integration
- 5. Examples of Argumentative Essay About Covid 19
- 6. Examples of Persuasive Speeches About Covid-19
- 7. Tips to Write a Persuasive Essay About Covid-19
- 8. Common Topics for a Persuasive Essay on COVID-19
Steps to Write a Persuasive Essay About Covid-19
Here are the steps to help you write a persuasive essay on this topic, along with an example essay:
Step 1: Choose a Specific Thesis Statement
Your thesis statement should clearly state your position on a specific aspect of COVID-19. It should be debatable and clear. For example:
Step 2: Research and Gather Information
Collect reliable and up-to-date information from reputable sources to support your thesis statement. This may include statistics, expert opinions, and scientific studies. For instance:
- COVID-19 vaccination effectiveness data
- Information on vaccine mandates in different countries
- Expert statements from health organizations like the WHO or CDC
Step 3: Outline Your Essay
Create a clear and organized outline to structure your essay. A persuasive essay typically follows this structure:
- Introduction
- Background Information
- Body Paragraphs (with supporting evidence)
- Counterarguments (addressing opposing views)
Step 4: Write the Introduction
In the introduction, grab your reader's attention and present your thesis statement. For example:
Step 5: Provide Background Information
Offer context and background information to help your readers understand the issue better. For instance:
Step 6: Develop Body Paragraphs
Each body paragraph should present a single point or piece of evidence that supports your thesis statement. Use clear topic sentences , evidence, and analysis. Here's an example:
Step 7: Address Counterarguments
Acknowledge opposing viewpoints and refute them with strong counterarguments. This demonstrates that you've considered different perspectives. For example:
Step 8: Write the Conclusion
Summarize your main points and restate your thesis statement in the conclusion. End with a strong call to action or thought-provoking statement. For instance:
Step 9: Revise and Proofread
Edit your essay for clarity, coherence, grammar, and spelling errors. Ensure that your argument flows logically.
Step 10: Cite Your Sources
Include proper citations and a bibliography page to give credit to your sources.
Remember to adjust your approach and arguments based on your target audience and the specific angle you want to take in your persuasive essay about COVID-19.

Paper Due? Why Suffer? That's our Job!
Examples of Persuasive Essay About COVID-19
When writing a persuasive essay about the COVID-19 pandemic, it’s important to consider how you want to present your argument. To help you get started, here are some example essays for you to read:
Here is another example explaining How COVID-19 has changed our lives essay:
Let’s look at another sample essay:
Check out some more PDF examples below:
Persuasive Essay About Covid-19 Pandemic
Sample Of Persuasive Essay About Covid-19
Persuasive Essay About Covid-19 In The Philippines - Example
If you're in search of a compelling persuasive essay on business, don't miss out on our “ persuasive essay about business ” blog!
Examples of Persuasive Essay About COVID-19 Vaccine
Covid19 vaccines are one of the ways to prevent the spread of COVID-19, but they have been a source of controversy. Different sides argue about the benefits or dangers of the new vaccines. Whatever your point of view is, writing a persuasive essay about it is a good way of organizing your thoughts and persuading others.
A persuasive essay about the COVID-19 vaccine could consider the benefits of getting vaccinated as well as the potential side effects.
Below are some examples of persuasive essays on getting vaccinated for Covid-19.
Covid19 Vaccine Persuasive Essay
Persuasive Essay on Covid Vaccines
Interested in thought-provoking discussions on abortion? Read our persuasive essay about abortion blog to eplore arguments!
Examples of Persuasive Essay About COVID-19 Integration
Covid19 has drastically changed the way people interact in schools, markets, and workplaces. In short, it has affected all aspects of life. However, people have started to learn to live with Covid19.
Writing a persuasive essay about it shouldn't be stressful. Read the sample essay below to get an idea for your own essay about Covid19 integration.
Persuasive Essay About Working From Home During Covid19
Searching for the topic of Online Education? Our persuasive essay about online education is a must-read.
Examples of Argumentative Essay About Covid 19
Covid-19 has been an ever-evolving issue, with new developments and discoveries being made on a daily basis.
Writing an argumentative essay about such an issue is both interesting and challenging. It allows you to evaluate different aspects of the pandemic, as well as consider potential solutions.
Here are some examples of argumentative essays on Covid19.
Argumentative Essay About Covid19 Sample
Argumentative Essay About Covid19 With Introduction Body and Conclusion
Looking for a persuasive take on the topic of smoking? You'll find it all related arguments in out Persuasive Essay About Smoking blog!
Examples of Persuasive Speeches About Covid-19
Do you need to prepare a speech about Covid19 and need examples? We have them for you!
Persuasive speeches about Covid-19 can provide the audience with valuable insights on how to best handle the pandemic. They can be used to advocate for specific changes in policies or simply raise awareness about the virus.
Check out some examples of persuasive speeches on Covid-19:
Persuasive Speech About Covid-19 Example
Persuasive Speech About Vaccine For Covid-19
You can also read persuasive essay examples on other topics to master your persuasive techniques!
Tips to Write a Persuasive Essay About Covid-19
Writing a persuasive essay about COVID-19 requires a thoughtful approach to present your arguments effectively.
Here are some tips to help you craft a compelling persuasive essay on this topic:
- Choose a Specific Angle: Narrow your focus to a specific aspect of COVID-19, like vaccination or public health measures.
- Provide Credible Sources: Support your arguments with reliable sources like scientific studies and government reports.
- Use Persuasive Language: Employ ethos, pathos, and logos , and use vivid examples to make your points relatable.
- Organize Your Essay: Create a solid persuasive essay outline and ensure a logical flow, with each paragraph focusing on a single point.
- Emphasize Benefits: Highlight how your suggestions can improve public health, safety, or well-being.
- Use Visuals: Incorporate graphs, charts, and statistics to reinforce your arguments.
- Call to Action: End your essay conclusion with a strong call to action, encouraging readers to take a specific step.
- Revise and Edit: Proofread for grammar, spelling, and clarity, ensuring smooth writing flow.
- Seek Feedback: Have someone else review your essay for valuable insights and improvements.
Tough Essay Due? Hire Tough Writers!
Common Topics for a Persuasive Essay on COVID-19
Here are some persuasive essay topics on COVID-19:
- The Importance of Vaccination Mandates for COVID-19 Control
- Balancing Public Health and Personal Freedom During a Pandemic
- The Economic Impact of Lockdowns vs. Public Health Benefits
- The Role of Misinformation in Fueling Vaccine Hesitancy
- Remote Learning vs. In-Person Education: What's Best for Students?
- The Ethics of Vaccine Distribution: Prioritizing Vulnerable Populations
- The Mental Health Crisis Amidst the COVID-19 Pandemic
- The Long-Term Effects of COVID-19 on Healthcare Systems
- Global Cooperation vs. Vaccine Nationalism in Fighting the Pandemic
- The Future of Telemedicine: Expanding Healthcare Access Post-COVID-19
In search of more inspiring topics for your next persuasive essay? Our persuasive essay topics blog has plenty of ideas!
To sum it up,
You’ve explored great sample essays and picked up some useful tips. You now have the tools you need to write a persuasive essay about Covid-19. So don’t let doubts hold you back—start writing!
If you’re feeling stuck or need a bit of extra help, don’t worry! MyPerfectWords.com offers a professional persuasive essay writing service that can assist you. Our experienced essay writers are ready to help you craft a well-structured, insightful paper on Covid-19.
Just place your “ do my essay for me ” request today, and let us take care of the rest!
Frequently Asked Questions
What is a good title for a covid-19 essay.
A good title for a COVID-19 essay should be clear, engaging, and reflective of the essay's content. Examples include:
- "The Impact of COVID-19 on Global Health"
- "How COVID-19 Has Transformed Our Daily Lives"
- "COVID-19: Lessons Learned and Future Implications"
How do I write an informative essay about COVID-19?
To write an informative essay about COVID-19, follow these steps:
- Choose a specific focus: Select a particular aspect of COVID-19, such as its transmission, symptoms, or vaccines.
- Research thoroughly: Gather information from credible sources like scientific journals and official health organizations.
- Organize your content: Structure your essay with an introduction, body paragraphs, and a conclusion.
- Present facts clearly: Use clear, concise language to convey information accurately.
- Include visuals: Use charts or graphs to illustrate data and make your essay more engaging.
How do I write an expository essay about COVID-19?
To write an expository essay about COVID-19, follow these steps:
- Select a clear topic: Focus on a specific question or issue related to COVID-19.
- Conduct thorough research: Use reliable sources to gather information.
- Create an outline: Organize your essay with an introduction, body paragraphs, and a conclusion.
- Explain the topic: Use facts and examples to explain the chosen aspect of COVID-19 in detail.
- Maintain objectivity: Present information in a neutral and unbiased manner.
- Edit and revise: Proofread your essay for clarity, coherence, and accuracy.

Write Essay Within 60 Seconds!

Caleb S. has been providing writing services for over five years and has a Masters degree from Oxford University. He is an expert in his craft and takes great pride in helping students achieve their academic goals. Caleb is a dedicated professional who always puts his clients first.
Struggling With Your Paper?
Get a custom paper written at
With a FREE Turnitin report, and a 100% money-back guarantee
LIMITED TIME ONLY!
Keep reading

OFFER EXPIRES SOON!
How to Write About Coronavirus in a College Essay
Students can share how they navigated life during the coronavirus pandemic in a full-length essay or an optional supplement.
Writing About COVID-19 in College Essays

Getty Images
Experts say students should be honest and not limit themselves to merely their experiences with the pandemic.
The global impact of COVID-19, the disease caused by the novel coronavirus, means colleges and prospective students alike are in for an admissions cycle like no other. Both face unprecedented challenges and questions as they grapple with their respective futures amid the ongoing fallout of the pandemic.
Colleges must examine applicants without the aid of standardized test scores for many – a factor that prompted many schools to go test-optional for now . Even grades, a significant component of a college application, may be hard to interpret with some high schools adopting pass-fail classes last spring due to the pandemic. Major college admissions factors are suddenly skewed.
"I can't help but think other (admissions) factors are going to matter more," says Ethan Sawyer, founder of the College Essay Guy, a website that offers free and paid essay-writing resources.
College essays and letters of recommendation , Sawyer says, are likely to carry more weight than ever in this admissions cycle. And many essays will likely focus on how the pandemic shaped students' lives throughout an often tumultuous 2020.
But before writing a college essay focused on the coronavirus, students should explore whether it's the best topic for them.
Writing About COVID-19 for a College Application
Much of daily life has been colored by the coronavirus. Virtual learning is the norm at many colleges and high schools, many extracurriculars have vanished and social lives have stalled for students complying with measures to stop the spread of COVID-19.
"For some young people, the pandemic took away what they envisioned as their senior year," says Robert Alexander, dean of admissions, financial aid and enrollment management at the University of Rochester in New York. "Maybe that's a spot on a varsity athletic team or the lead role in the fall play. And it's OK for them to mourn what should have been and what they feel like they lost, but more important is how are they making the most of the opportunities they do have?"
That question, Alexander says, is what colleges want answered if students choose to address COVID-19 in their college essay.
But the question of whether a student should write about the coronavirus is tricky. The answer depends largely on the student.
"In general, I don't think students should write about COVID-19 in their main personal statement for their application," Robin Miller, master college admissions counselor at IvyWise, a college counseling company, wrote in an email.
"Certainly, there may be exceptions to this based on a student's individual experience, but since the personal essay is the main place in the application where the student can really allow their voice to be heard and share insight into who they are as an individual, there are likely many other topics they can choose to write about that are more distinctive and unique than COVID-19," Miller says.
Opinions among admissions experts vary on whether to write about the likely popular topic of the pandemic.
"If your essay communicates something positive, unique, and compelling about you in an interesting and eloquent way, go for it," Carolyn Pippen, principal college admissions counselor at IvyWise, wrote in an email. She adds that students shouldn't be dissuaded from writing about a topic merely because it's common, noting that "topics are bound to repeat, no matter how hard we try to avoid it."
Above all, she urges honesty.
"If your experience within the context of the pandemic has been truly unique, then write about that experience, and the standing out will take care of itself," Pippen says. "If your experience has been generally the same as most other students in your context, then trying to find a unique angle can easily cross the line into exploiting a tragedy, or at least appearing as though you have."
But focusing entirely on the pandemic can limit a student to a single story and narrow who they are in an application, Sawyer says. "There are so many wonderful possibilities for what you can say about yourself outside of your experience within the pandemic."
He notes that passions, strengths, career interests and personal identity are among the multitude of essay topic options available to applicants and encourages them to probe their values to help determine the topic that matters most to them – and write about it.
That doesn't mean the pandemic experience has to be ignored if applicants feel the need to write about it.
Writing About Coronavirus in Main and Supplemental Essays
Students can choose to write a full-length college essay on the coronavirus or summarize their experience in a shorter form.
To help students explain how the pandemic affected them, The Common App has added an optional section to address this topic. Applicants have 250 words to describe their pandemic experience and the personal and academic impact of COVID-19.
"That's not a trick question, and there's no right or wrong answer," Alexander says. Colleges want to know, he adds, how students navigated the pandemic, how they prioritized their time, what responsibilities they took on and what they learned along the way.
If students can distill all of the above information into 250 words, there's likely no need to write about it in a full-length college essay, experts say. And applicants whose lives were not heavily altered by the pandemic may even choose to skip the optional COVID-19 question.
"This space is best used to discuss hardship and/or significant challenges that the student and/or the student's family experienced as a result of COVID-19 and how they have responded to those difficulties," Miller notes. Using the section to acknowledge a lack of impact, she adds, "could be perceived as trite and lacking insight, despite the good intentions of the applicant."
To guard against this lack of awareness, Sawyer encourages students to tap someone they trust to review their writing , whether it's the 250-word Common App response or the full-length essay.
Experts tend to agree that the short-form approach to this as an essay topic works better, but there are exceptions. And if a student does have a coronavirus story that he or she feels must be told, Alexander encourages the writer to be authentic in the essay.
"My advice for an essay about COVID-19 is the same as my advice about an essay for any topic – and that is, don't write what you think we want to read or hear," Alexander says. "Write what really changed you and that story that now is yours and yours alone to tell."
Sawyer urges students to ask themselves, "What's the sentence that only I can write?" He also encourages students to remember that the pandemic is only a chapter of their lives and not the whole book.
Miller, who cautions against writing a full-length essay on the coronavirus, says that if students choose to do so they should have a conversation with their high school counselor about whether that's the right move. And if students choose to proceed with COVID-19 as a topic, she says they need to be clear, detailed and insightful about what they learned and how they adapted along the way.
"Approaching the essay in this manner will provide important balance while demonstrating personal growth and vulnerability," Miller says.
Pippen encourages students to remember that they are in an unprecedented time for college admissions.
"It is important to keep in mind with all of these (admission) factors that no colleges have ever had to consider them this way in the selection process, if at all," Pippen says. "They have had very little time to calibrate their evaluations of different application components within their offices, let alone across institutions. This means that colleges will all be handling the admissions process a little bit differently, and their approaches may even evolve over the course of the admissions cycle."
Searching for a college? Get our complete rankings of Best Colleges.
10 Ways to Discover College Essay Ideas

Tags: students , colleges , college admissions , college applications , college search , Coronavirus
2025 Best Colleges

Search for your perfect fit with the U.S. News rankings of colleges and universities.
College Admissions: Get a Step Ahead!
Sign up to receive the latest updates from U.S. News & World Report and our trusted partners and sponsors. By clicking submit, you are agreeing to our Terms and Conditions & Privacy Policy .
Ask an Alum: Making the Most Out of College
You May Also Like
How to make a college list.
Cole Claybourn Nov. 6, 2024

Weighing LSAT Test Prep Options
Gabriel Kuris Nov. 4, 2024

Data Privacy Tips for College Students
Cole Claybourn Nov. 4, 2024

Preparing for Your First Job Post-Grad
Sarah Wood Oct. 31, 2024

5 Ways to Decrease Medical School Costs
Anayat Durrani Oct. 31, 2024

Graduate School with Student Loan Debt
A.R. Cabral Oct. 31, 2024

Colleges With Dog Mascots
Helen Lewis Oct. 31, 2024

15 Scholarships to Help Pay for College
Cole Claybourn and Alison Murtagh Oct. 29, 2024

Questions for Med School Social Events
Rachel Rizal Oct. 29, 2024

Schools for International Students
Sarah Wood Oct. 29, 2024

- Research article
- Open access
- Published: 04 June 2021
Coronavirus disease (COVID-19) pandemic: an overview of systematic reviews
- Israel Júnior Borges do Nascimento 1 , 2 ,
- Dónal P. O’Mathúna 3 , 4 ,
- Thilo Caspar von Groote 5 ,
- Hebatullah Mohamed Abdulazeem 6 ,
- Ishanka Weerasekara 7 , 8 ,
- Ana Marusic 9 ,
- Livia Puljak ORCID: orcid.org/0000-0002-8467-6061 10 ,
- Vinicius Tassoni Civile 11 ,
- Irena Zakarija-Grkovic 9 ,
- Tina Poklepovic Pericic 9 ,
- Alvaro Nagib Atallah 11 ,
- Santino Filoso 12 ,
- Nicola Luigi Bragazzi 13 &
- Milena Soriano Marcolino 1
On behalf of the International Network of Coronavirus Disease 2019 (InterNetCOVID-19)
BMC Infectious Diseases volume 21 , Article number: 525 ( 2021 ) Cite this article
19k Accesses
38 Citations
14 Altmetric
Metrics details
Navigating the rapidly growing body of scientific literature on the SARS-CoV-2 pandemic is challenging, and ongoing critical appraisal of this output is essential. We aimed to summarize and critically appraise systematic reviews of coronavirus disease (COVID-19) in humans that were available at the beginning of the pandemic.
Nine databases (Medline, EMBASE, Cochrane Library, CINAHL, Web of Sciences, PDQ-Evidence, WHO’s Global Research, LILACS, and Epistemonikos) were searched from December 1, 2019, to March 24, 2020. Systematic reviews analyzing primary studies of COVID-19 were included. Two authors independently undertook screening, selection, extraction (data on clinical symptoms, prevalence, pharmacological and non-pharmacological interventions, diagnostic test assessment, laboratory, and radiological findings), and quality assessment (AMSTAR 2). A meta-analysis was performed of the prevalence of clinical outcomes.
Eighteen systematic reviews were included; one was empty (did not identify any relevant study). Using AMSTAR 2, confidence in the results of all 18 reviews was rated as “critically low”. Identified symptoms of COVID-19 were (range values of point estimates): fever (82–95%), cough with or without sputum (58–72%), dyspnea (26–59%), myalgia or muscle fatigue (29–51%), sore throat (10–13%), headache (8–12%) and gastrointestinal complaints (5–9%). Severe symptoms were more common in men. Elevated C-reactive protein and lactate dehydrogenase, and slightly elevated aspartate and alanine aminotransferase, were commonly described. Thrombocytopenia and elevated levels of procalcitonin and cardiac troponin I were associated with severe disease. A frequent finding on chest imaging was uni- or bilateral multilobar ground-glass opacity. A single review investigated the impact of medication (chloroquine) but found no verifiable clinical data. All-cause mortality ranged from 0.3 to 13.9%.
Conclusions
In this overview of systematic reviews, we analyzed evidence from the first 18 systematic reviews that were published after the emergence of COVID-19. However, confidence in the results of all reviews was “critically low”. Thus, systematic reviews that were published early on in the pandemic were of questionable usefulness. Even during public health emergencies, studies and systematic reviews should adhere to established methodological standards.
Peer Review reports
The spread of the “Severe Acute Respiratory Coronavirus 2” (SARS-CoV-2), the causal agent of COVID-19, was characterized as a pandemic by the World Health Organization (WHO) in March 2020 and has triggered an international public health emergency [ 1 ]. The numbers of confirmed cases and deaths due to COVID-19 are rapidly escalating, counting in millions [ 2 ], causing massive economic strain, and escalating healthcare and public health expenses [ 3 , 4 ].
The research community has responded by publishing an impressive number of scientific reports related to COVID-19. The world was alerted to the new disease at the beginning of 2020 [ 1 ], and by mid-March 2020, more than 2000 articles had been published on COVID-19 in scholarly journals, with 25% of them containing original data [ 5 ]. The living map of COVID-19 evidence, curated by the Evidence for Policy and Practice Information and Co-ordinating Centre (EPPI-Centre), contained more than 40,000 records by February 2021 [ 6 ]. More than 100,000 records on PubMed were labeled as “SARS-CoV-2 literature, sequence, and clinical content” by February 2021 [ 7 ].
Due to publication speed, the research community has voiced concerns regarding the quality and reproducibility of evidence produced during the COVID-19 pandemic, warning of the potential damaging approach of “publish first, retract later” [ 8 ]. It appears that these concerns are not unfounded, as it has been reported that COVID-19 articles were overrepresented in the pool of retracted articles in 2020 [ 9 ]. These concerns about inadequate evidence are of major importance because they can lead to poor clinical practice and inappropriate policies [ 10 ].
Systematic reviews are a cornerstone of today’s evidence-informed decision-making. By synthesizing all relevant evidence regarding a particular topic, systematic reviews reflect the current scientific knowledge. Systematic reviews are considered to be at the highest level in the hierarchy of evidence and should be used to make informed decisions. However, with high numbers of systematic reviews of different scope and methodological quality being published, overviews of multiple systematic reviews that assess their methodological quality are essential [ 11 , 12 , 13 ]. An overview of systematic reviews helps identify and organize the literature and highlights areas of priority in decision-making.
In this overview of systematic reviews, we aimed to summarize and critically appraise systematic reviews of coronavirus disease (COVID-19) in humans that were available at the beginning of the pandemic.
Methodology
Research question.
This overview’s primary objective was to summarize and critically appraise systematic reviews that assessed any type of primary clinical data from patients infected with SARS-CoV-2. Our research question was purposefully broad because we wanted to analyze as many systematic reviews as possible that were available early following the COVID-19 outbreak.
Study design
We conducted an overview of systematic reviews. The idea for this overview originated in a protocol for a systematic review submitted to PROSPERO (CRD42020170623), which indicated a plan to conduct an overview.
Overviews of systematic reviews use explicit and systematic methods for searching and identifying multiple systematic reviews addressing related research questions in the same field to extract and analyze evidence across important outcomes. Overviews of systematic reviews are in principle similar to systematic reviews of interventions, but the unit of analysis is a systematic review [ 14 , 15 , 16 ].
We used the overview methodology instead of other evidence synthesis methods to allow us to collate and appraise multiple systematic reviews on this topic, and to extract and analyze their results across relevant topics [ 17 ]. The overview and meta-analysis of systematic reviews allowed us to investigate the methodological quality of included studies, summarize results, and identify specific areas of available or limited evidence, thereby strengthening the current understanding of this novel disease and guiding future research [ 13 ].
A reporting guideline for overviews of reviews is currently under development, i.e., Preferred Reporting Items for Overviews of Reviews (PRIOR) [ 18 ]. As the PRIOR checklist is still not published, this study was reported following the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) 2009 statement [ 19 ]. The methodology used in this review was adapted from the Cochrane Handbook for Systematic Reviews of Interventions and also followed established methodological considerations for analyzing existing systematic reviews [ 14 ].
Approval of a research ethics committee was not necessary as the study analyzed only publicly available articles.
Eligibility criteria
Systematic reviews were included if they analyzed primary data from patients infected with SARS-CoV-2 as confirmed by RT-PCR or another pre-specified diagnostic technique. Eligible reviews covered all topics related to COVID-19 including, but not limited to, those that reported clinical symptoms, diagnostic methods, therapeutic interventions, laboratory findings, or radiological results. Both full manuscripts and abbreviated versions, such as letters, were eligible.
No restrictions were imposed on the design of the primary studies included within the systematic reviews, the last search date, whether the review included meta-analyses or language. Reviews related to SARS-CoV-2 and other coronaviruses were eligible, but from those reviews, we analyzed only data related to SARS-CoV-2.
No consensus definition exists for a systematic review [ 20 ], and debates continue about the defining characteristics of a systematic review [ 21 ]. Cochrane’s guidance for overviews of reviews recommends setting pre-established criteria for making decisions around inclusion [ 14 ]. That is supported by a recent scoping review about guidance for overviews of systematic reviews [ 22 ].
Thus, for this study, we defined a systematic review as a research report which searched for primary research studies on a specific topic using an explicit search strategy, had a detailed description of the methods with explicit inclusion criteria provided, and provided a summary of the included studies either in narrative or quantitative format (such as a meta-analysis). Cochrane and non-Cochrane systematic reviews were considered eligible for inclusion, with or without meta-analysis, and regardless of the study design, language restriction and methodology of the included primary studies. To be eligible for inclusion, reviews had to be clearly analyzing data related to SARS-CoV-2 (associated or not with other viruses). We excluded narrative reviews without those characteristics as these are less likely to be replicable and are more prone to bias.
Scoping reviews and rapid reviews were eligible for inclusion in this overview if they met our pre-defined inclusion criteria noted above. We included reviews that addressed SARS-CoV-2 and other coronaviruses if they reported separate data regarding SARS-CoV-2.
Information sources
Nine databases were searched for eligible records published between December 1, 2019, and March 24, 2020: Cochrane Database of Systematic Reviews via Cochrane Library, PubMed, EMBASE, CINAHL (Cumulative Index to Nursing and Allied Health Literature), Web of Sciences, LILACS (Latin American and Caribbean Health Sciences Literature), PDQ-Evidence, WHO’s Global Research on Coronavirus Disease (COVID-19), and Epistemonikos.
The comprehensive search strategy for each database is provided in Additional file 1 and was designed and conducted in collaboration with an information specialist. All retrieved records were primarily processed in EndNote, where duplicates were removed, and records were then imported into the Covidence platform [ 23 ]. In addition to database searches, we screened reference lists of reviews included after screening records retrieved via databases.
Study selection
All searches, screening of titles and abstracts, and record selection, were performed independently by two investigators using the Covidence platform [ 23 ]. Articles deemed potentially eligible were retrieved for full-text screening carried out independently by two investigators. Discrepancies at all stages were resolved by consensus. During the screening, records published in languages other than English were translated by a native/fluent speaker.
Data collection process
We custom designed a data extraction table for this study, which was piloted by two authors independently. Data extraction was performed independently by two authors. Conflicts were resolved by consensus or by consulting a third researcher.
We extracted the following data: article identification data (authors’ name and journal of publication), search period, number of databases searched, population or settings considered, main results and outcomes observed, and number of participants. From Web of Science (Clarivate Analytics, Philadelphia, PA, USA), we extracted journal rank (quartile) and Journal Impact Factor (JIF).
We categorized the following as primary outcomes: all-cause mortality, need for and length of mechanical ventilation, length of hospitalization (in days), admission to intensive care unit (yes/no), and length of stay in the intensive care unit.
The following outcomes were categorized as exploratory: diagnostic methods used for detection of the virus, male to female ratio, clinical symptoms, pharmacological and non-pharmacological interventions, laboratory findings (full blood count, liver enzymes, C-reactive protein, d-dimer, albumin, lipid profile, serum electrolytes, blood vitamin levels, glucose levels, and any other important biomarkers), and radiological findings (using radiography, computed tomography, magnetic resonance imaging or ultrasound).
We also collected data on reporting guidelines and requirements for the publication of systematic reviews and meta-analyses from journal websites where included reviews were published.
Quality assessment in individual reviews
Two researchers independently assessed the reviews’ quality using the “A MeaSurement Tool to Assess Systematic Reviews 2 (AMSTAR 2)”. We acknowledge that the AMSTAR 2 was created as “a critical appraisal tool for systematic reviews that include randomized or non-randomized studies of healthcare interventions, or both” [ 24 ]. However, since AMSTAR 2 was designed for systematic reviews of intervention trials, and we included additional types of systematic reviews, we adjusted some AMSTAR 2 ratings and reported these in Additional file 2 .
Adherence to each item was rated as follows: yes, partial yes, no, or not applicable (such as when a meta-analysis was not conducted). The overall confidence in the results of the review is rated as “critically low”, “low”, “moderate” or “high”, according to the AMSTAR 2 guidance based on seven critical domains, which are items 2, 4, 7, 9, 11, 13, 15 as defined by AMSTAR 2 authors [ 24 ]. We reported our adherence ratings for transparency of our decision with accompanying explanations, for each item, in each included review.
One of the included systematic reviews was conducted by some members of this author team [ 25 ]. This review was initially assessed independently by two authors who were not co-authors of that review to prevent the risk of bias in assessing this study.
Synthesis of results
For data synthesis, we prepared a table summarizing each systematic review. Graphs illustrating the mortality rate and clinical symptoms were created. We then prepared a narrative summary of the methods, findings, study strengths, and limitations.
For analysis of the prevalence of clinical outcomes, we extracted data on the number of events and the total number of patients to perform proportional meta-analysis using RStudio© software, with the “meta” package (version 4.9–6), using the “metaprop” function for reviews that did not perform a meta-analysis, excluding case studies because of the absence of variance. For reviews that did not perform a meta-analysis, we presented pooled results of proportions with their respective confidence intervals (95%) by the inverse variance method with a random-effects model, using the DerSimonian-Laird estimator for τ 2 . We adjusted data using Freeman-Tukey double arcosen transformation. Confidence intervals were calculated using the Clopper-Pearson method for individual studies. We created forest plots using the RStudio© software, with the “metafor” package (version 2.1–0) and “forest” function.
Managing overlapping systematic reviews
Some of the included systematic reviews that address the same or similar research questions may include the same primary studies in overviews. Including such overlapping reviews may introduce bias when outcome data from the same primary study are included in the analyses of an overview multiple times. Thus, in summaries of evidence, multiple-counting of the same outcome data will give data from some primary studies too much influence [ 14 ]. In this overview, we did not exclude overlapping systematic reviews because, according to Cochrane’s guidance, it may be appropriate to include all relevant reviews’ results if the purpose of the overview is to present and describe the current body of evidence on a topic [ 14 ]. To avoid any bias in summary estimates associated with overlapping reviews, we generated forest plots showing data from individual systematic reviews, but the results were not pooled because some primary studies were included in multiple reviews.
Our search retrieved 1063 publications, of which 175 were duplicates. Most publications were excluded after the title and abstract analysis ( n = 860). Among the 28 studies selected for full-text screening, 10 were excluded for the reasons described in Additional file 3 , and 18 were included in the final analysis (Fig. 1 ) [ 25 , 26 , 27 , 28 , 29 , 30 , 31 , 32 , 33 , 34 , 35 , 36 , 37 , 38 , 39 , 40 , 41 , 42 ]. Reference list screening did not retrieve any additional systematic reviews.
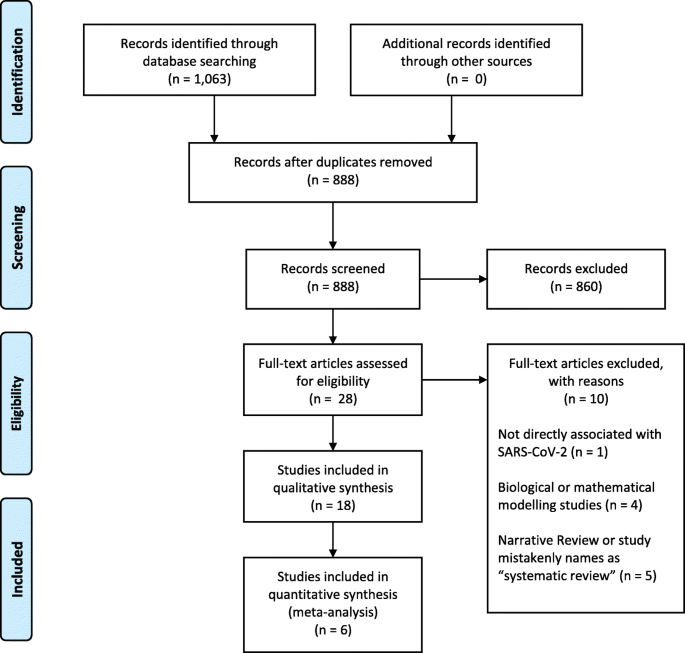
PRISMA flow diagram
Characteristics of included reviews
Summary features of 18 systematic reviews are presented in Table 1 . They were published in 14 different journals. Only four of these journals had specific requirements for systematic reviews (with or without meta-analysis): European Journal of Internal Medicine, Journal of Clinical Medicine, Ultrasound in Obstetrics and Gynecology, and Clinical Research in Cardiology . Two journals reported that they published only invited reviews ( Journal of Medical Virology and Clinica Chimica Acta ). Three systematic reviews in our study were published as letters; one was labeled as a scoping review and another as a rapid review (Table 2 ).
All reviews were published in English, in first quartile (Q1) journals, with JIF ranging from 1.692 to 6.062. One review was empty, meaning that its search did not identify any relevant studies; i.e., no primary studies were included [ 36 ]. The remaining 17 reviews included 269 unique studies; the majority ( N = 211; 78%) were included in only a single review included in our study (range: 1 to 12). Primary studies included in the reviews were published between December 2019 and March 18, 2020, and comprised case reports, case series, cohorts, and other observational studies. We found only one review that included randomized clinical trials [ 38 ]. In the included reviews, systematic literature searches were performed from 2019 (entire year) up to March 9, 2020. Ten systematic reviews included meta-analyses. The list of primary studies found in the included systematic reviews is shown in Additional file 4 , as well as the number of reviews in which each primary study was included.
Population and study designs
Most of the reviews analyzed data from patients with COVID-19 who developed pneumonia, acute respiratory distress syndrome (ARDS), or any other correlated complication. One review aimed to evaluate the effectiveness of using surgical masks on preventing transmission of the virus [ 36 ], one review was focused on pediatric patients [ 34 ], and one review investigated COVID-19 in pregnant women [ 37 ]. Most reviews assessed clinical symptoms, laboratory findings, or radiological results.
Systematic review findings
The summary of findings from individual reviews is shown in Table 2 . Overall, all-cause mortality ranged from 0.3 to 13.9% (Fig. 2 ).
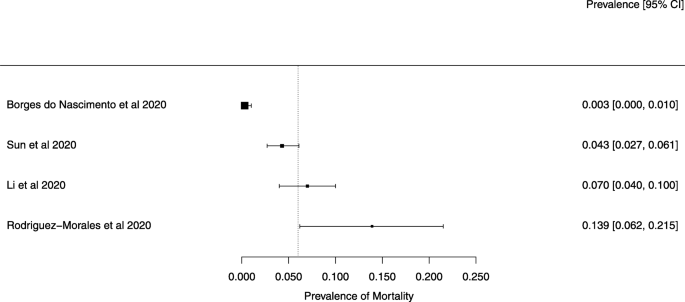
A meta-analysis of the prevalence of mortality
Clinical symptoms
Seven reviews described the main clinical manifestations of COVID-19 [ 26 , 28 , 29 , 34 , 35 , 39 , 41 ]. Three of them provided only a narrative discussion of symptoms [ 26 , 34 , 35 ]. In the reviews that performed a statistical analysis of the incidence of different clinical symptoms, symptoms in patients with COVID-19 were (range values of point estimates): fever (82–95%), cough with or without sputum (58–72%), dyspnea (26–59%), myalgia or muscle fatigue (29–51%), sore throat (10–13%), headache (8–12%), gastrointestinal disorders, such as diarrhea, nausea or vomiting (5.0–9.0%), and others (including, in one study only: dizziness 12.1%) (Figs. 3 , 4 , 5 , 6 , 7 , 8 and 9 ). Three reviews assessed cough with and without sputum together; only one review assessed sputum production itself (28.5%).
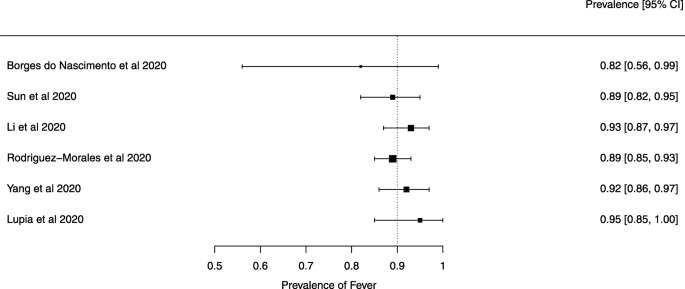
A meta-analysis of the prevalence of fever
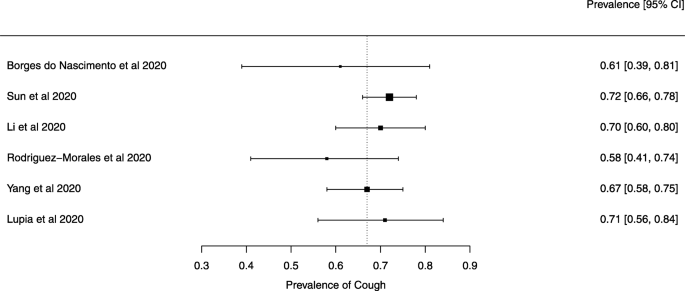
A meta-analysis of the prevalence of cough
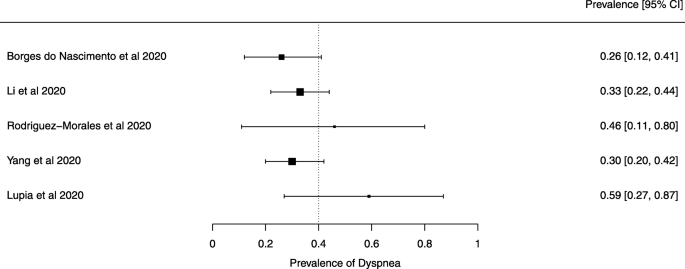
A meta-analysis of the prevalence of dyspnea
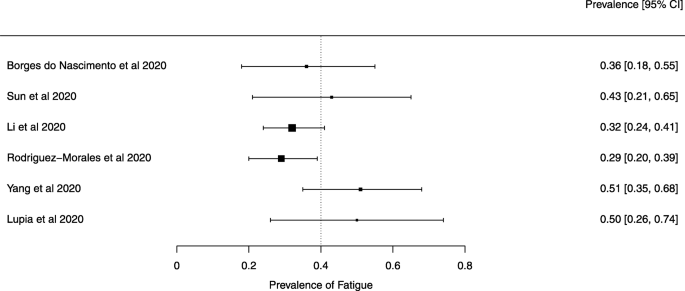
A meta-analysis of the prevalence of fatigue or myalgia
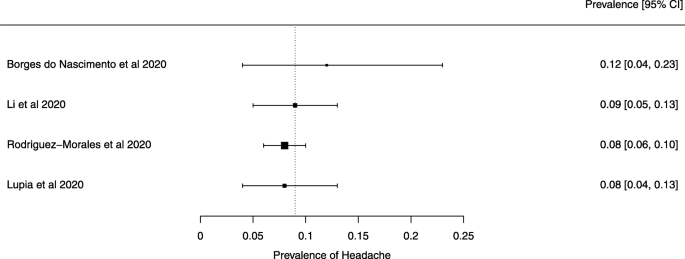
A meta-analysis of the prevalence of headache
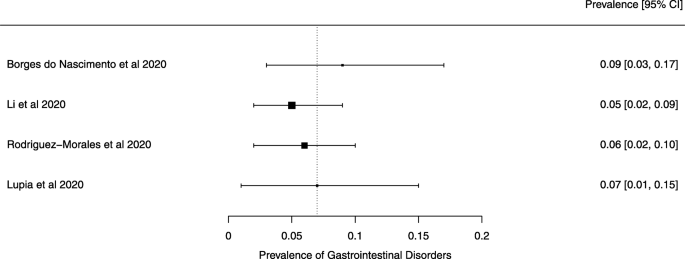
A meta-analysis of the prevalence of gastrointestinal disorders
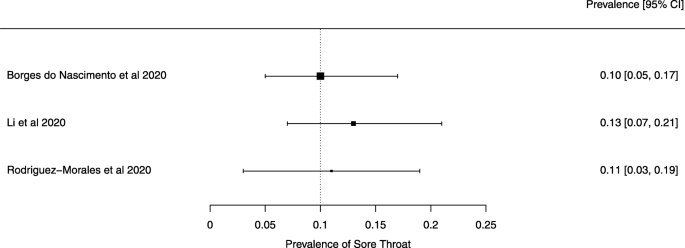
A meta-analysis of the prevalence of sore throat
Diagnostic aspects
Three reviews described methodologies, protocols, and tools used for establishing the diagnosis of COVID-19 [ 26 , 34 , 38 ]. The use of respiratory swabs (nasal or pharyngeal) or blood specimens to assess the presence of SARS-CoV-2 nucleic acid using RT-PCR assays was the most commonly used diagnostic method mentioned in the included studies. These diagnostic tests have been widely used, but their precise sensitivity and specificity remain unknown. One review included a Chinese study with clinical diagnosis with no confirmation of SARS-CoV-2 infection (patients were diagnosed with COVID-19 if they presented with at least two symptoms suggestive of COVID-19, together with laboratory and chest radiography abnormalities) [ 34 ].
Therapeutic possibilities
Pharmacological and non-pharmacological interventions (supportive therapies) used in treating patients with COVID-19 were reported in five reviews [ 25 , 27 , 34 , 35 , 38 ]. Antivirals used empirically for COVID-19 treatment were reported in seven reviews [ 25 , 27 , 34 , 35 , 37 , 38 , 41 ]; most commonly used were protease inhibitors (lopinavir, ritonavir, darunavir), nucleoside reverse transcriptase inhibitor (tenofovir), nucleotide analogs (remdesivir, galidesivir, ganciclovir), and neuraminidase inhibitors (oseltamivir). Umifenovir, a membrane fusion inhibitor, was investigated in two studies [ 25 , 35 ]. Possible supportive interventions analyzed were different types of oxygen supplementation and breathing support (invasive or non-invasive ventilation) [ 25 ]. The use of antibiotics, both empirically and to treat secondary pneumonia, was reported in six studies [ 25 , 26 , 27 , 34 , 35 , 38 ]. One review specifically assessed evidence on the efficacy and safety of the anti-malaria drug chloroquine [ 27 ]. It identified 23 ongoing trials investigating the potential of chloroquine as a therapeutic option for COVID-19, but no verifiable clinical outcomes data. The use of mesenchymal stem cells, antifungals, and glucocorticoids were described in four reviews [ 25 , 34 , 35 , 38 ].
Laboratory and radiological findings
Of the 18 reviews included in this overview, eight analyzed laboratory parameters in patients with COVID-19 [ 25 , 29 , 30 , 32 , 33 , 34 , 35 , 39 ]; elevated C-reactive protein levels, associated with lymphocytopenia, elevated lactate dehydrogenase, as well as slightly elevated aspartate and alanine aminotransferase (AST, ALT) were commonly described in those eight reviews. Lippi et al. assessed cardiac troponin I (cTnI) [ 25 ], procalcitonin [ 32 ], and platelet count [ 33 ] in COVID-19 patients. Elevated levels of procalcitonin [ 32 ] and cTnI [ 30 ] were more likely to be associated with a severe disease course (requiring intensive care unit admission and intubation). Furthermore, thrombocytopenia was frequently observed in patients with complicated COVID-19 infections [ 33 ].
Chest imaging (chest radiography and/or computed tomography) features were assessed in six reviews, all of which described a frequent pattern of local or bilateral multilobar ground-glass opacity [ 25 , 34 , 35 , 39 , 40 , 41 ]. Those six reviews showed that septal thickening, bronchiectasis, pleural and cardiac effusions, halo signs, and pneumothorax were observed in patients suffering from COVID-19.
Quality of evidence in individual systematic reviews
Table 3 shows the detailed results of the quality assessment of 18 systematic reviews, including the assessment of individual items and summary assessment. A detailed explanation for each decision in each review is available in Additional file 5 .
Using AMSTAR 2 criteria, confidence in the results of all 18 reviews was rated as “critically low” (Table 3 ). Common methodological drawbacks were: omission of prospective protocol submission or publication; use of inappropriate search strategy: lack of independent and dual literature screening and data-extraction (or methodology unclear); absence of an explanation for heterogeneity among the studies included; lack of reasons for study exclusion (or rationale unclear).
Risk of bias assessment, based on a reported methodological tool, and quality of evidence appraisal, in line with the Grading of Recommendations Assessment, Development, and Evaluation (GRADE) method, were reported only in one review [ 25 ]. Five reviews presented a table summarizing bias, using various risk of bias tools [ 25 , 29 , 39 , 40 , 41 ]. One review analyzed “study quality” [ 37 ]. One review mentioned the risk of bias assessment in the methodology but did not provide any related analysis [ 28 ].
This overview of systematic reviews analyzed the first 18 systematic reviews published after the onset of the COVID-19 pandemic, up to March 24, 2020, with primary studies involving more than 60,000 patients. Using AMSTAR-2, we judged that our confidence in all those reviews was “critically low”. Ten reviews included meta-analyses. The reviews presented data on clinical manifestations, laboratory and radiological findings, and interventions. We found no systematic reviews on the utility of diagnostic tests.
Symptoms were reported in seven reviews; most of the patients had a fever, cough, dyspnea, myalgia or muscle fatigue, and gastrointestinal disorders such as diarrhea, nausea, or vomiting. Olfactory dysfunction (anosmia or dysosmia) has been described in patients infected with COVID-19 [ 43 ]; however, this was not reported in any of the reviews included in this overview. During the SARS outbreak in 2002, there were reports of impairment of the sense of smell associated with the disease [ 44 , 45 ].
The reported mortality rates ranged from 0.3 to 14% in the included reviews. Mortality estimates are influenced by the transmissibility rate (basic reproduction number), availability of diagnostic tools, notification policies, asymptomatic presentations of the disease, resources for disease prevention and control, and treatment facilities; variability in the mortality rate fits the pattern of emerging infectious diseases [ 46 ]. Furthermore, the reported cases did not consider asymptomatic cases, mild cases where individuals have not sought medical treatment, and the fact that many countries had limited access to diagnostic tests or have implemented testing policies later than the others. Considering the lack of reviews assessing diagnostic testing (sensitivity, specificity, and predictive values of RT-PCT or immunoglobulin tests), and the preponderance of studies that assessed only symptomatic individuals, considerable imprecision around the calculated mortality rates existed in the early stage of the COVID-19 pandemic.
Few reviews included treatment data. Those reviews described studies considered to be at a very low level of evidence: usually small, retrospective studies with very heterogeneous populations. Seven reviews analyzed laboratory parameters; those reviews could have been useful for clinicians who attend patients suspected of COVID-19 in emergency services worldwide, such as assessing which patients need to be reassessed more frequently.
All systematic reviews scored poorly on the AMSTAR 2 critical appraisal tool for systematic reviews. Most of the original studies included in the reviews were case series and case reports, impacting the quality of evidence. Such evidence has major implications for clinical practice and the use of these reviews in evidence-based practice and policy. Clinicians, patients, and policymakers can only have the highest confidence in systematic review findings if high-quality systematic review methodologies are employed. The urgent need for information during a pandemic does not justify poor quality reporting.
We acknowledge that there are numerous challenges associated with analyzing COVID-19 data during a pandemic [ 47 ]. High-quality evidence syntheses are needed for decision-making, but each type of evidence syntheses is associated with its inherent challenges.
The creation of classic systematic reviews requires considerable time and effort; with massive research output, they quickly become outdated, and preparing updated versions also requires considerable time. A recent study showed that updates of non-Cochrane systematic reviews are published a median of 5 years after the publication of the previous version [ 48 ].
Authors may register a review and then abandon it [ 49 ], but the existence of a public record that is not updated may lead other authors to believe that the review is still ongoing. A quarter of Cochrane review protocols remains unpublished as completed systematic reviews 8 years after protocol publication [ 50 ].
Rapid reviews can be used to summarize the evidence, but they involve methodological sacrifices and simplifications to produce information promptly, with inconsistent methodological approaches [ 51 ]. However, rapid reviews are justified in times of public health emergencies, and even Cochrane has resorted to publishing rapid reviews in response to the COVID-19 crisis [ 52 ]. Rapid reviews were eligible for inclusion in this overview, but only one of the 18 reviews included in this study was labeled as a rapid review.
Ideally, COVID-19 evidence would be continually summarized in a series of high-quality living systematic reviews, types of evidence synthesis defined as “ a systematic review which is continually updated, incorporating relevant new evidence as it becomes available ” [ 53 ]. However, conducting living systematic reviews requires considerable resources, calling into question the sustainability of such evidence synthesis over long periods [ 54 ].
Research reports about COVID-19 will contribute to research waste if they are poorly designed, poorly reported, or simply not necessary. In principle, systematic reviews should help reduce research waste as they usually provide recommendations for further research that is needed or may advise that sufficient evidence exists on a particular topic [ 55 ]. However, systematic reviews can also contribute to growing research waste when they are not needed, or poorly conducted and reported. Our present study clearly shows that most of the systematic reviews that were published early on in the COVID-19 pandemic could be categorized as research waste, as our confidence in their results is critically low.
Our study has some limitations. One is that for AMSTAR 2 assessment we relied on information available in publications; we did not attempt to contact study authors for clarifications or additional data. In three reviews, the methodological quality appraisal was challenging because they were published as letters, or labeled as rapid communications. As a result, various details about their review process were not included, leading to AMSTAR 2 questions being answered as “not reported”, resulting in low confidence scores. Full manuscripts might have provided additional information that could have led to higher confidence in the results. In other words, low scores could reflect incomplete reporting, not necessarily low-quality review methods. To make their review available more rapidly and more concisely, the authors may have omitted methodological details. A general issue during a crisis is that speed and completeness must be balanced. However, maintaining high standards requires proper resourcing and commitment to ensure that the users of systematic reviews can have high confidence in the results.
Furthermore, we used adjusted AMSTAR 2 scoring, as the tool was designed for critical appraisal of reviews of interventions. Some reviews may have received lower scores than actually warranted in spite of these adjustments.
Another limitation of our study may be the inclusion of multiple overlapping reviews, as some included reviews included the same primary studies. According to the Cochrane Handbook, including overlapping reviews may be appropriate when the review’s aim is “ to present and describe the current body of systematic review evidence on a topic ” [ 12 ], which was our aim. To avoid bias with summarizing evidence from overlapping reviews, we presented the forest plots without summary estimates. The forest plots serve to inform readers about the effect sizes for outcomes that were reported in each review.
Several authors from this study have contributed to one of the reviews identified [ 25 ]. To reduce the risk of any bias, two authors who did not co-author the review in question initially assessed its quality and limitations.
Finally, we note that the systematic reviews included in our overview may have had issues that our analysis did not identify because we did not analyze their primary studies to verify the accuracy of the data and information they presented. We give two examples to substantiate this possibility. Lovato et al. wrote a commentary on the review of Sun et al. [ 41 ], in which they criticized the authors’ conclusion that sore throat is rare in COVID-19 patients [ 56 ]. Lovato et al. highlighted that multiple studies included in Sun et al. did not accurately describe participants’ clinical presentations, warning that only three studies clearly reported data on sore throat [ 56 ].
In another example, Leung [ 57 ] warned about the review of Li, L.Q. et al. [ 29 ]: “ it is possible that this statistic was computed using overlapped samples, therefore some patients were double counted ”. Li et al. responded to Leung that it is uncertain whether the data overlapped, as they used data from published articles and did not have access to the original data; they also reported that they requested original data and that they plan to re-do their analyses once they receive them; they also urged readers to treat the data with caution [ 58 ]. This points to the evolving nature of evidence during a crisis.
Our study’s strength is that this overview adds to the current knowledge by providing a comprehensive summary of all the evidence synthesis about COVID-19 available early after the onset of the pandemic. This overview followed strict methodological criteria, including a comprehensive and sensitive search strategy and a standard tool for methodological appraisal of systematic reviews.
In conclusion, in this overview of systematic reviews, we analyzed evidence from the first 18 systematic reviews that were published after the emergence of COVID-19. However, confidence in the results of all the reviews was “critically low”. Thus, systematic reviews that were published early on in the pandemic could be categorized as research waste. Even during public health emergencies, studies and systematic reviews should adhere to established methodological standards to provide patients, clinicians, and decision-makers trustworthy evidence.
Availability of data and materials
All data collected and analyzed within this study are available from the corresponding author on reasonable request.
World Health Organization. Timeline - COVID-19: Available at: https://www.who.int/news/item/29-06-2020-covidtimeline . Accessed 1 June 2021.
COVID-19 Dashboard by the Center for Systems Science and Engineering (CSSE) at Johns Hopkins University (JHU). Available at: https://coronavirus.jhu.edu/map.html . Accessed 1 June 2021.
Anzai A, Kobayashi T, Linton NM, Kinoshita R, Hayashi K, Suzuki A, et al. Assessing the Impact of Reduced Travel on Exportation Dynamics of Novel Coronavirus Infection (COVID-19). J Clin Med. 2020;9(2):601.
Chinazzi M, Davis JT, Ajelli M, Gioannini C, Litvinova M, Merler S, et al. The effect of travel restrictions on the spread of the 2019 novel coronavirus (COVID-19) outbreak. Science. 2020;368(6489):395–400. https://doi.org/10.1126/science.aba9757 .
Article CAS PubMed PubMed Central Google Scholar
Fidahic M, Nujic D, Runjic R, Civljak M, Markotic F, Lovric Makaric Z, et al. Research methodology and characteristics of journal articles with original data, preprint articles and registered clinical trial protocols about COVID-19. BMC Med Res Methodol. 2020;20(1):161. https://doi.org/10.1186/s12874-020-01047-2 .
EPPI Centre . COVID-19: a living systematic map of the evidence. Available at: http://eppi.ioe.ac.uk/cms/Projects/DepartmentofHealthandSocialCare/Publishedreviews/COVID-19Livingsystematicmapoftheevidence/tabid/3765/Default.aspx . Accessed 1 June 2021.
NCBI SARS-CoV-2 Resources. Available at: https://www.ncbi.nlm.nih.gov/sars-cov-2/ . Accessed 1 June 2021.
Gustot T. Quality and reproducibility during the COVID-19 pandemic. JHEP Rep. 2020;2(4):100141. https://doi.org/10.1016/j.jhepr.2020.100141 .
Article PubMed PubMed Central Google Scholar
Kodvanj, I., et al., Publishing of COVID-19 Preprints in Peer-reviewed Journals, Preprinting Trends, Public Discussion and Quality Issues. Preprint article. bioRxiv 2020.11.23.394577; doi: https://doi.org/10.1101/2020.11.23.394577 .
Dobler CC. Poor quality research and clinical practice during COVID-19. Breathe (Sheff). 2020;16(2):200112. https://doi.org/10.1183/20734735.0112-2020 .
Article Google Scholar
Bastian H, Glasziou P, Chalmers I. Seventy-five trials and eleven systematic reviews a day: how will we ever keep up? PLoS Med. 2010;7(9):e1000326. https://doi.org/10.1371/journal.pmed.1000326 .
Lunny C, Brennan SE, McDonald S, McKenzie JE. Toward a comprehensive evidence map of overview of systematic review methods: paper 1-purpose, eligibility, search and data extraction. Syst Rev. 2017;6(1):231. https://doi.org/10.1186/s13643-017-0617-1 .
Pollock M, Fernandes RM, Becker LA, Pieper D, Hartling L. Chapter V: Overviews of Reviews. In: Higgins JPT, Thomas J, Chandler J, Cumpston M, Li T, Page MJ, Welch VA (editors). Cochrane Handbook for Systematic Reviews of Interventions version 6.1 (updated September 2020). Cochrane. 2020. Available from www.training.cochrane.org/handbook .
Higgins JPT, Thomas J, Chandler J, Cumpston M, Li T, Page MJ, et al. Cochrane handbook for systematic reviews of interventions version 6.1 (updated September 2020). Cochrane. 2020; Available from www.training.cochrane.org/handbook .
Pollock M, Fernandes RM, Newton AS, Scott SD, Hartling L. The impact of different inclusion decisions on the comprehensiveness and complexity of overviews of reviews of healthcare interventions. Syst Rev. 2019;8(1):18. https://doi.org/10.1186/s13643-018-0914-3 .
Pollock M, Fernandes RM, Newton AS, Scott SD, Hartling L. A decision tool to help researchers make decisions about including systematic reviews in overviews of reviews of healthcare interventions. Syst Rev. 2019;8(1):29. https://doi.org/10.1186/s13643-018-0768-8 .
Hunt H, Pollock A, Campbell P, Estcourt L, Brunton G. An introduction to overviews of reviews: planning a relevant research question and objective for an overview. Syst Rev. 2018;7(1):39. https://doi.org/10.1186/s13643-018-0695-8 .
Pollock M, Fernandes RM, Pieper D, Tricco AC, Gates M, Gates A, et al. Preferred reporting items for overviews of reviews (PRIOR): a protocol for development of a reporting guideline for overviews of reviews of healthcare interventions. Syst Rev. 2019;8(1):335. https://doi.org/10.1186/s13643-019-1252-9 .
Moher D, Liberati A, Tetzlaff J, Altman DG, PRISMA Group. Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. Open Med. 2009;3(3):e123–30.
Krnic Martinic M, Pieper D, Glatt A, Puljak L. Definition of a systematic review used in overviews of systematic reviews, meta-epidemiological studies and textbooks. BMC Med Res Methodol. 2019;19(1):203. https://doi.org/10.1186/s12874-019-0855-0 .
Puljak L. If there is only one author or only one database was searched, a study should not be called a systematic review. J Clin Epidemiol. 2017;91:4–5. https://doi.org/10.1016/j.jclinepi.2017.08.002 .
Article PubMed Google Scholar
Gates M, Gates A, Guitard S, Pollock M, Hartling L. Guidance for overviews of reviews continues to accumulate, but important challenges remain: a scoping review. Syst Rev. 2020;9(1):254. https://doi.org/10.1186/s13643-020-01509-0 .
Covidence - systematic review software. Available at: https://www.covidence.org/ . Accessed 1 June 2021.
Shea BJ, Reeves BC, Wells G, Thuku M, Hamel C, Moran J, et al. AMSTAR 2: a critical appraisal tool for systematic reviews that include randomised or non-randomised studies of healthcare interventions, or both. BMJ. 2017;358:j4008.
Borges do Nascimento IJ, et al. Novel Coronavirus Infection (COVID-19) in Humans: A Scoping Review and Meta-Analysis. J Clin Med. 2020;9(4):941.
Article PubMed Central Google Scholar
Adhikari SP, Meng S, Wu YJ, Mao YP, Ye RX, Wang QZ, et al. Epidemiology, causes, clinical manifestation and diagnosis, prevention and control of coronavirus disease (COVID-19) during the early outbreak period: a scoping review. Infect Dis Poverty. 2020;9(1):29. https://doi.org/10.1186/s40249-020-00646-x .
Cortegiani A, Ingoglia G, Ippolito M, Giarratano A, Einav S. A systematic review on the efficacy and safety of chloroquine for the treatment of COVID-19. J Crit Care. 2020;57:279–83. https://doi.org/10.1016/j.jcrc.2020.03.005 .
Li B, Yang J, Zhao F, Zhi L, Wang X, Liu L, et al. Prevalence and impact of cardiovascular metabolic diseases on COVID-19 in China. Clin Res Cardiol. 2020;109(5):531–8. https://doi.org/10.1007/s00392-020-01626-9 .
Article CAS PubMed Google Scholar
Li LQ, Huang T, Wang YQ, Wang ZP, Liang Y, Huang TB, et al. COVID-19 patients’ clinical characteristics, discharge rate, and fatality rate of meta-analysis. J Med Virol. 2020;92(6):577–83. https://doi.org/10.1002/jmv.25757 .
Lippi G, Lavie CJ, Sanchis-Gomar F. Cardiac troponin I in patients with coronavirus disease 2019 (COVID-19): evidence from a meta-analysis. Prog Cardiovasc Dis. 2020;63(3):390–1. https://doi.org/10.1016/j.pcad.2020.03.001 .
Lippi G, Henry BM. Active smoking is not associated with severity of coronavirus disease 2019 (COVID-19). Eur J Intern Med. 2020;75:107–8. https://doi.org/10.1016/j.ejim.2020.03.014 .
Lippi G, Plebani M. Procalcitonin in patients with severe coronavirus disease 2019 (COVID-19): a meta-analysis. Clin Chim Acta. 2020;505:190–1. https://doi.org/10.1016/j.cca.2020.03.004 .
Lippi G, Plebani M, Henry BM. Thrombocytopenia is associated with severe coronavirus disease 2019 (COVID-19) infections: a meta-analysis. Clin Chim Acta. 2020;506:145–8. https://doi.org/10.1016/j.cca.2020.03.022 .
Ludvigsson JF. Systematic review of COVID-19 in children shows milder cases and a better prognosis than adults. Acta Paediatr. 2020;109(6):1088–95. https://doi.org/10.1111/apa.15270 .
Lupia T, Scabini S, Mornese Pinna S, di Perri G, de Rosa FG, Corcione S. 2019 novel coronavirus (2019-nCoV) outbreak: a new challenge. J Glob Antimicrob Resist. 2020;21:22–7. https://doi.org/10.1016/j.jgar.2020.02.021 .
Marasinghe, K.M., A systematic review investigating the effectiveness of face mask use in limiting the spread of COVID-19 among medically not diagnosed individuals: shedding light on current recommendations provided to individuals not medically diagnosed with COVID-19. Research Square. Preprint article. doi : https://doi.org/10.21203/rs.3.rs-16701/v1 . 2020 .
Mullins E, Evans D, Viner RM, O’Brien P, Morris E. Coronavirus in pregnancy and delivery: rapid review. Ultrasound Obstet Gynecol. 2020;55(5):586–92. https://doi.org/10.1002/uog.22014 .
Pang J, Wang MX, Ang IYH, Tan SHX, Lewis RF, Chen JIP, et al. Potential Rapid Diagnostics, Vaccine and Therapeutics for 2019 Novel coronavirus (2019-nCoV): a systematic review. J Clin Med. 2020;9(3):623.
Rodriguez-Morales AJ, Cardona-Ospina JA, Gutiérrez-Ocampo E, Villamizar-Peña R, Holguin-Rivera Y, Escalera-Antezana JP, et al. Clinical, laboratory and imaging features of COVID-19: a systematic review and meta-analysis. Travel Med Infect Dis. 2020;34:101623. https://doi.org/10.1016/j.tmaid.2020.101623 .
Salehi S, Abedi A, Balakrishnan S, Gholamrezanezhad A. Coronavirus disease 2019 (COVID-19): a systematic review of imaging findings in 919 patients. AJR Am J Roentgenol. 2020;215(1):87–93. https://doi.org/10.2214/AJR.20.23034 .
Sun P, Qie S, Liu Z, Ren J, Li K, Xi J. Clinical characteristics of hospitalized patients with SARS-CoV-2 infection: a single arm meta-analysis. J Med Virol. 2020;92(6):612–7. https://doi.org/10.1002/jmv.25735 .
Yang J, Zheng Y, Gou X, Pu K, Chen Z, Guo Q, et al. Prevalence of comorbidities and its effects in patients infected with SARS-CoV-2: a systematic review and meta-analysis. Int J Infect Dis. 2020;94:91–5. https://doi.org/10.1016/j.ijid.2020.03.017 .
Bassetti M, Vena A, Giacobbe DR. The novel Chinese coronavirus (2019-nCoV) infections: challenges for fighting the storm. Eur J Clin Investig. 2020;50(3):e13209. https://doi.org/10.1111/eci.13209 .
Article CAS Google Scholar
Hwang CS. Olfactory neuropathy in severe acute respiratory syndrome: report of a case. Acta Neurol Taiwanica. 2006;15(1):26–8.
Google Scholar
Suzuki M, Saito K, Min WP, Vladau C, Toida K, Itoh H, et al. Identification of viruses in patients with postviral olfactory dysfunction. Laryngoscope. 2007;117(2):272–7. https://doi.org/10.1097/01.mlg.0000249922.37381.1e .
Rajgor DD, Lee MH, Archuleta S, Bagdasarian N, Quek SC. The many estimates of the COVID-19 case fatality rate. Lancet Infect Dis. 2020;20(7):776–7. https://doi.org/10.1016/S1473-3099(20)30244-9 .
Wolkewitz M, Puljak L. Methodological challenges of analysing COVID-19 data during the pandemic. BMC Med Res Methodol. 2020;20(1):81. https://doi.org/10.1186/s12874-020-00972-6 .
Rombey T, Lochner V, Puljak L, Könsgen N, Mathes T, Pieper D. Epidemiology and reporting characteristics of non-Cochrane updates of systematic reviews: a cross-sectional study. Res Synth Methods. 2020;11(3):471–83. https://doi.org/10.1002/jrsm.1409 .
Runjic E, Rombey T, Pieper D, Puljak L. Half of systematic reviews about pain registered in PROSPERO were not published and the majority had inaccurate status. J Clin Epidemiol. 2019;116:114–21. https://doi.org/10.1016/j.jclinepi.2019.08.010 .
Runjic E, Behmen D, Pieper D, Mathes T, Tricco AC, Moher D, et al. Following Cochrane review protocols to completion 10 years later: a retrospective cohort study and author survey. J Clin Epidemiol. 2019;111:41–8. https://doi.org/10.1016/j.jclinepi.2019.03.006 .
Tricco AC, Antony J, Zarin W, Strifler L, Ghassemi M, Ivory J, et al. A scoping review of rapid review methods. BMC Med. 2015;13(1):224. https://doi.org/10.1186/s12916-015-0465-6 .
COVID-19 Rapid Reviews: Cochrane’s response so far. Available at: https://training.cochrane.org/resource/covid-19-rapid-reviews-cochrane-response-so-far . Accessed 1 June 2021.
Cochrane. Living systematic reviews. Available at: https://community.cochrane.org/review-production/production-resources/living-systematic-reviews . Accessed 1 June 2021.
Millard T, Synnot A, Elliott J, Green S, McDonald S, Turner T. Feasibility and acceptability of living systematic reviews: results from a mixed-methods evaluation. Syst Rev. 2019;8(1):325. https://doi.org/10.1186/s13643-019-1248-5 .
Babic A, Poklepovic Pericic T, Pieper D, Puljak L. How to decide whether a systematic review is stable and not in need of updating: analysis of Cochrane reviews. Res Synth Methods. 2020;11(6):884–90. https://doi.org/10.1002/jrsm.1451 .
Lovato A, Rossettini G, de Filippis C. Sore throat in COVID-19: comment on “clinical characteristics of hospitalized patients with SARS-CoV-2 infection: a single arm meta-analysis”. J Med Virol. 2020;92(7):714–5. https://doi.org/10.1002/jmv.25815 .
Leung C. Comment on Li et al: COVID-19 patients’ clinical characteristics, discharge rate, and fatality rate of meta-analysis. J Med Virol. 2020;92(9):1431–2. https://doi.org/10.1002/jmv.25912 .
Li LQ, Huang T, Wang YQ, Wang ZP, Liang Y, Huang TB, et al. Response to Char’s comment: comment on Li et al: COVID-19 patients’ clinical characteristics, discharge rate, and fatality rate of meta-analysis. J Med Virol. 2020;92(9):1433. https://doi.org/10.1002/jmv.25924 .
Download references
Acknowledgments
We thank Catherine Henderson DPhil from Swanscoe Communications for pro bono medical writing and editing support. We acknowledge support from the Covidence Team, specifically Anneliese Arno. We thank the whole International Network of Coronavirus Disease 2019 (InterNetCOVID-19) for their commitment and involvement. Members of the InterNetCOVID-19 are listed in Additional file 6 . We thank Pavel Cerny and Roger Crosthwaite for guiding the team supervisor (IJBN) on human resources management.
This research received no external funding.
Author information
Authors and affiliations.
University Hospital and School of Medicine, Universidade Federal de Minas Gerais, Belo Horizonte, Minas Gerais, Brazil
Israel Júnior Borges do Nascimento & Milena Soriano Marcolino
Medical College of Wisconsin, Milwaukee, WI, USA
Israel Júnior Borges do Nascimento
Helene Fuld Health Trust National Institute for Evidence-based Practice in Nursing and Healthcare, College of Nursing, The Ohio State University, Columbus, OH, USA
Dónal P. O’Mathúna
School of Nursing, Psychotherapy and Community Health, Dublin City University, Dublin, Ireland
Department of Anesthesiology, Intensive Care and Pain Medicine, University of Münster, Münster, Germany
Thilo Caspar von Groote
Department of Sport and Health Science, Technische Universität München, Munich, Germany
Hebatullah Mohamed Abdulazeem
School of Health Sciences, Faculty of Health and Medicine, The University of Newcastle, Callaghan, Australia
Ishanka Weerasekara
Department of Physiotherapy, Faculty of Allied Health Sciences, University of Peradeniya, Peradeniya, Sri Lanka
Cochrane Croatia, University of Split, School of Medicine, Split, Croatia
Ana Marusic, Irena Zakarija-Grkovic & Tina Poklepovic Pericic
Center for Evidence-Based Medicine and Health Care, Catholic University of Croatia, Ilica 242, 10000, Zagreb, Croatia
Livia Puljak
Cochrane Brazil, Evidence-Based Health Program, Universidade Federal de São Paulo, São Paulo, Brazil
Vinicius Tassoni Civile & Alvaro Nagib Atallah
Yorkville University, Fredericton, New Brunswick, Canada
Santino Filoso
Laboratory for Industrial and Applied Mathematics (LIAM), Department of Mathematics and Statistics, York University, Toronto, Ontario, Canada
Nicola Luigi Bragazzi
You can also search for this author in PubMed Google Scholar
Contributions
IJBN conceived the research idea and worked as a project coordinator. DPOM, TCVG, HMA, IW, AM, LP, VTC, IZG, TPP, ANA, SF, NLB and MSM were involved in data curation, formal analysis, investigation, methodology, and initial draft writing. All authors revised the manuscript critically for the content. The author(s) read and approved the final manuscript.
Corresponding author
Correspondence to Livia Puljak .
Ethics declarations
Ethics approval and consent to participate.
Not required as data was based on published studies.
Consent for publication
Not applicable.
Competing interests
The authors declare no conflict of interest.
Additional information
Publisher’s note.
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Additional file 1: appendix 1..
Search strategies used in the study.

Additional file 2: Appendix 2.
Adjusted scoring of AMSTAR 2 used in this study for systematic reviews of studies that did not analyze interventions.
Additional file 3: Appendix 3.
List of excluded studies, with reasons.
Additional file 4: Appendix 4.
Table of overlapping studies, containing the list of primary studies included, their visual overlap in individual systematic reviews, and the number in how many reviews each primary study was included.
Additional file 5: Appendix 5.
A detailed explanation of AMSTAR scoring for each item in each review.
Additional file 6: Appendix 6.
List of members and affiliates of International Network of Coronavirus Disease 2019 (InterNetCOVID-19).
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/ . The Creative Commons Public Domain Dedication waiver ( http://creativecommons.org/publicdomain/zero/1.0/ ) applies to the data made available in this article, unless otherwise stated in a credit line to the data.
Reprints and permissions
About this article
Cite this article.
Borges do Nascimento, I.J., O’Mathúna, D.P., von Groote, T.C. et al. Coronavirus disease (COVID-19) pandemic: an overview of systematic reviews. BMC Infect Dis 21 , 525 (2021). https://doi.org/10.1186/s12879-021-06214-4
Download citation
Received : 12 April 2020
Accepted : 19 May 2021
Published : 04 June 2021
DOI : https://doi.org/10.1186/s12879-021-06214-4
Share this article
Anyone you share the following link with will be able to read this content:
Sorry, a shareable link is not currently available for this article.
Provided by the Springer Nature SharedIt content-sharing initiative
- Coronavirus
- Evidence-based medicine
- Infectious diseases
BMC Infectious Diseases
ISSN: 1471-2334
- General enquiries: [email protected]
Now is the time for a 'great reset'

In every crisis, there is an opportunity Image: Space Uptopian/Unsplash
.chakra .wef-spn4bz{transition-property:var(--chakra-transition-property-common);transition-duration:var(--chakra-transition-duration-fast);transition-timing-function:var(--chakra-transition-easing-ease-out);cursor:pointer;text-decoration:none;outline:2px solid transparent;outline-offset:2px;color:inherit;}.chakra .wef-spn4bz:hover,.chakra .wef-spn4bz[data-hover]{text-decoration:underline;}.chakra .wef-spn4bz:focus-visible,.chakra .wef-spn4bz[data-focus-visible]{box-shadow:var(--chakra-shadows-outline);} Klaus Schwab
- Visit the Great Reset microsite here .
- Hear Klaus Schwab on these podcast episodes: the Great Reset launch and his book .
- We can emerge from this crisis a better world, if we act quickly and jointly, writes Schwab.
- The changes we have already seen in response to COVID-19 prove that a reset of our economic and social foundations is possible.
- This is our best chance to instigate stakeholder capitalism - and here's how it can be achieved.
COVID-19 lockdowns may be gradually easing, but anxiety about the world’s social and economic prospects is only intensifying. There is good reason to worry: a sharp economic downturn has already begun, and we could be facing the worst depression since the 1930s. But, while this outcome is likely, it is not unavoidable.
To achieve a better outcome, the world must act jointly and swiftly to revamp all aspects of our societies and economies, from education to social contracts and working conditions. Every country, from the United States to China, must participate, and every industry, from oil and gas to tech, must be transformed. In short, we need a “Great Reset” of capitalism.
Responding to the COVID-19 pandemic requires global cooperation among governments, international organizations and the business community , which is at the centre of the World Economic Forum’s mission as the International Organization for Public-Private Cooperation.
Since its launch on 11 March, the Forum’s COVID Action Platform has brought together 1,667 stakeholders from 1,106 businesses and organizations to mitigate the risk and impact of the unprecedented global health emergency that is COVID-19.
The platform is created with the support of the World Health Organization and is open to all businesses and industry groups, as well as other stakeholders, aiming to integrate and inform joint action.
As an organization, the Forum has a track record of supporting efforts to contain epidemics. In 2017, at our Annual Meeting, the Coalition for Epidemic Preparedness Innovations (CEPI) was launched – bringing together experts from government, business, health, academia and civil society to accelerate the development of vaccines. CEPI is currently supporting the race to develop a vaccine against this strand of the coronavirus.
There are many reasons to pursue a Great Reset, but the most urgent is COVID-19. Having already led to hundreds of thousands of deaths, the pandemic represents one of the worst public-health crises in recent history. And, with casualties still mounting in many parts of the world, it is far from over.
This will have serious long-term consequences for economic growth, public debt, employment, and human wellbeing. According to the Financial Times , global government debt has already reached its highest level in peacetime. Moreover, unemployment is skyrocketing in many countries: in the US, for example, one in four workers have filed for unemployment since mid-March, with new weekly claims far above historic highs. The International Monetary Fund expects the world economy to shrink by 3% this year – a downgrade of 6.3 percentage points in just four months.
All of this will exacerbate the climate and social crises that were already underway. Some countries have already used the COVID-19 crisis as an excuse to weaken environmental protections and enforcement. And frustrations over social ills like rising inequality – US billionaires’ combined wealth has increased during the crisis – are intensifying.
Have you read?
What risks does covid-19 pose to society in the long-term, covid-19 is a litmus test for stakeholder capitalism.
Left unaddressed, these crises, together with COVID-19, will deepen and leave the world even less sustainable, less equal, and more fragile. Incremental measures and ad hoc fixes will not suffice to prevent this scenario. We must build entirely new foundations for our economic and social systems.
The level of cooperation and ambition this implies is unprecedented. But it is not some impossible dream. In fact, one silver lining of the pandemic is that it has shown how quickly we can make radical changes to our lifestyles. Almost instantly, the crisis forced businesses and individuals to abandon practices long claimed to be essential, from frequent air travel to working in an office.
Likewise, populations have overwhelmingly shown a willingness to make sacrifices for the sake of health-care and other essential workers and vulnerable populations, such as the elderly. And many companies have stepped up to support their workers, customers, and local communities, in a shift toward the kind of stakeholder capitalism to which they had previously paid lip service .
Clearly, the will to build a better society does exist. We must use it to secure the Great Reset that we so badly need. That will require stronger and more effective governments, though this does not imply an ideological push for bigger ones. And it will demand private-sector engagement every step of the way.
The Great Reset agenda would have three main components. The first would steer the market toward fairer outcomes. To this end, governments should improve coordination (for example, in tax, regulatory, and fiscal policy), upgrade trade arrangements, and create the conditions for a “stakeholder economy.” At a time of diminishing tax bases and soaring public debt, governments have a powerful incentive to pursue such action.
Moreover, governments should implement long-overdue reforms that promote more equitable outcomes. Depending on the country, these may include changes to wealth taxes, the withdrawal of fossil-fuel subsidies, and new rules governing intellectual property, trade, and competition.
The second component of a Great Reset agenda would ensure that investments advance shared goals, such as equality and sustainability. Here, the large-scale spending programs that many governments are implementing represent a major opportunity for progress. The European Commission, for one, has unveiled plans for a €750 billion ($826 billion) recovery fund. The US, China, and Japan also have ambitious economic-stimulus plans.
Rather than using these funds, as well as investments from private entities and pension funds, to fill cracks in the old system, we should use them to create a new one that is more resilient, equitable, and sustainable in the long run. This means, for example, building “green” urban infrastructure and creating incentives for industries to improve their track record on environmental, social, and governance (ESG) metrics.
The third and final priority of a Great Reset agenda is to harness the innovations of the Fourth Industrial Revolution to support the public good, especially by addressing health and social challenges. During the COVID-19 crisis, companies, universities, and others have joined forces to develop diagnostics, therapeutics, and possible vaccines; establish testing centers; create mechanisms for tracing infections; and deliver telemedicine. Imagine what could be possible if similar concerted efforts were made in every sector.

The COVID-19 crisis is affecting every facet of people’s lives in every corner of the world. But tragedy need not be its only legacy. On the contrary, the pandemic represents a rare but narrow window of opportunity to reflect, reimagine, and reset our world to create a healthier, more equitable, and more prosperous future.

Don't miss any update on this topic
Create a free account and access your personalized content collection with our latest publications and analyses.
License and Republishing
World Economic Forum articles may be republished in accordance with the Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International Public License, and in accordance with our Terms of Use.
The views expressed in this article are those of the author alone and not the World Economic Forum.
Stay up to date:
Sustainable development, related topics:.

.chakra .wef-1v7zi92{margin-top:var(--chakra-space-base);margin-bottom:var(--chakra-space-base);line-height:var(--chakra-lineHeights-base);font-size:var(--chakra-fontSizes-larger);}@media screen and (min-width: 56.5rem){.chakra .wef-1v7zi92{font-size:var(--chakra-fontSizes-large);}} Explore and monitor how .chakra .wef-ugz4zj{margin-top:var(--chakra-space-base);margin-bottom:var(--chakra-space-base);line-height:var(--chakra-lineHeights-base);font-size:var(--chakra-fontSizes-larger);color:var(--chakra-colors-yellow);}@media screen and (min-width: 56.5rem){.chakra .wef-ugz4zj{font-size:var(--chakra-fontSizes-large);}} Sustainable Development is affecting economies, industries and global issues

.chakra .wef-19044xk{margin-top:var(--chakra-space-base);margin-bottom:var(--chakra-space-base);line-height:var(--chakra-lineHeights-base);color:var(--chakra-colors-uplinkBlue);font-size:var(--chakra-fontSizes-larger);}@media screen and (min-width: 56.5rem){.chakra .wef-19044xk{font-size:var(--chakra-fontSizes-large);}} Get involved with our crowdsourced digital platform to deliver impact at scale
The agenda .chakra .wef-dog8kz{margin-top:var(--chakra-space-base);margin-bottom:var(--chakra-space-base);line-height:var(--chakra-lineheights-base);font-weight:var(--chakra-fontweights-normal);} weekly.
A weekly update of the most important issues driving the global agenda
.chakra .wef-1dtnjt5{display:flex;align-items:center;flex-wrap:wrap;} More on Sustainable Development .chakra .wef-17xejub{flex:1;justify-self:stretch;align-self:stretch;} .chakra .wef-2sx2oi{display:inline-flex;vertical-align:middle;padding-inline-start:var(--chakra-space-1);padding-inline-end:var(--chakra-space-1);text-transform:uppercase;font-size:var(--chakra-fontSizes-smallest);border-radius:var(--chakra-radii-base);font-weight:var(--chakra-fontWeights-bold);background:none;box-shadow:var(--badge-shadow);align-items:center;line-height:var(--chakra-lineHeights-short);letter-spacing:1.25px;padding:var(--chakra-space-0);white-space:normal;color:var(--chakra-colors-greyLight);box-decoration-break:clone;-webkit-box-decoration-break:clone;}@media screen and (min-width: 37.5rem){.chakra .wef-2sx2oi{font-size:var(--chakra-fontSizes-smaller);}}@media screen and (min-width: 56.5rem){.chakra .wef-2sx2oi{font-size:var(--chakra-fontSizes-base);}} See all

How digital twins are transforming the world of water management
November 1, 2024

How public-private partnerships are creating more energy-efficient appliances in Japan

Can toys go green? Here's how 5 major companies plan to make their products nature positive

How geopolitics will both hinder and accelerate the global energy transition

How legislation can help boost renewable energy investments in Africa

Here's how to mobilize for Sustainable Development Goal 14 ahead of UN Ocean Conference 2025
The Essex website uses cookies. By continuing to browse the site you are consenting to their use. Please visit our cookie policy to find out which cookies we use and why. View cookie policy.
Thesis Submission Guidance: COVID-19 Impact Statement
In response to the impact of the global pandemic, we’re giving you the option to include a statement at the start of your thesis which outlines the effects that COVID-19 may have had on the research that you have undertaken towards your doctoral degree.
The inclusion of a statement is to facilitate the reader’s awareness, both now and in the future, that the pandemic may have had an effect on the scope, direction and presentation of the research.
The academic standards and quality threshold for the award remains unchanged. Where statements are included, you should be reassured that this is not evidencing a lack of original research or intellectual rigour.
If you decide to include one such statement, it should appear on the first page of the thesis, after the cover page, and be titled ‘Impact of COVID-19’. The statement should not exceed 1000 words and will not count towards the total thesis word count.
Examples of potential areas for consideration and comment when developing your impact statement are below. However, you should discuss the content of the statement with your supervisor before submission:
- Details on how disruption caused by COVID-19 has impacted the research (for example, an inability to conduct face to face research, an inability to collect/analyse data as a result of travel constraints, or restricted access to labs or other working spaces).
- A description of how the planned work would have fitted within the thesis narrative (e.g., through method development, expansion of analytical skills or advancement of hypotheses).
- A summary of any decisions / actions taken to mitigate for any work or data collection/analyses that were prevented by COVID-19.
- Highlighting new research questions and developments, emphasising the work that has been undertaken in pivoting or adjusting the project.
You are reminded of the public nature of the published thesis and the longevity of any such included statements about the impact of the pandemic. You are advised to take a cautious approach as to the insertion of any personal information in these statements.
- For enquiries contact your Student Services Hub
- University of Essex
- Wivenhoe Park
- Colchester CO4 3SQ
- Accessibility
- Privacy and Cookie Policy
Log in using your username and password
- Search More Search for this keyword Advanced search
- Latest content
- Current issue
- BMJ Journals More You are viewing from: Google Indexer
You are here
- Volume 76, Issue 2
- COVID-19 pandemic and its impact on social relationships and health
- Article Text
- Article info
- Citation Tools
- Rapid Responses
- Article metrics
- http://orcid.org/0000-0003-1512-4471 Emily Long 1 ,
- Susan Patterson 1 ,
- Karen Maxwell 1 ,
- Carolyn Blake 1 ,
- http://orcid.org/0000-0001-7342-4566 Raquel Bosó Pérez 1 ,
- Ruth Lewis 1 ,
- Mark McCann 1 ,
- Julie Riddell 1 ,
- Kathryn Skivington 1 ,
- Rachel Wilson-Lowe 1 ,
- http://orcid.org/0000-0002-4409-6601 Kirstin R Mitchell 2
- 1 MRC/CSO Social and Public Health Sciences Unit , University of Glasgow , Glasgow , UK
- 2 MRC/CSO Social and Public Health Sciences Unit, Institute of Health & Wellbeing , University of Glasgow , Glasgow , UK
- Correspondence to Dr Emily Long, MRC/CSO Social and Public Health Sciences Unit, University of Glasgow, Glasgow G3 7HR, UK; emily.long{at}glasgow.ac.uk
This essay examines key aspects of social relationships that were disrupted by the COVID-19 pandemic. It focuses explicitly on relational mechanisms of health and brings together theory and emerging evidence on the effects of the COVID-19 pandemic to make recommendations for future public health policy and recovery. We first provide an overview of the pandemic in the UK context, outlining the nature of the public health response. We then introduce four distinct domains of social relationships: social networks, social support, social interaction and intimacy, highlighting the mechanisms through which the pandemic and associated public health response drastically altered social interactions in each domain. Throughout the essay, the lens of health inequalities, and perspective of relationships as interconnecting elements in a broader system, is used to explore the varying impact of these disruptions. The essay concludes by providing recommendations for longer term recovery ensuring that the social relational cost of COVID-19 is adequately considered in efforts to rebuild.
- inequalities
Data availability statement
Data sharing not applicable as no data sets generated and/or analysed for this study. Data sharing not applicable as no data sets generated or analysed for this essay.
This is an open access article distributed in accordance with the Creative Commons Attribution 4.0 Unported (CC BY 4.0) license, which permits others to copy, redistribute, remix, transform and build upon this work for any purpose, provided the original work is properly cited, a link to the licence is given, and indication of whether changes were made. See: https://creativecommons.org/licenses/by/4.0/ .
https://doi.org/10.1136/jech-2021-216690
Statistics from Altmetric.com
Request permissions.
If you wish to reuse any or all of this article please use the link below which will take you to the Copyright Clearance Center’s RightsLink service. You will be able to get a quick price and instant permission to reuse the content in many different ways.
Introduction
Infectious disease pandemics, including SARS and COVID-19, demand intrapersonal behaviour change and present highly complex challenges for public health. 1 A pandemic of an airborne infection, spread easily through social contact, assails human relationships by drastically altering the ways through which humans interact. In this essay, we draw on theories of social relationships to examine specific ways in which relational mechanisms key to health and well-being were disrupted by the COVID-19 pandemic. Relational mechanisms refer to the processes between people that lead to change in health outcomes.
At the time of writing, the future surrounding COVID-19 was uncertain. Vaccine programmes were being rolled out in countries that could afford them, but new and more contagious variants of the virus were also being discovered. The recovery journey looked long, with continued disruption to social relationships. The social cost of COVID-19 was only just beginning to emerge, but the mental health impact was already considerable, 2 3 and the inequality of the health burden stark. 4 Knowledge of the epidemiology of COVID-19 accrued rapidly, but evidence of the most effective policy responses remained uncertain.
The initial response to COVID-19 in the UK was reactive and aimed at reducing mortality, with little time to consider the social implications, including for interpersonal and community relationships. The terminology of ‘social distancing’ quickly became entrenched both in public and policy discourse. This equation of physical distance with social distance was regrettable, since only physical proximity causes viral transmission, whereas many forms of social proximity (eg, conversations while walking outdoors) are minimal risk, and are crucial to maintaining relationships supportive of health and well-being.
The aim of this essay is to explore four key relational mechanisms that were impacted by the pandemic and associated restrictions: social networks, social support, social interaction and intimacy. We use relational theories and emerging research on the effects of the COVID-19 pandemic response to make three key recommendations: one regarding public health responses; and two regarding social recovery. Our understanding of these mechanisms stems from a ‘systems’ perspective which casts social relationships as interdependent elements within a connected whole. 5
Social networks
Social networks characterise the individuals and social connections that compose a system (such as a workplace, community or society). Social relationships range from spouses and partners, to coworkers, friends and acquaintances. They vary across many dimensions, including, for example, frequency of contact and emotional closeness. Social networks can be understood both in terms of the individuals and relationships that compose the network, as well as the overall network structure (eg, how many of your friends know each other).
Social networks show a tendency towards homophily, or a phenomenon of associating with individuals who are similar to self. 6 This is particularly true for ‘core’ network ties (eg, close friends), while more distant, sometimes called ‘weak’ ties tend to show more diversity. During the height of COVID-19 restrictions, face-to-face interactions were often reduced to core network members, such as partners, family members or, potentially, live-in roommates; some ‘weak’ ties were lost, and interactions became more limited to those closest. Given that peripheral, weaker social ties provide a diversity of resources, opinions and support, 7 COVID-19 likely resulted in networks that were smaller and more homogenous.
Such changes were not inevitable nor necessarily enduring, since social networks are also adaptive and responsive to change, in that a disruption to usual ways of interacting can be replaced by new ways of engaging (eg, Zoom). Yet, important inequalities exist, wherein networks and individual relationships within networks are not equally able to adapt to such changes. For example, individuals with a large number of newly established relationships (eg, university students) may have struggled to transfer these relationships online, resulting in lost contacts and a heightened risk of social isolation. This is consistent with research suggesting that young adults were the most likely to report a worsening of relationships during COVID-19, whereas older adults were the least likely to report a change. 8
Lastly, social connections give rise to emergent properties of social systems, 9 where a community-level phenomenon develops that cannot be attributed to any one member or portion of the network. For example, local area-based networks emerged due to geographic restrictions (eg, stay-at-home orders), resulting in increases in neighbourly support and local volunteering. 10 In fact, research suggests that relationships with neighbours displayed the largest net gain in ratings of relationship quality compared with a range of relationship types (eg, partner, colleague, friend). 8 Much of this was built from spontaneous individual interactions within local communities, which together contributed to the ‘community spirit’ that many experienced. 11 COVID-19 restrictions thus impacted the personal social networks and the structure of the larger networks within the society.
Social support
Social support, referring to the psychological and material resources provided through social interaction, is a critical mechanism through which social relationships benefit health. In fact, social support has been shown to be one of the most important resilience factors in the aftermath of stressful events. 12 In the context of COVID-19, the usual ways in which individuals interact and obtain social support have been severely disrupted.
One such disruption has been to opportunities for spontaneous social interactions. For example, conversations with colleagues in a break room offer an opportunity for socialising beyond one’s core social network, and these peripheral conversations can provide a form of social support. 13 14 A chance conversation may lead to advice helpful to coping with situations or seeking formal help. Thus, the absence of these spontaneous interactions may mean the reduction of indirect support-seeking opportunities. While direct support-seeking behaviour is more effective at eliciting support, it also requires significantly more effort and may be perceived as forceful and burdensome. 15 The shift to homeworking and closure of community venues reduced the number of opportunities for these spontaneous interactions to occur, and has, second, focused them locally. Consequently, individuals whose core networks are located elsewhere, or who live in communities where spontaneous interaction is less likely, have less opportunity to benefit from spontaneous in-person supportive interactions.
However, alongside this disruption, new opportunities to interact and obtain social support have arisen. The surge in community social support during the initial lockdown mirrored that often seen in response to adverse events (eg, natural disasters 16 ). COVID-19 restrictions that confined individuals to their local area also compelled them to focus their in-person efforts locally. Commentators on the initial lockdown in the UK remarked on extraordinary acts of generosity between individuals who belonged to the same community but were unknown to each other. However, research on adverse events also tells us that such community support is not necessarily maintained in the longer term. 16
Meanwhile, online forms of social support are not bound by geography, thus enabling interactions and social support to be received from a wider network of people. Formal online social support spaces (eg, support groups) existed well before COVID-19, but have vastly increased since. While online interactions can increase perceived social support, it is unclear whether remote communication technologies provide an effective substitute from in-person interaction during periods of social distancing. 17 18 It makes intuitive sense that the usefulness of online social support will vary by the type of support offered, degree of social interaction and ‘online communication skills’ of those taking part. Youth workers, for instance, have struggled to keep vulnerable youth engaged in online youth clubs, 19 despite others finding a positive association between amount of digital technology used by individuals during lockdown and perceived social support. 20 Other research has found that more frequent face-to-face contact and phone/video contact both related to lower levels of depression during the time period of March to August 2020, but the negative effect of a lack of contact was greater for those with higher levels of usual sociability. 21 Relatedly, important inequalities in social support exist, such that individuals who occupy more socially disadvantaged positions in society (eg, low socioeconomic status, older people) tend to have less access to social support, 22 potentially exacerbated by COVID-19.
Social and interactional norms
Interactional norms are key relational mechanisms which build trust, belonging and identity within and across groups in a system. Individuals in groups and societies apply meaning by ‘approving, arranging and redefining’ symbols of interaction. 23 A handshake, for instance, is a powerful symbol of trust and equality. Depending on context, not shaking hands may symbolise a failure to extend friendship, or a failure to reach agreement. The norms governing these symbols represent shared values and identity; and mutual understanding of these symbols enables individuals to achieve orderly interactions, establish supportive relationship accountability and connect socially. 24 25
Physical distancing measures to contain the spread of COVID-19 radically altered these norms of interaction, particularly those used to convey trust, affinity, empathy and respect (eg, hugging, physical comforting). 26 As epidemic waves rose and fell, the work to negotiate these norms required intense cognitive effort; previously taken-for-granted interactions were re-examined, factoring in current restriction levels, own and (assumed) others’ vulnerability and tolerance of risk. This created awkwardness, and uncertainty, for example, around how to bring closure to an in-person interaction or convey warmth. The instability in scripted ways of interacting created particular strain for individuals who already struggled to encode and decode interactions with others (eg, those who are deaf or have autism spectrum disorder); difficulties often intensified by mask wearing. 27
Large social gatherings—for example, weddings, school assemblies, sporting events—also present key opportunities for affirming and assimilating interactional norms, building cohesion and shared identity and facilitating cooperation across social groups. 28 Online ‘equivalents’ do not easily support ‘social-bonding’ activities such as singing and dancing, and rarely enable chance/spontaneous one-on-one conversations with peripheral/weaker network ties (see the Social networks section) which can help strengthen bonds across a larger network. The loss of large gatherings to celebrate rites of passage (eg, bar mitzvah, weddings) has additional relational costs since these events are performed by and for communities to reinforce belonging, and to assist in transitioning to new phases of life. 29 The loss of interaction with diverse others via community and large group gatherings also reduces intergroup contact, which may then tend towards more prejudiced outgroup attitudes. While online interaction can go some way to mimicking these interaction norms, there are key differences. A sense of anonymity, and lack of in-person emotional cues, tends to support norms of polarisation and aggression in expressing differences of opinion online. And while online platforms have potential to provide intergroup contact, the tendency of much social media to form homogeneous ‘echo chambers’ can serve to further reduce intergroup contact. 30 31
Intimacy relates to the feeling of emotional connection and closeness with other human beings. Emotional connection, through romantic, friendship or familial relationships, fulfils a basic human need 32 and strongly benefits health, including reduced stress levels, improved mental health, lowered blood pressure and reduced risk of heart disease. 32 33 Intimacy can be fostered through familiarity, feeling understood and feeling accepted by close others. 34
Intimacy via companionship and closeness is fundamental to mental well-being. Positively, the COVID-19 pandemic has offered opportunities for individuals to (re)connect and (re)strengthen close relationships within their household via quality time together, following closure of many usual external social activities. Research suggests that the first full UK lockdown period led to a net gain in the quality of steady relationships at a population level, 35 but amplified existing inequalities in relationship quality. 35 36 For some in single-person households, the absence of a companion became more conspicuous, leading to feelings of loneliness and lower mental well-being. 37 38 Additional pandemic-related relational strain 39 40 resulted, for some, in the initiation or intensification of domestic abuse. 41 42
Physical touch is another key aspect of intimacy, a fundamental human need crucial in maintaining and developing intimacy within close relationships. 34 Restrictions on social interactions severely restricted the number and range of people with whom physical affection was possible. The reduction in opportunity to give and receive affectionate physical touch was not experienced equally. Many of those living alone found themselves completely without physical contact for extended periods. The deprivation of physical touch is evidenced to take a heavy emotional toll. 43 Even in future, once physical expressions of affection can resume, new levels of anxiety over germs may introduce hesitancy into previously fluent blending of physical and verbal intimate social connections. 44
The pandemic also led to shifts in practices and norms around sexual relationship building and maintenance, as individuals adapted and sought alternative ways of enacting sexual intimacy. This too is important, given that intimate sexual activity has known benefits for health. 45 46 Given that social restrictions hinged on reducing household mixing, possibilities for partnered sexual activity were primarily guided by living arrangements. While those in cohabiting relationships could potentially continue as before, those who were single or in non-cohabiting relationships generally had restricted opportunities to maintain their sexual relationships. Pornography consumption and digital partners were reported to increase since lockdown. 47 However, online interactions are qualitatively different from in-person interactions and do not provide the same opportunities for physical intimacy.
Recommendations and conclusions
In the sections above we have outlined the ways in which COVID-19 has impacted social relationships, showing how relational mechanisms key to health have been undermined. While some of the damage might well self-repair after the pandemic, there are opportunities inherent in deliberative efforts to build back in ways that facilitate greater resilience in social and community relationships. We conclude by making three recommendations: one regarding public health responses to the pandemic; and two regarding social recovery.
Recommendation 1: explicitly count the relational cost of public health policies to control the pandemic
Effective handling of a pandemic recognises that social, economic and health concerns are intricately interwoven. It is clear that future research and policy attention must focus on the social consequences. As described above, policies which restrict physical mixing across households carry heavy and unequal relational costs. These include for individuals (eg, loss of intimate touch), dyads (eg, loss of warmth, comfort), networks (eg, restricted access to support) and communities (eg, loss of cohesion and identity). Such costs—and their unequal impact—should not be ignored in short-term efforts to control an epidemic. Some public health responses—restrictions on international holiday travel and highly efficient test and trace systems—have relatively small relational costs and should be prioritised. At a national level, an earlier move to proportionate restrictions, and investment in effective test and trace systems, may help prevent escalation of spread to the point where a national lockdown or tight restrictions became an inevitability. Where policies with relational costs are unavoidable, close attention should be paid to the unequal relational impact for those whose personal circumstances differ from normative assumptions of two adult families. This includes consideration of whether expectations are fair (eg, for those who live alone), whether restrictions on social events are equitable across age group, religious/ethnic groupings and social class, and also to ensure that the language promoted by such policies (eg, households; families) is not exclusionary. 48 49 Forethought to unequal impacts on social relationships should thus be integral to the work of epidemic preparedness teams.
Recommendation 2: intelligently balance online and offline ways of relating
A key ingredient for well-being is ‘getting together’ in a physical sense. This is fundamental to a human need for intimate touch, physical comfort, reinforcing interactional norms and providing practical support. Emerging evidence suggests that online ways of relating cannot simply replace physical interactions. But online interaction has many benefits and for some it offers connections that did not exist previously. In particular, online platforms provide new forms of support for those unable to access offline services because of mobility issues (eg, older people) or because they are geographically isolated from their support community (eg, lesbian, gay, bisexual, transgender and queer (LGBTQ) youth). Ultimately, multiple forms of online and offline social interactions are required to meet the needs of varying groups of people (eg, LGBTQ, older people). Future research and practice should aim to establish ways of using offline and online support in complementary and even synergistic ways, rather than veering between them as social restrictions expand and contract. Intelligent balancing of online and offline ways of relating also pertains to future policies on home and flexible working. A decision to switch to wholesale or obligatory homeworking should consider the risk to relational ‘group properties’ of the workplace community and their impact on employees’ well-being, focusing in particular on unequal impacts (eg, new vs established employees). Intelligent blending of online and in-person working is required to achieve flexibility while also nurturing supportive networks at work. Intelligent balance also implies strategies to build digital literacy and minimise digital exclusion, as well as coproducing solutions with intended beneficiaries.
Recommendation 3: build stronger and sustainable localised communities
In balancing offline and online ways of interacting, there is opportunity to capitalise on the potential for more localised, coherent communities due to scaled-down travel, homeworking and local focus that will ideally continue after restrictions end. There are potential economic benefits after the pandemic, such as increased trade as home workers use local resources (eg, coffee shops), but also relational benefits from stronger relationships around the orbit of the home and neighbourhood. Experience from previous crises shows that community volunteer efforts generated early on will wane over time in the absence of deliberate work to maintain them. Adequately funded partnerships between local government, third sector and community groups are required to sustain community assets that began as a direct response to the pandemic. Such partnerships could work to secure green spaces and indoor (non-commercial) meeting spaces that promote community interaction. Green spaces in particular provide a triple benefit in encouraging physical activity and mental health, as well as facilitating social bonding. 50 In building local communities, small community networks—that allow for diversity and break down ingroup/outgroup views—may be more helpful than the concept of ‘support bubbles’, which are exclusionary and less sustainable in the longer term. Rigorously designed intervention and evaluation—taking a systems approach—will be crucial in ensuring scale-up and sustainability.
The dramatic change to social interaction necessitated by efforts to control the spread of COVID-19 created stark challenges but also opportunities. Our essay highlights opportunities for learning, both to ensure the equity and humanity of physical restrictions, and to sustain the salutogenic effects of social relationships going forward. The starting point for capitalising on this learning is recognition of the disruption to relational mechanisms as a key part of the socioeconomic and health impact of the pandemic. In recovery planning, a general rule is that what is good for decreasing health inequalities (such as expanding social protection and public services and pursuing green inclusive growth strategies) 4 will also benefit relationships and safeguard relational mechanisms for future generations. Putting this into action will require political will.
Ethics statements
Patient consent for publication.
Not required.
- Office for National Statistics (ONS)
- Ford T , et al
- Riordan R ,
- Ford J , et al
- Glonti K , et al
- McPherson JM ,
- Smith-Lovin L
- Granovetter MS
- Fancourt D et al
- Stadtfeld C
- Office for Civil Society
- Cook J et al
- Rodriguez-Llanes JM ,
- Guha-Sapir D
- Patulny R et al
- Granovetter M
- Winkeler M ,
- Filipp S-H ,
- Kaniasty K ,
- de Terte I ,
- Guilaran J , et al
- Wright KB ,
- Martin J et al
- Gabbiadini A ,
- Baldissarri C ,
- Durante F , et al
- Sommerlad A ,
- Marston L ,
- Huntley J , et al
- Turner RJ ,
- Bicchieri C
- Brennan G et al
- Watson-Jones RE ,
- Amichai-Hamburger Y ,
- McKenna KYA
- Page-Gould E ,
- Aron A , et al
- Pietromonaco PR ,
- Timmerman GM
- Bradbury-Jones C ,
- Mikocka-Walus A ,
- Klas A , et al
- Marshall L ,
- Steptoe A ,
- Stanley SM ,
- Campbell AM
- ↵ (ONS), O.f.N.S., Domestic abuse during the coronavirus (COVID-19) pandemic, England and Wales . Available: https://www.ons.gov.uk/peoplepopulationandcommunity/crimeandjustice/articles/domesticabuseduringthecoronaviruscovid19pandemicenglandandwales/november2020
- Rosenberg M ,
- Hensel D , et al
- Banerjee D ,
- Bruner DW , et al
- Bavel JJV ,
- Baicker K ,
- Boggio PS , et al
- van Barneveld K ,
- Quinlan M ,
- Kriesler P , et al
- Mitchell R ,
- de Vries S , et al
Twitter @karenmaxSPHSU, @Mark_McCann, @Rwilsonlowe, @KMitchinGlasgow
Contributors EL and KM led on the manuscript conceptualisation, review and editing. SP, KM, CB, RBP, RL, MM, JR, KS and RW-L contributed to drafting and revising the article. All authors assisted in revising the final draft.
Funding The research reported in this publication was supported by the Medical Research Council (MC_UU_00022/1, MC_UU_00022/3) and the Chief Scientist Office (SPHSU11, SPHSU14). EL is also supported by MRC Skills Development Fellowship Award (MR/S015078/1). KS and MM are also supported by a Medical Research Council Strategic Award (MC_PC_13027).
Competing interests None declared.
Provenance and peer review Not commissioned; externally peer reviewed.
Read the full text or download the PDF:
Log in using your username and password
- Search More Search for this keyword Advanced search
- Latest content
- For authors
- Browse by collection
- BMJ Journals More You are viewing from: Google Indexer
You are here
- Volume 10, Issue 12
- Impact of the COVID-19 pandemic on mental health and well-being of communities: an exploratory qualitative study protocol
- Article Text
- Article info
- Citation Tools
- Rapid Responses
- Article metrics
- http://orcid.org/0000-0003-0180-0213 Anam Shahil Feroz 1 , 2 ,
- Naureen Akber Ali 3 ,
- Noshaba Akber Ali 1 ,
- Ridah Feroz 4 ,
- Salima Nazim Meghani 1 ,
- Sarah Saleem 1
- 1 Community Health Sciences , Aga Khan University , Karachi , Pakistan
- 2 Institute of Health Policy, Management and Evaluation , University of Toronto , Toronto , Ontario , Canada
- 3 School of Nursing and Midwifery , Aga Khan University , Karachi , Pakistan
- 4 Aga Khan University Institute for Educational Development , Karachi , Pakistan
- Correspondence to Ms Anam Shahil Feroz; anam.sahyl{at}gmail.com
Introduction The COVID-19 pandemic has certainly resulted in an increased level of anxiety and fear in communities in terms of disease management and infection spread. Due to fear and social stigma linked with COVID-19, many individuals in the community hide their disease and do not access healthcare facilities in a timely manner. In addition, with the widespread use of social media, rumours, myths and inaccurate information about the virus are spreading rapidly, leading to intensified irritability, fearfulness, insomnia, oppositional behaviours and somatic complaints. Considering the relevance of all these factors, we aim to explore the perceptions and attitudes of community members towards COVID-19 and its impact on their daily lives and mental well-being.
Methods and analysis This formative research will employ an exploratory qualitative research design using semistructured interviews and a purposive sampling approach. The data collection methods for this formative research will include indepth interviews with community members. The study will be conducted in the Karimabad Federal B Area and in the Garden (East and West) community settings in Karachi, Pakistan. The community members of these areas have been selected purposively for the interview. Study data will be analysed thematically using NVivo V.12 Plus software.
Ethics and dissemination Ethical approval for this study has been obtained from the Aga Khan University Ethical Review Committee (2020-4825-10599). The results of the study will be disseminated to the scientific community and to the research subjects participating in the study. The findings will help us explore the perceptions and attitudes of different community members towards the COVID-19 pandemic and its impact on their daily lives and mental well-being.
- mental health
- public health
This is an open access article distributed in accordance with the Creative Commons Attribution Non Commercial (CC BY-NC 4.0) license, which permits others to distribute, remix, adapt, build upon this work non-commercially, and license their derivative works on different terms, provided the original work is properly cited, appropriate credit is given, any changes made indicated, and the use is non-commercial. See: http://creativecommons.org/licenses/by-nc/4.0/ .
https://doi.org/10.1136/bmjopen-2020-041641
Statistics from Altmetric.com
Request permissions.
If you wish to reuse any or all of this article please use the link below which will take you to the Copyright Clearance Center’s RightsLink service. You will be able to get a quick price and instant permission to reuse the content in many different ways.
Strengths and limitations of this study
The mental health impact of the COVID-19 pandemic is likely to last much longer than the physical health impact, and this study is positioned well to explore the perceptions and attitudes of community members towards the pandemic and its impact on their daily lives and mental well-being.
This study will guide the development of context-specific innovative mental health programmes to support communities in the future.
One limitation is that to minimise the risk of infection all study respondents will be interviewed online over Zoom and hence the authors will not have the opportunity to build rapport with the respondents or obtain non-verbal cues during interviews.
The COVID-19 pandemic has affected almost 180 countries since it was first detected in Wuhan, China in December 2019. 1 2 The COVID-19 outbreak has been declared a public health emergency of international concern by the WHO. 3 The WHO estimates the global mortality to be about 3.4% 4 ; however, death rates vary between countries and across age groups. 5 In Pakistan, a total of 10 880 cases and 228 deaths due to COVID-19 infection have been reported to date. 6
The worldwide COVID-19 pandemic has not only incurred massive challenges to the global supply chains and healthcare systems but also has a detrimental effect on the overall health of individuals. 7 The pandemic has led to lockdowns and has created destructive impact on the societies at large. Most company employees, including daily wage workers, have been prohibited from going to their workplaces or have been asked to work from home, which has caused job-related insecurities and financial crises in the communities. 8 Educational institutions and training centres have also been closed, which resulted in children losing their routine of going to schools, studying and socialising with their peers. Delay in examinations is likewise a huge stressor for students. 8 Alongside this, parents have been struggling with creating a structured milieu for their children. 9 COVID-19 has hindered the normal routine life of every individual, be it children, teenagers, adults or the elderly. The crisis is engendering burden throughout populations and communities, particularly in developing countries such as Pakistan which face major challenges due to fragile healthcare systems and poor economic structures. 10
The COVID-19 pandemic has certainly resulted in an increased level of anxiety and fear in communities in terms of disease management and infection spread. 8 Further, the highly contagious nature of COVID-19 has also escalated confusion, fear and panic among community residents. Moreover, social distancing is often an unpleasant experience for community members and for patients as it adds to mental suffering, particularly in the local setting where get-togethers with friends and families are a major source of entertainment. 9 Recent studies also showed that individuals who are following social distancing rules experience loneliness, causing a substantial level of distress in the form of anxiety, stress, anger, misperception and post-traumatic stress symptoms. 8 11 Separation from family members, loss of autonomy, insecurity over disease status, inadequate supplies, inadequate information, financial loss, frustration, stigma and boredom are all major stressors that can create drastic impact on an individual’s life. 11 Due to fear and social stigma linked with COVID-19, many individuals in the community hide their disease and do not access healthcare facilities in a timely manner. 12 With the widespread use of social media, 13 rumours, myths and inaccurate information about COVID-19 are also spreading rapidly, not only among adults but are also carried on to children, leading to intensified irritability, fearfulness, insomnia, oppositional behaviours and somatic complaints. 9 The psychological symptoms associated with COVID-19 at the community level are also manifested as anxiety-driven panic buying, resulting in exhaustion of resources from the market. 14 Some level of panic also dwells in the community due to the unavailability of essential protective equipment, particularly masks and sanitisers. 15 Similarly, mental health issues, including depression, anxiety, panic attacks, psychotic symptoms and even suicide, were reported during the early severe acute respiratory syndrome outbreak. 16 17 COVID-19 is likely posing a similar risk throughout the world. 12
The fear of transmitting the disease or a family member falling ill is a probable mental function of human nature, but at some point the psychological fear of the disease generates more anxiety than the disease itself. Therefore, mental health problems are likely to increase among community residents during an epidemic situation. Considering the relevance of all these factors, we aim to explore the perceptions and attitudes towards COVID-19 among community residents and the impact of these perceptions and attitude on their daily lives and mental well-being.
Methods and analysis
Study design.
This study will employ an exploratory qualitative research design using semistructured interviews and a purposive sampling approach. The data collection methods for this formative research will include indepth interviews (IDIs) with community members. The IDIs aim to explore perceptions of community members towards COVID-19 and its impact on their mental well-being.
Study setting and study participants
The study will be conducted in two communities in Karachi City: Karimabad Federal B Area Block 3 Gulberg Town, and Garden East and Garden West. Karimabad is a neighbourhood in the Karachi Central District of Karachi, Pakistan, situated in the south of Gulberg Town bordering Liaquatabad, Gharibabad and Federal B Area. The population of this neighbourhood is predominantly Ismailis. People living here belong mostly to the middle class to the lower middle class. It is also known for its wholesale market of sports goods and stationery. Garden is an upmarket neighbourhood in the Karachi South District of Karachi, Pakistan, subdivided into two neighbourhoods: Garden East and Garden West. It is the residential area around the Karachi Zoological Gardens; hence, it is popularly known as the ‘Garden’ area. The population of Garden used to be primarily Ismailis and Goan Catholics but has seen an increasing number of Memons, Pashtuns and Baloch. These areas have been selected purposively because the few members of these communities are already known to one of the coinvestigators. The coinvestigator will serve as a gatekeeper for providing entrance to the community for the purpose of this study. Adult community members of different ages and both genders will be interviewed from both sites, as mentioned in table 1 . Interview participants will be selected following the eligibility criteria.
- View inline
Study participants for indepth interviews
IDIs with community members
We will conduct IDIs with community members to explore the perceptions and attitudes of community members towards COVID-19 and its effects on their daily lives and mental well-being. IDI participants will be identified via the community WhatsApp group, and will be invited for an interview via a WhatsApp message or email. Consent will be taken over email or WhatsApp before the interview begins, where they will agree that the interview can be audio-recorded and that written notes can be taken. The interviews will be conducted either in Urdu or in English language, and each interview will last around 40–50 min. Study participants will be assured that their information will remain confidential and that no identifying features will be mentioned on the transcript. The major themes will include a general discussion about participants’ knowledge and perceptions about the COVID-19 pandemic, perceptions on safety measures, and perceived challenges in the current situation and its impact on their mental well-being. We anticipate that 24–30 interviews will be conducted, but we will cease interviews once data saturation has been achieved. Data saturation is the point when no new themes emerge from the additional interviews. Data collection will occur concurrently with data analysis to determine data saturation point. The audio recordings will be transcribed by a transcriptionist within 24 hours of the interviews.
An interview guide for IDIs is shown in online supplemental annex 1 .
Supplemental material
Eligibility criteria.
The following are the criteria for inclusion and exclusion of study participants:
Inclusion criteria
Residents of Garden (East and West) and Karimabad Federal B Area of Karachi who have not contracted the disease.
Exclusion criteria
Those who refuse to participate in the study.
Those who have experienced COVID-19 and are undergoing treatment.
Those who are suspected for COVID-19 and have been isolated/quarantined.
Family members of COVID-19-positive cases.
Data collection procedure
A semistructured interview guide has been developed for community members. The initial questions on the guide will help to explore participants’ perceptions and attitudes towards COVID-19. Additional questions on the guide will assess the impact of these perceptions and attitude on the daily lives and mental health and well-being of community residents. All semistructured interviews will be conducted online via Zoom or WhatsApp. Interviews will be scheduled at the participant’s convenient day and time. Interviews are anticipated to begin on 1 December 2020.
Patient and public involvement
No patients were involved.
Data analysis
We will transcribe and translate collected data into English language by listening to the audio recordings in order to conduct a thematic analysis. NVivo V.12 Plus software will be used to import, organise and explore data for analysis. Two independent researchers will read the transcripts at various times to develop familiarity and clarification with the data. We will employ an iterative process which will help us to label data and generate new categories to identify emergent themes. The recorded text will be divided into shortened units and labelled as a ‘code’ without losing the main essence of the research study. Subsequently, codes will be analysed and merged into comparable categories. Lastly, the same categories will be grouped into subthemes and final themes. To ensure inter-rater reliability, two independent investigators will perform the coding, category creation and thematic analyses. Discrepancies between the two investigators will be resolved through consensus meetings to reduce researcher bias.
Ethics and dissemination
Study participants will be asked to provide informed, written consent prior to participation in the study. The informed consent form can be submitted by the participant via WhatsApp or email. Participants who are unable to write their names will be asked to provide a thumbprint to symbolise their consent to participate. Ethical approval for this study has been obtained from the Aga Khan University Ethical Review Committee (2020-4825-10599). The study results will be disseminated to the scientific community and to the research subjects participating in the study. The findings will help us explore the perceptions and attitudes of different community members towards the COVID-19 pandemic and its impact on their daily lives and mental well-being.
The findings of this study will help us to explore the perceptions and attitudes towards the COVID-19 pandemic and its impact on the daily lives and mental well-being of individuals in the community. Besides, an indepth understanding of the needs of the community will be identified, which will help us develop context-specific innovative mental health programmes to support communities in the future. The study will provide insights into how communities are managing their lives under such a difficult situation.
- World Health Organization
- Nielsen-Saines K , et al
- Worldometer
- Ebrahim SH ,
- Gozzer E , et al
- Snoswell CL ,
- Harding LE , et al
- Nargis Asad
- van Weel C ,
- Qidwai W , et al
- Brooks SK ,
- Webster RK ,
- Smith LE , et al
- Tripathy S ,
- Kar SK , et al
- Schwartz J ,
- Maunder R ,
Supplementary materials
Supplementary data.
This web only file has been produced by the BMJ Publishing Group from an electronic file supplied by the author(s) and has not been edited for content.
- Data supplement 1
ASF and NAA are joint first authors.
Contributors ASF and NAA conceived the study. ASF, NAA, RF, NA, SNM and SS contributed to the development of the study design and final protocols for sample selection and interviews. ASF and NAA contributed to writing the manuscript. All authors reviewed and approved the final version of the paper.
Funding The authors have not declared a specific grant for this research from any funding agency in the public, commercial or not-for-profit sectors.
Competing interests None declared.
Patient consent for publication Not required.
Provenance and peer review Not commissioned; externally peer reviewed
Supplemental material This content has been supplied by the author(s). It has not been vetted by BMJ Publishing Group Limited (BMJ) and may not have been peer-reviewed. Any opinions or recommendations discussed are solely those of the author(s) and are not endorsed by BMJ. BMJ disclaims all liability and responsibility arising from any reliance placed on the content. Where the content includes any translated material, BMJ does not warrant the accuracy and reliability of the translations (including but not limited to local regulations, clinical guidelines, terminology, drug names and drug dosages), and is not responsible for any error and/or omissions arising from translation and adaptation or otherwise.
Read the full text or download the PDF:
Click through the PLOS taxonomy to find articles in your field.
For more information about PLOS Subject Areas, click here .
Loading metrics
Open Access
Peer-reviewed
Research Article
The impact of COVID-19 pandemic on physical and mental health of Asians: A study of seven middle-income countries in Asia
Roles Conceptualization, Data curation, Formal analysis, Methodology, Project administration, Supervision, Validation, Visualization, Writing – original draft, Writing – review & editing
Affiliation Institute of Cognitive Neuroscience, Faculty of Education, Huaibei Normal University, Huaibei, China
Roles Conceptualization, Data curation, Formal analysis, Investigation, Methodology, Project administration, Validation, Visualization, Writing – original draft, Writing – review & editing
Affiliation College of Medicine, University of the Philippines, Manila, Philippines
Roles Conceptualization, Supervision, Visualization
Affiliation University Malaysia Sarawak (UNIMAS), Sarawak, Malaysia
Roles Conceptualization, Methodology, Supervision, Visualization, Writing – original draft, Writing – review & editing
Affiliation Department of Psychology, Zahedan Branch, Islamic Azad University, Zahedan, Iran
Roles Conceptualization, Investigation, Methodology, Supervision, Visualization
Affiliation College of Public Health Sciences, Chulalongkorn University, a member of Thailand One Health University Network (THOHUN), Bangkok, Thailand
Roles Conceptualization, Investigation, Methodology, Supervision, Visualization, Writing – original draft, Writing – review & editing
Affiliation Institute of Clinical Psychology, University of Karachi, Karachi, Pakistan
Affiliations Institute for Preventive Medicine and Public Health, Hanoi Medical University, Hanoi, Vietnam, Bloomberg School of Public Health, Johns Hopkins University, Baltimore, MD, United States of America
Roles Formal analysis, Investigation, Methodology, Supervision, Validation
Affiliation DHQ Hospital Jhelum, Jhelum, Pakistan
Roles Formal analysis, Investigation, Methodology, Supervision
Affiliation Institute for Global Health Innovations, Duy Tan University, Da Nang, Vietnam
Roles Investigation, Methodology, Project administration, Supervision, Validation
Affiliation Institute for Preventive Medicine and Public Health, Hanoi Medical University, Hanoi, Vietnam
Roles Data curation, Investigation, Methodology, Project administration, Supervision, Validation
Roles Investigation, Methodology, Supervision, Validation
Affiliation Faculty of Medicine, Duy Tan University, Da Nang, Vietnam
Roles Data curation, Investigation, Methodology, Supervision, Validation
Affiliation Department of Psychology, University of Sistan and Baluchestan, Zahedan, Iran
Affiliation Center of Excellence in Evidence-based Medicine, Nguyen Tat Thanh University, Ho Chi Minh City, Vietnam
Roles Data curation, Project administration, Validation
Affiliation Department of Psychological Medicine, Yong Loo Lin School of Medicine, National University of Singapore, Singapore, Singapore
Roles Formal analysis, Writing – original draft, Writing – review & editing
Affiliation Mood Disorders Psychopharmacology Unit, University Health Network, University of Toronto, Toronto, Canada
Roles Formal analysis, Validation, Writing – original draft, Writing – review & editing
Affiliation Department of Psychological Medicine, National University Health System, Singapore, Singapore
Roles Conceptualization, Formal analysis, Funding acquisition, Project administration, Supervision, Validation, Visualization, Writing – original draft, Writing – review & editing
* E-mail: [email protected]
Affiliation Institute for Health Innovation and Technology (iHealthtech), Yong Loo Lin School of Medicine, National University of Singapore, Singapore, Singapore
- [ ... ],
Roles Conceptualization, Investigation, Methodology, Supervision, Validation, Writing – original draft, Writing – review & editing
Affiliation Southeast Asia One Health University Network (SEAOHUN), Chiang Mai, Thailand
- [ view all ]
- [ view less ]
- Cuiyan Wang,
- Michael Tee,
- Ashley Edward Roy,
- Mohammad A. Fardin,
- Wandee Srichokchatchawan,
- Hina A. Habib,
- Bach X. Tran,
- Shahzad Hussain,
- Men T. Hoang,

- Published: February 11, 2021
- https://doi.org/10.1371/journal.pone.0246824
- Reader Comments
The coronavirus disease (COVID-19) pandemic has impacted the economy, livelihood, and physical and mental well-being of people worldwide. This study aimed to compare the mental health status during the pandemic in the general population of seven middle income countries (MICs) in Asia (China, Iran, Malaysia, Pakistan, Philippines, Thailand, and Vietnam). All the countries used the Impact of Event Scale–Revised (IES-R) and Depression, Anxiety and Stress Scale (DASS-21) to measure mental health. There were 4479 Asians completed the questionnaire with demographic characteristics, physical symptoms and health service utilization, contact history, knowledge and concern, precautionary measure, and rated their mental health with the IES-R and DASS-21. Descriptive statistics, One-Way analysis of variance (ANOVA), and linear regression were used to identify protective and risk factors associated with mental health parameters. There were significant differences in IES-R and DASS-21 scores between 7 MICs (p<0.05). Thailand had all the highest scores of IES-R, DASS-21 stress, anxiety, and depression scores whereas Vietnam had all the lowest scores. The risk factors for adverse mental health during the COVID-19 pandemic include age <30 years, high education background, single and separated status, discrimination by other countries and contact with people with COVID-19 (p<0.05). The protective factors for mental health include male gender, staying with children or more than 6 people in the same household, employment, confidence in doctors, high perceived likelihood of survival, and spending less time on health information (p<0.05). This comparative study among 7 MICs enhanced the understanding of metal health in the general population during the COVID-19 pandemic.
Citation: Wang C, Tee M, Roy AE, Fardin MA, Srichokchatchawan W, Habib HA, et al. (2021) The impact of COVID-19 pandemic on physical and mental health of Asians: A study of seven middle-income countries in Asia. PLoS ONE 16(2): e0246824. https://doi.org/10.1371/journal.pone.0246824
Editor: Tauqeer Hussain Mallhi, Jouf University, Kingdom of Saudi Arabia, SAUDI ARABIA
Received: October 17, 2020; Accepted: January 27, 2021; Published: February 11, 2021
Copyright: © 2021 Wang et al. This is an open access article distributed under the terms of the Creative Commons Attribution License , which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Data Availability: All relevant data are within the paper and its Supporting Information files.
Funding: This study has the following funding sources: 1. Author C.W, 1 grant, Huaibei Normal University, China. 2. Author R.H, 1 grant, National University of Singapore iHealthtech Other Operating Expenses (R-722-000-004-731) 3. Author B.X.T, 1 grant, Vingroup Innovation Foundation (VINIF) COVID research grant (VINIF.2020.Covid19.DA07) in Vietnam
Competing interests: The authors have declared that no competing interests exist.
Introduction
Emerging psychiatric conditions and mental well-being were identified as the tenth most frequent research topic during the COVID-19 pandemic [ 1 ]. A recent systematic review found that relatively high rates of symptoms of anxiety, depression, post-traumatic stress disorder and stress were reported in the general population and health care professionals during the COVID-19 pandemic globally [ 2 , 3 ]. Asia has a number of middle income countries (MICs) that face tremendous economic challenges and limited medical resources to maintain physical and mental well-being during the pandemic [ 4 ]. This extended to North America as well, with the sudden change in economic security during COVID-19 projected to increase suicide rates [ 5 ]. During the pandemic, the Asia Pacific Disaster Mental Health Network recommended to establish a mental health agenda for Asia [ 6 ]. It is therefore important to conduct research to assess psychiatric status of Asians living in MICs to develop capacity of various health systems to respond to COVID-19. Previous studies mainly focused on mental health of individual Asian countries during the pandemic without cross comparison [ 7 – 9 ].
With no prior comparative study found on physical and mental health of Asians living in MICs during the COVID-19 pandemic, this study aimed to investigate the impact of the pandemic on physical and mental health in 7 Asian MICs (China, Iran, Malaysia, Pakistan, Philippines, Thailand and Vietnam), identify differences among countries, understand their concerns and precautions toward COVID-19, as well as to identify protective and risk factors associated with mental health outcomes.
Methodology
Study design and study population.
This was a cross-sectional study that involved seven countries. The recruitment was conducted after COVID-19 became an epidemic in each country. To minimize risks of COVID-19 infection, a respondent-driven sampling strategy on recruiting the general public was utilized where new participants were electronically invited by existing study respondents rather than face-to-face interaction. The respondents completed the questionnaires through an online survey platform (‘SurveyStar’, Changsha Ranxing Science and Technology in China, SurveyMonkey in Philippines, and Google Forms in other countries).
Ethics approval
The study was approved by the Institutional Review Boards from each MIC, China (Huaibei Normal University of China, HBU-IRB-2020-001/002), Iran (Islamic Azad University, Protocol Number: IRB-2020-001), Malaysia (Universiti Malaysia Sarawak, UNIMAS/NC-21.02/03-02 Jld.4 (85)), Pakistan (University of Karachi Protocol Number: ICP-1 (101) 2698), Philippines (University of Philippines Manila Research Ethics Board, UPMREB 2020-198-01), Thailand (Chulalongkorn University, COA No. 147/2563), and Vietnam (Hanoi Medical University, QD 75/QD-YHDP&YHDP). All IRBs allowed participants aged 12 years to 17 years to participate in this study and provide their own consent because the online survey did not pose any risk to research participants. All respondents provided informed consent. Confidentiality was maintained because no personally identifiable information was collected.
Measures and instruments
The COVID-19 online questionnaire designed by the National University of Singapore [ 10 ] had five sections: demographic, physical symptoms related to COVID-19 in the past 14 days, knowledge and concerns about COVID-19, precautionary measures against COVID, and views of health information required. Psychometric properties of the questionnaire were established in the initial phase and peak of the COVID-19 epidemic [ 8 , 9 ].
The psychological impact of COVID-19 was measured using the well-validated Impact of Event Scale-Revised (IES-R) in the Asians for determining the extent of psychological impact after exposure to a traumatic event (i.e., the COVID-19 pandemic) within one week of exposure [ 11 – 14 ]. In this study, the Cronbach’s alpha for different versions of IES-R is very high in all countries and ranges from 0.912–0.950. Cronbach’s alpha of 0.70 or higher in measuring the internal consistency is considered “acceptable” in most social science research [ 15 ].
The mental health status of respondents was measured using the Depression, Anxiety and Stress Scale (DASS-21) [ 16 ], which has been used to assess mental health in Asians [ 17 , 18 ]. Furthermore, DASS-21 assessed three domains (i.e. anxiety, depression and stress) and its psychometric properties was validated across clinical and non-clinical samples in different cultures and languages during the COVID-19 pandemic [ 19 ]. In this study, the Cronbach’s alpha (internal consistency) for different versions of DASS-21 is as follows: stress scale ranges from 0.839–0.934, anxiety scale ranges from 0.784–0.914, and depression scale ranges from 0.878–0.943. The IES-R and DASS-21 scales were previously used in research related to the COVID-19 epidemic [ 8 , 12 , 20 , 21 ]. The DASS and IES-R questionnaires are available in the public domain, and so permission is not required to use these two questionnaires [ 22 , 23 ].
Statistical analysis
Descriptive statistics were calculated to compare demographic characteristics, physical symptoms and health service utilization, contact history, knowledge and concern, precautionary measure and additional health information variables among 7 MICs. One-Way analysis of variance (ANOVA) was calculated to compare the mean IES-R and DASS-21 scores between 7 MICs in order to determine whether the associated population mean IES-R or DASS-21 scores were significantly different. If there were significant differences among 7 MICs, the Least Significant Difference (LSD) would calculate the smallest significant between mean scores of two countries with different combinations. Any difference larger than the LSD is considered a significant result. We used linear regressions to calculate the univariate associations between independent and dependent variables including the IES-S score and DASS-21 stress, anxiety and depression subscale scores for all respondents separately. All tests were two-tailed, with a significance level of p <0.05. Statistical analysis was performed on IBM SPSS Statistics version 21.0.
A total of 4479 participants from 7 MICs in Asia completed the survey. The distribution of the number of participants by country is listed as follows: China (27%), Philippines (19%), Malaysia (16.2%), Iran (12.3%), Thailand (11.6%), Pakistan (11.3%), and Vietnam (2.7%). Fig 1 compares the IES-R and DASS-21 scores amongst all 7 MICs in Asia.
- PPT PowerPoint slide
- PNG larger image
- TIFF original image
https://doi.org/10.1371/journal.pone.0246824.g001
The top three countries with highest IES-R scores were Thailand (mean 42.35, SD 13.39), China (mean 32.98, SD 15.42), and Iran (mean 30.42, SD 15.82). The top three countries with highest DASS-21 stress scores were Thailand (mean 21.94, SD 7.74), Pakistan (mean 14.02, SD 11.53) and Philippines (mean 10.60, SD 8.01). The top three countries with highest DASS-21 anxiety scores were Thailand (mean 18.66, SD 5.98), Pakistan (mean 8.23, SD 9.69) and Malaysia (mean 7.80, SD 10.95). The top three countries with highest DASS-21 depression scores were Thailand (mean 19.74, SD 6.99), Pakistan (mean 11.33, SD 11.28) and Philippines (mean 9.72, SD 8.99).
Differences in IES-R scores and DASS-21 stress, anxiety, depression scores amongst the 7 MICs were all statistically significant (IES-R: F(6, 4472) = 144.47, p<0.001, η2 = 0.16; Stress: F(6,4472) = 167.49 p<0.001, η2 = 0.18; Anxiety: F (6,4471) = 172.03, p<0.001, η2 = 0.19; Depression: F(6, 4472) = 137.11, p<0.001, η2 = 0.16). Vietnam had the lowest scores of IES-R (mean 17.39, SD 13.72), stress (mean 3.80, SD 5.81), anxiety (mean 2.10, SD 4.91) and depression (mean 2.28, SD 5.43). The LSD analysis revealed that the scores of Vietnam were significantly lower than the other countries (p<0.05).
S1 Table compares the demographics of 7 MICs. More than half of participants were women in all countries (Range: 52.6% in Pakistan to 76.8% in Thailand). More than half of Chinese, Filipino, Iranian and Pakistani participants were below age of 31 years. Majority of Chinese, Vietnamese and Malaysian respondents were married while majority of Filipino and Thai respondents were single. Majority of Filipino, Iranian, Pakistani, Malaysian and Thai respondents did not have children. More than half of participants stayed in a household with more than 3–5 people across all countries except Pakistan (49%). Majority of respondents from Philippines, Pakistan, Vietnam and Malaysia were employed when the study was conducted.
Table 1 shows the association between demographic characteristics of all participants and mental health parameters. Demographic characteristics associated with lower psychological impact were male gender whereas age younger than 30 years and students were associated with higher psychological impact. Participants who have children were associated with lower stress, anxiety and depression whereas participants with higher education, single and separated status were associated with higher stress, anxiety and depression. Staying with 6 or more people and those who were employed were associated with lower anxiety and depression.
https://doi.org/10.1371/journal.pone.0246824.t001
S2 Table shows the frequency of physical symptoms that resemble COVID-19 infection and there were significant differences among all countries. During the COVID-19 pandemic, the most common physical symptoms reported by general population in the 7 countries were headache (23.13%), cough (21.86%) and sore throat (19.29%). About 8.13% of respondents consulted General Practitioner (GP); 2.69% were hospitalized; 3.89% were tested positive for COVID-19 and 57.1% had a health insurance. Pakistani had the significantly highest proportion of respondents consulted GP (27.5%), hospitalized (16.4%), receiving COVID-19 test (17.2%) and being isolated (17.8%). Table 2 shows the association between physical symptoms and mental health outcomes. The physical symptoms that were significantly associated with higher scores in all mental health outcomes (IES-R and DASS-21 subscales) including rhinitis and persistent fever with cough or breathing difficulties. Chills or rigors, headache and nausea or vomiting were associated with higher DASS-21 stress and anxiety scores. Myalgia, cough, dizziness and sore throat were associated with higher score of IES-R. Usage of medical services such as seeing a doctor, hospitalization, recent COVID-19 testing, quarantine, poor rating of health status that were significantly associated with higher scores in all mental health outcomes (IES-R and DASS-21 subscales). History of chronic illness were significantly associated with higher DASS-21 subscale scores. Having medical insurance coverage was associated with higher IES-R scores.
https://doi.org/10.1371/journal.pone.0246824.t002
S3 Table shows the belief of route of transmission among participants in 7 MICs and there were significant differences among all countries. Out of all participants, there were a small number of participants who did not agree with transmission of COVID-19 being via droplets (10.34%) and contaminated objects (17.21%). It is interesting to note that China (60.5%) and Vietnam (59.8%) demonstrated significantly higher percentage of participants who believed in airborne transmission compared to .64.76% of participants from the other five countries who did not agree that COVID-19 was airborne transmitted.
Participants expressing confident and very confident in their doctors diagnosing COVID-19 were very high in Malaysia (93.8%) and China (92.9%); level of confidence was much lower in Iran (65.5%) and Pakistan (62.6%). About 50.26% of participants reported that they were likely and very likely to contract COVID-19, with Malaysian participants demonstrating the highest perceived risk of COVID-19 (72.8%) whilst the Filipino demonstrated the highest proportion of participants believing that they would not contract COVID-19 (53.2%). About 89.8% of Thai participants believed that they would survive if contracted with COVID-19 while the Pakistani had the highest proportion who believed that they would not survive COVID-19 (15.4%). About 78.43% of participants were satisfied with health information related to COVID-19; Vietnamese participants reported the highest proportion of satisfaction (97.5%). About 77.38% of participants were worried their family members contracting COVID-19. Pakistani participants reported the highest proportion of people who faced discrimination (42.7%). About 44.68% of participants spent more than 2 hours per day to view information on COVID-19 with Filipino participants having the highest proportion for spending more than 2 hours per day to view information (47.2%).
Table 3 shows the association between knowledge and concerns related to COVID-19 and mental health parameters. Agreement with airborne, contact with contaminated objects and droplet transmission was associated with higher DASS-21 in all subscales. Likelihood of contracting COVID-19, discrimination against by other countries and contact with people infected with COVID-19 were associated with higher IES-R or DASS-21 scores. Confidence in one’s own doctor diagnosing COVID-19, high likelihood of survival if infected with COVID-19 and spent less than two hours per day to monitor information relating to COVID-19 were associated with lower level of IES-R or DASS-21 scores.
https://doi.org/10.1371/journal.pone.0246824.t003
S4 Table shows the prevalence of precautionary measures and there were significant differences among 7 MICs (p<0.001). High percentages were reported by participants covering their mouth and nose after sneezing (98.0%), avoided sharing utensils (90.8%), practised hand hygiene (98.9%), washed hand after touching contaminated objects (96.2%), and wear face masks (93.5%). All Vietnamese participants (100%) responded wearing a face mask. About 68% of respondents felt that people were too worried about COVID-19 with Malaysia (90.5%), Thailand (90.5%) and Pakistan (86.6%) as the top three countries. Approximately 53% of respondents spent 20–24 hours per day at home; with China (84.7%), Iran (73.5%) and Philippines (55%) as the top three countries.
Table 4 shows the association between precautionary measures related to COVID-19 and mental health parameters. Avoidance of sharing cutlery dealing meals was associated with higher anxiety and depression. In contrast, hand hygiene practice was associated with lower IES-R and DASS-21 in all subscales. Wearing a face mask was associated with lower levels of stress and depression. Worries about COVID-19 was associated with significantly higher levels of DASS-21 in all subscales. Shorter duration of homestay was associated with higher levels of anxiety, depression and stress as compared to those who stayed at home for 20–24 hours per day.
https://doi.org/10.1371/journal.pone.0246824.t004
S5 Table compares the health information needs of participants from 7 MICs and there were significant differences among 7 MICs. The Chinese had the highest proportion who wanted to understand the symptoms of COVID-19 (91.6%), the prevention method (93.7%), effectiveness of drugs and vaccines (94.1%), number of infected cases and location (95.9%), travel advice (96.9%), mode of transmission (94.5%), required regular information update (92.7%) and personalized information (96.8%). The Iranians had the highest proportion who sought advices regarding treatment methods (90.4%) and Malaysians had the highest proportion who wanted to understand local outbreaks (94.2%).
Table 5 shows the association between health information needs about COVID-19 and mental health parameters. Most additional information including information on COVID-19 symptoms, prevention, treatment advice, needs for regular updates, knowledge on local transmission, effectiveness on drugs and vaccines, number of infected people based on geographical locations, travel advice and transmission mode of COVID were associated with higher IES-R scores. In contrast, the need for more personalized information, information on the effectiveness of drugs and vaccines, travel advices, transmission mode were associated with significantly lower level of depression.
https://doi.org/10.1371/journal.pone.0246824.t005
The main findings of this first multinational population-based study in MICs in Asia during the COVID-19 pandemic are summarized as follows. First, Thai respondents reported the highest levels of IES-R and DASS-21 scores. Second, Pakistani respondents reported the second highest levels of DASS-21 scores. Comparatively, Vietnamese respondents reported the lowest levels in DASS-21 scores. Third, Iranian respondents demonstrated the lowest confidence in their doctors whilst Pakistani respondents had the highest proportion who believed they would not survive COVID-19 and reported discrimination.
Assessing COVID-19’s association with respondents’ mental health, the three most common physical symptoms associated with adverse mental health were headache, cough and sore throat. Risk factors associated with adverse mental health during the COVID-19 pandemic include age <30 years old, high education background, single and separated status, discrimination by other countries, contact with people with COVID-19 and worries about COVID-19. Protective factors for mental health during the COVID-19 pandemic include male gender, staying with children, staying with 6 or more people, employment, confidence in own’s doctors diagnosing COVID-19, high perceived likelihood of surviving COVID-19, spending less time on health information, hand hygiene practice and wearing a face mask. Importantly, these findings will be significantly helpful for healthcare administrators in Asia at the national and local community levels [ 24 ] when preparing for the next wave of COVID-19 outbreak and future pandemics [ 25 ].
Iran had the highest total reported COVID cases (386,658) and number of COVID cases per 1 million people (4,593), as well as the highest number of deaths from COVID (22,293) and deaths per 1 million people (265) [ 26 ]. Pakistan had the second highest number of cases (298,509) and deaths (6,342) [ 26 ]. Of the 7 MICs, Vietnam had the lowest total numbers and rates across all seven countries, with 1,049 reported cases, 35 deaths and rates of just 11 cases and 0.4 deaths per 1 million [ 26 ]. As a result, Vietnamese respondents reported the lowest IES-R and DASS-21 scores. Vietnam has adopted several strategies to combat COVID-19 including development of the action plan and response strategies to optimize the utilization of human resources and equipment [ 24 ]; address the health information needs based on the diverse socioeconomic, demographic, and ethnic factors [ 27 ]; re-design communication activities for a more effective dissemination of information related to the epidemic [ 28 ]; safeguarding the health of workforce [ 29 ] to ensure minimal impact on economy and involvement of the grassroot system and village health collaborators to combat pandemics [ 30 , 31 ].
Thailand recorded the second lowest number of total cases (3,444) and deaths (58), and similarly the second lowest case rates (49) and death rates (0.8) per 1 million [ 26 ]. Surprisingly, we found that Thailand was the country with the highest IES-R and DASS-21 depression scores. This could be due to the impact of COVID-19 on the economy in Thailand. Among all MICs in Asia, the disruption on COVID-19 pandemic is the most severe on Thailand economy, due to its reliance on tourism as compared to other MICs. For 2020, the International Monetary Fund has predicted Thailand’s GDP to be reduced by 6.7 percent which is highest among Asian countries [ 32 ]. Pakistan ranked second in terms of DASS-21 scores and number of COVID cases and deaths. The congruence between psychological parameters and epidemiology of COVID-19 in Pakistan was due to poor sanitation, lack of basic preventive measures, lack of proper testing and medical facilities. Pakistani health professionals started protesting and threatened to quit work due to lack of Personal Protective Equipment (PPE) [ 33 ]. Currently, the vaccination coverage in rural Pakistan remains unsatisfactory amid various barriers including price, hesitancy, and low level of awareness [ 34 ]. Eid-ul-Adha is an annual religious festival that could not be cancelled due to religious obligations and led to a sharp spike in COVID-19 cases [ 35 ]. The unpreparedness and contradictory policies resulted in an alarming high rate of COVID-19 spread and worsening mental health and discrimination faced by Pakistani people. Iranian respondents demonstrated lowest confidence in their doctors. The economic sanctions that prevented medical supplies, equipment and drugs from arriving in Iran could lead to low confidence among Iranians [ 36 ].
This study highlighted unique protective factors for mental health in MICs of Asia. In this study, more than 90% of respondents agreed to wear masks to prevent COVID-19. During the initial stage of COVID-19 pandemic, medical and public health experts from the US and some European countries believed that there was no direct evidence of airborne transmission of COVID-19 [ 37 ]. In contrast, respiratory clinicians and public health experts from Asia argued that lack of evidence does not equate to evidence of ineffectiveness of face masks [ 38 ]. The use of face masks by Asians have played an important role in controlling the spread of COVID-19 [ 39 ]. This study showed the association between the use of face mask and lower DASS-21 anxiety and depression scores. This finding might support the postulation that wearing face mask could offer psychological benefits, such as feeling less vulnerable to infection via perceived control [ 37 ]. Staying with children and more than 6 people in the same household were protective factors due to the values of family support among Asians. Compared with western countries, family support has a greater influence on reducing the risk of adverse mental health in Asia [ 10 ].
The findings of this first multinational study have several implications for health and government policies. Firstly, the health authorities should offer psychological interventions to the general population who are at higher risk of developing adverse mental health including women, people younger than 30 years and single and separated status. High education background is a risk factor and online psychological interventions such as cognitive behaviour therapy (CBT) and mindfulness-based therapy could improve mental health for highly educated individual [ 40 ]. For countries with high IES-R scores (Thailand, China and Iran), online trauma-focused CBT that promotes trauma narration, problem solving related to problems associated with COVID-19 and home based relaxation could be helpful in reducing psychological impact [ 9 ]. Second, as physical symptoms resembling COVID-19 infection (e.g., rhinitis, persistent fever with cough, breathing difficulties) were associated with high IES-R and DASS-21 scores groups. There is an urgent need to develop accurate, rapid diagnostic tests in general practitioners’ clinics, community and rural settings [ 31 ]. A negative COVID-19 test result may alleviate anxiety, depression, stress and psychological impact. Enhancing the capacity of health system to combat COVID-19 may increase the confidence of public and improve mental health. Third, based on our findings, the WHO, governments and health authorities should provide regular updates on the effectiveness of vaccines and treatment methods. Mis-information related to the cause of COVID-19 [ 41 ], rumours [ 42 ] and inconsistent information [ 43 ] on COVID-19 symptoms, prevention, treatment and transmission mode were associated with negative psychological impact. Local governments, news agencies, professional and advocacy organisations should all provide health information and advices related to COVID-19 that are consistent with national guidelines and avoid mis-information [ 44 ]. It is important to identify group-specific demands would be helpful to provide proper information related to COVID-19 to fulfil the need of different population groups [ 27 ]. Various governments should offer relief packages to safeguard employment and economy to protect mental health. Additionally, the level of policy stringency in response to COVID-19 or pandemics, as measured by the Oxford Stringency Index, may influence mental health and should be moderated accordingly by respective governments [ 45 ].
This study has several limitations. First, the findings of this study were based on seven MICs in Asia and could not be generated to other countries. The study population had different sociodemographic characteristics as compared to the general population in the world due to sampling bias because only participants with Internet access could participate in this online survey. The respondent sampling method also compromised the representativeness of samples. The study population was female predominant (proportion of female in the study population: 67.76%; world population 49.58%) [ 46 ] and a high proportion of the study population possessed a university degree (85.6%). Thus, there is a potential risk of sampling bias because we could not reach out to potential respondents without Internet access. The second limitation was the cross-sectional nature of this study and inability to demonstrate cause and effect relationship. The third limitation was that we did not record demographic data regarding pre-existing mental illness of the study participants. The fourth limitation is that self-reported levels of psychological impact, anxiety, depression and stress may not always be aligned with objective assessment by mental health professionals. Nevertheless, psychological impact, anxiety, depression and stress are based on personal feelings, and self-reporting was paramount during the COVID-19 pandemic. The fifth limitation is that we did not study other aspects of the pandemic such as the potential threat of self-medication of hydroxychloroquine and cholorquine [ 47 ] and precautionary measures of walkthrough sanitization gates [ 48 ]. Lastly, we were unable to calculate the response rate. For potential respondents who were not keen to participate in the online survey, no response was recorded, and we could not collect any information from them.
Conclusions
In conclusion, this multi-national study across 7 MICs in Asia showed that Thai reported the highest mean IES-R and DASS-21 anxiety, depression and stress scores. In contrast, Vietnamese reported the lowest mean scores in IES-R and DASS-21 anxiety, depression and stress scales. The risk factors for adverse mental health include age < 30 years, high education background, single and separated status, discrimination by other countries, contact with people with COVID-19 and worries about COVID-19. The protective factors for mental health include male gender, staying with children, staying with 6 or more people, employment, confidence in own’s doctors diagnosing COVID-19, high perceived likelihood of surviving COVID-19, spending less time on health information, hand hygiene practice and wearing a face mask.
Supporting information
S1 table. comparison of demographics of the participants from seven countries..
https://doi.org/10.1371/journal.pone.0246824.s001
S2 Table. Physical symptoms resembling COVID-19 infection reported by the participants from seven countries.
https://doi.org/10.1371/journal.pone.0246824.s002
S3 Table. Comparison of knowledge related to COVID-19 in participants of the seven countries.
https://doi.org/10.1371/journal.pone.0246824.s003
S4 Table. Comparison of precautionary measures related to COVID-19 in the participants of the seven countries.
https://doi.org/10.1371/journal.pone.0246824.s004
S5 Table. Comparison of information needs about COVID-19 in the participants of the seven Asian countries.
https://doi.org/10.1371/journal.pone.0246824.s005
- View Article
- Google Scholar
- PubMed/NCBI
- 15. UCLA. What Does Cronbach’s Alpha Mean? 2020 [Available from: https://stats.idre.ucla.edu/spss/faq/what-does-cronbachs-alpha-mean/ .
- 22. Frequently asked questions Permission to use DASS-21: University of New South Wales; [Available from: http://www2.psy.unsw.edu.au/DASS/DASSFAQ.htm#_3.__How_do_I_get_permission_to_use_ .
- 23. Impact of Event Scale-Revised: National Health Service; [Available from: https://www.quest.scot.nhs.uk/hc/en-gb/articles/115002862649-Impact-of-Events-Scale-Revised .
- 26. Worldmeters. COVID Cases Data 2020 2020 [Available from: https://www.worldometers.info/coronavirus/#countries .
- 32. O.P.IMF. Thai GDP Down 6.7% 2020 [Available from: https://www.bangkokpost.com/business/1900795/imf-thai-gdp-down-6-7 .
- 36. G. M. Iran Says U.S. Sanctions Blocked Delivery of UK-Made Masks 2020 [Available from: https://www.bloomberg.com/news/articles/2020-03-21/iran-says-u-s-sanctions-blocked-delivery-of-u-k-made-masks .
- 43. Geddie J SJ. To mask or not to mask: confusion spreads over coronavirus protection: Reuter; 2020 [updated 31 January 2020. Available from: https://uk.reuters.com/article/us-china-health-masks-safety/to-mask-or-not-to-mask-confusion-spreads-over-coronavirus-protection-idUKKBN1ZU0PH .
- 46. Worldbank. Population, Female (% of Total Population) 2020 [Available from: https://data.worldbank.org/indicator/SP.POP.TOTL.FE.ZS .
- Frontiers in Psychology
- Personality and Social Psychology
- Research Topics
Coronavirus Disease (COVID-19): The Impact and Role of Mass Media During the Pandemic
Total Downloads
Total Views and Downloads
About this Research Topic
The outbreak of coronavirus disease 2019 (COVID-19) has created a global health crisis that has had a deep impact on the way we perceive our world and our everyday lives. Not only the rate of contagion and patterns of transmission threatens our sense of agency, but the safety measures put in place to contain ...
Keywords : COVID-19, coronavirus disease, mass media, health communication, prevention, intervention, social behavioral changes
Important Note : All contributions to this Research Topic must be within the scope of the section and journal to which they are submitted, as defined in their mission statements. Frontiers reserves the right to guide an out-of-scope manuscript to a more suitable section or journal at any stage of peer review.
Topic Editors
Topic coordinators, recent articles, submission deadlines.
Submission closed.
Participating Journals
Total views.
- Demographics
No records found
total views article views downloads topic views
Top countries
Top referring sites, about frontiers research topics.
With their unique mixes of varied contributions from Original Research to Review Articles, Research Topics unify the most influential researchers, the latest key findings and historical advances in a hot research area! Find out more on how to host your own Frontiers Research Topic or contribute to one as an author.
An official website of the United States Government
- Kreyòl ayisyen
- Search Toggle search Search Include Historical Content - Any - No Include Historical Content - Any - No Search
- Menu Toggle menu
- INFORMATION FOR…
- Individuals
- Business & Self Employed
- Charities and Nonprofits
- International Taxpayers
- Federal State and Local Governments
- Indian Tribal Governments
- Tax Exempt Bonds
- FILING FOR INDIVIDUALS
- How to File
- When to File
- Where to File
- Update Your Information
- Get Your Tax Record
- Apply for an Employer ID Number (EIN)
- Check Your Amended Return Status
- Get an Identity Protection PIN (IP PIN)
- File Your Taxes for Free
- Bank Account (Direct Pay)
- Payment Plan (Installment Agreement)
- Electronic Federal Tax Payment System (EFTPS)
- Your Online Account
- Tax Withholding Estimator
- Estimated Taxes
- Where's My Refund
- Direct Deposit
- Reduced Refunds
- Amend Return
Credits & Deductions
- INFORMATION FOR...
- Businesses & Self-Employed
- Earned Income Credit (EITC)
- Child Tax Credit
- Clean Energy and Vehicle Credits
- Standard Deduction
- Retirement Plans
Forms & Instructions
- POPULAR FORMS & INSTRUCTIONS
- Form 1040 Instructions
- Form 4506-T
- POPULAR FOR TAX PROS
- Form 1040-X
- Circular 230
Scranton man charged with committing $850,000 in COVID-19 pandemic fraud
More in our agency.
- IRS organization
- A closer look
- Financial and budget reports
- Tax statistics
- Do business with the IRS
- What we investigate
- Identify tax schemes
- Report tax fraud
- Voluntary disclosure
- Investigation process
- Press releases
- Annual report
- Whistleblower Office
- Freedom of Information Act
- Privacy policy
- Civil rights
- Vulnerability disclosure policy
Date: Nov. 6, 2024
Contact: [email protected]
SCRANTON — The United States Attorney’s Office for the Middle District of Pennsylvania announced today that Yoel Weiss of Scranton, Pennsylvania, was charged in an indictment with 41 combined counts of wire fraud, false statements to the Small Business Administration, identity theft, unlawful monetary transactions, and witness tampering.
According to United States Attorney Gerard M. Karam, the indictment alleges that Weiss owned and operated multiple corporate entities in Pennsylvania and New York. Weiss allegedly filed at least seven fraudulent applications for pandemic stimulus funds through the Economic Injury and Disaster Loan (EIDL) program. Weiss was charged with seven counts of wire fraud, and seven count of making false statements to the United States Small Business Administration, for the fraudulent applications. Weiss also is charged with three counts of aggravated identity theft, for using stolen identities to file three applications.
The applications allegedly submitted by Weiss were filed on behalf of corporate entities that did not, in fact, have actual business operations, and that bore false dates of business establishment, false employee headcount information, and fabricated gross revenues, costs of goods sold, and lost rental income. Weiss allegedly obtained in excess of approximately $850,000 in EIDL funds through filing the fraudulent applications, which he spent on unapproved personal expenses. Weiss is charged with 23 counts of making unlawful monetary transactions with the proceeds of his fraud.
Weiss is further charged with threatening and intimidating a witness in an attempt to influence and prevent the witness’s testimony before a federal grand jury.
“The American tax system is designed to provide vital government services to our people. It is not a slush fund for thieves and fraudsters,” said Amy MacNeely, Acting Special Agent in Charge, IRS Criminal Investigation, Philadelphia Field Office.
The EIDL program, funded by the March 2020 CARES Act, was designed to help small businesses facing financial difficulties during the COVID-19 pandemic. EIDL funds are offered in low-interest rate loans, designated for specific business expenses, such as fixed debts, payroll, and business obligation.
The case was investigated by the Internal Revenue Service Criminal Investigation (IRS-CI). Assistant U.S. Robert J. O’Hara is prosecuting the case.
The maximum penalty under federal law for the most serious charges are 20 years of imprisonment, a term of supervised release following imprisonment, and a fine. The aggravated identity theft offense carries a mandatory two-year sentence of imprisonment that is to run consecutive to any other term of imprisonment imposed. A sentence following a finding of guilt is imposed by the Judge after consideration of the applicable federal sentencing statutes and the Federal Sentencing Guidelines.
Indictments are only allegations. All persons charged are presumed to be innocent unless and until found guilty in court.
IRS-CI is the criminal investigative arm of the IRS, responsible for conducting financial crime investigations, including tax fraud, narcotics trafficking, money-laundering, public corruption, healthcare fraud, identity theft and more. IRS-CI special agents are the only federal law enforcement agents with investigative jurisdiction over violations of the Internal Revenue Code, obtaining a more than a 90 percent federal conviction rate. The agency has 20 field offices located across the U.S. and 12 attaché posts abroad.

IMAGES
COMMENTS
The COVID-19 Thesis Impact Statement aims to provide the examiners with a clearer understanding of how the research was affected and shaped due to COVID-19 disruptions. A COVID-19 Thesis Impact Statement is not required and you may submit your thesis for examination without reference to the COVID-19 pandemic. Should you wish to submit your ...
The structure of a doctoral thesis and Covid-19 In this document we attempt to guide you through the usual chapters in a thesis and suggest how the pandemic might be referenced within them. We have listed the purpose of each chapter and considered how you may acknowledge the shaping influence of Covid-19. While this information has
In the introduction, grab your reader's attention and present your thesis statement. For example: Introduction: ... Opinion About the COVID-19 Pandemic. The COVID-19 pandemic has been a transformative event, reshaping every aspect of our lives. In my opinion, while the pandemic has brought immense challenges, it has also offered valuable ...
The global impact of COVID-19, the disease caused by the novel coronavirus, means colleges and prospective students alike are in for an admissions cycle like no other. Both face unprecedented ...
My thesis timeline envisioned the data collection and analysis to be completed in December 2020, but because the interview process was completed just before the holiday break in 2020, the analysis of the data got delayed until 2021 and was completed in February of 2021. As reported in this impact statement. The COVID-19 pandemic affected my thesis
AN ANALYSIS OF THE COVID-19 PANDEMIC 1 CHAPTER ONE Introduction Coronavirus disease (COVID-19) is a highly infectious virus introduced to the United States on January 21, 2020 (World Health Organization). According to many scientists, COVID-19 originated as an epidemic in Wuhan, China from contaminated animal product sold at a
The spread of the "Severe Acute Respiratory Coronavirus 2" (SARS-CoV-2), the causal agent of COVID-19, was characterized as a pandemic by the World Health Organization (WHO) in March 2020 and has triggered an international public health emergency [].The numbers of confirmed cases and deaths due to COVID-19 are rapidly escalating, counting in millions [], causing massive economic strain ...
variation in the e ects of COVID-19 across students. In terms of labor market expectations, on average, students foresee a 13 percentage points decrease in. the probability of. on, a reduction of 2 percent in their reservation wages, a. d a2.3 percent decrease in their expected earn. ID-19 demonstrate that stude.
Introduction. 1.1. Where possible, research students should adapt their research activities to address disruptions caused by Covid-19 restrictions. 1.2. Students may choose to include a statement at the front of their thesis on the impact of disruptions on their work. Examiners will consider this statement as contextual information to support ...
research and their thesis in order to comply with restrictions resulting from the COVID-19 pandemic and public health emergency measures. SGS recommends writing an COVID-19 Impact Statement that can be sent to examiners (as a separate document from your thesis) so they can understand how your thesis has been forced to change.
The COVID-19 crisis is affecting every facet of people's lives in every corner of the world. But tragedy need not be its only legacy. On the contrary, the pandemic represents a rare but narrow window of opportunity to reflect, reimagine, and reset our world to create a healthier, more equitable, and more prosperous future.
The aim of this research is to identify any existing correlations between the COVID-19. pandemic and negative mental health outcomes in younger populations. This paper examines the. impact of the COVID-19 pandemic on the mental health of those younger than 25 years of age, specifically focusing on students.
the last decades significantly. However, the outbreak of the Covid-19 pandemic in 2019 has severely affected the global economy as interconnected value chains have been disrupted, and digitalization has become a sudden necessity due to lockdowns and travel bans. The aim of this master's thesis was to identify the impact of the Covid-19 ...
saw friends lose family members and future employment opportunities to COVID-19. They questioned and changed their lives to adjust to the pandemic. I also watched a mental health crisis emerge for students at the University of Mississippi. This thesis tells their stories, which are filled with hope, fear and ambiguities, and connected by a virus.
Thesis Submission Guidance: COVID-19 Impact Statement. In response to the impact of the global pandemic, we're giving you the option to include a statement at the start of your thesis which outlines the effects that COVID-19 may have had on the research that you have undertaken towards your doctoral degree. The inclusion of a statement is to ...
This essay examines key aspects of social relationships that were disrupted by the COVID-19 pandemic. It focuses explicitly on relational mechanisms of health and brings together theory and emerging evidence on the effects of the COVID-19 pandemic to make recommendations for future public health policy and recovery. We first provide an overview of the pandemic in the UK context, outlining the ...
Even though closing schools is an effective solution to curb the spread of COVID-19, many scholars are concerned about the impact on student intellectual performance and learning variety (Haug et al., 2020).Furthermore, studies found that students underwent inadequate learning and encountered multiple barriers in instructional and educational endeavours during COVID-19 (Khaliq et al., 2020 ...
Introduction The COVID-19 pandemic has certainly resulted in an increased level of anxiety and fear in communities in terms of disease management and infection spread. Due to fear and social stigma linked with COVID-19, many individuals in the community hide their disease and do not access healthcare facilities in a timely manner. In addition, with the widespread use of social media, rumours ...
The coronavirus disease (COVID-19) pandemic has impacted the economy, livelihood, and physical and mental well-being of people worldwide. This study aimed to compare the mental health status during the pandemic in the general population of seven middle income countries (MICs) in Asia (China, Iran, Malaysia, Pakistan, Philippines, Thailand, and Vietnam). All the countries used the Impact of ...
The outbreak of coronavirus disease 2019 (COVID-19) has created a global health crisis that has had a deep impact on the way we perceive our world and our everyday lives. Not only the rate of contagion and patterns of transmission threatens our sense of agency, but the safety measures put in place to contain the spread of the virus also require social distancing by refraining from doing what ...
THE COVID 19 PANDEMIC AND ITS EFFECTS ON MEDICATION USAGETHE COVID. by. Margaret Elizabeth Adamo. A thesis submitted to the Johns Hopkins University in conformity with the requirements for. of Science Baltimore, Maryland May 2021 Abstract Nearly everyone in the. rld has bee.
The EIDL program, funded by the March 2020 CARES Act, was designed to help small businesses facing financial difficulties during the COVID-19 pandemic. EIDL funds are offered in low-interest rate loans, designated for specific business expenses, such as fixed debts, payroll, and business obligation.