The Value of Critical Thinking in Nursing

- How Nurses Use Critical Thinking
- How to Improve Critical Thinking
- Common Mistakes

Some experts describe a person’s ability to question belief systems, test previously held assumptions, and recognize ambiguity as evidence of critical thinking. Others identify specific skills that demonstrate critical thinking, such as the ability to identify problems and biases, infer and draw conclusions, and determine the relevance of information to a situation.
Nicholas McGowan, BSN, RN, CCRN, has been a critical care nurse for 10 years in neurological trauma nursing and cardiovascular and surgical intensive care. He defines critical thinking as “necessary for problem-solving and decision-making by healthcare providers. It is a process where people use a logical process to gather information and take purposeful action based on their evaluation.”
“This cognitive process is vital for excellent patient outcomes because it requires that nurses make clinical decisions utilizing a variety of different lenses, such as fairness, ethics, and evidence-based practice,” he says.

How Do Nurses Use Critical Thinking?
Successful nurses think beyond their assigned tasks to deliver excellent care for their patients. For example, a nurse might be tasked with changing a wound dressing, delivering medications, and monitoring vital signs during a shift. However, it requires critical thinking skills to understand how a difference in the wound may affect blood pressure and temperature and when those changes may require immediate medical intervention.
Nurses care for many patients during their shifts. Strong critical thinking skills are crucial when juggling various tasks so patient safety and care are not compromised.
Jenna Liphart Rhoads, Ph.D., RN, is a nurse educator with a clinical background in surgical-trauma adult critical care, where critical thinking and action were essential to the safety of her patients. She talks about examples of critical thinking in a healthcare environment, saying:
“Nurses must also critically think to determine which patient to see first, which medications to pass first, and the order in which to organize their day caring for patients. Patient conditions and environments are continually in flux, therefore nurses must constantly be evaluating and re-evaluating information they gather (assess) to keep their patients safe.”
The COVID-19 pandemic created hospital care situations where critical thinking was essential. It was expected of the nurses on the general floor and in intensive care units. Crystal Slaughter is an advanced practice nurse in the intensive care unit (ICU) and a nurse educator. She observed critical thinking throughout the pandemic as she watched intensive care nurses test the boundaries of previously held beliefs and master providing excellent care while preserving resources.
“Nurses are at the patient’s bedside and are often the first ones to detect issues. Then, the nurse needs to gather the appropriate subjective and objective data from the patient in order to frame a concise problem statement or question for the physician or advanced practice provider,” she explains.
Top 5 Ways Nurses Can Improve Critical Thinking Skills
We asked our experts for the top five strategies nurses can use to purposefully improve their critical thinking skills.
Case-Based Approach
Slaughter is a fan of the case-based approach to learning critical thinking skills.
In much the same way a detective would approach a mystery, she mentors her students to ask questions about the situation that help determine the information they have and the information they need. “What is going on? What information am I missing? Can I get that information? What does that information mean for the patient? How quickly do I need to act?”
Consider forming a group and working with a mentor who can guide you through case studies. This provides you with a learner-centered environment in which you can analyze data to reach conclusions and develop communication, analytical, and collaborative skills with your colleagues.
Practice Self-Reflection
Rhoads is an advocate for self-reflection. “Nurses should reflect upon what went well or did not go well in their workday and identify areas of improvement or situations in which they should have reached out for help.” Self-reflection is a form of personal analysis to observe and evaluate situations and how you responded.
This gives you the opportunity to discover mistakes you may have made and to establish new behavior patterns that may help you make better decisions. You likely already do this. For example, after a disagreement or contentious meeting, you may go over the conversation in your head and think about ways you could have responded.
It’s important to go through the decisions you made during your day and determine if you should have gotten more information before acting or if you could have asked better questions.
During self-reflection, you may try thinking about the problem in reverse. This may not give you an immediate answer, but can help you see the situation with fresh eyes and a new perspective. How would the outcome of the day be different if you planned the dressing change in reverse with the assumption you would find a wound infection? How does this information change your plan for the next dressing change?
Develop a Questioning Mind
McGowan has learned that “critical thinking is a self-driven process. It isn’t something that can simply be taught. Rather, it is something that you practice and cultivate with experience. To develop critical thinking skills, you have to be curious and inquisitive.”
To gain critical thinking skills, you must undergo a purposeful process of learning strategies and using them consistently so they become a habit. One of those strategies is developing a questioning mind. Meaningful questions lead to useful answers and are at the core of critical thinking .
However, learning to ask insightful questions is a skill you must develop. Faced with staff and nursing shortages , declining patient conditions, and a rising number of tasks to be completed, it may be difficult to do more than finish the task in front of you. Yet, questions drive active learning and train your brain to see the world differently and take nothing for granted.
It is easier to practice questioning in a non-stressful, quiet environment until it becomes a habit. Then, in the moment when your patient’s care depends on your ability to ask the right questions, you can be ready to rise to the occasion.
Practice Self-Awareness in the Moment
Critical thinking in nursing requires self-awareness and being present in the moment. During a hectic shift, it is easy to lose focus as you struggle to finish every task needed for your patients. Passing medication, changing dressings, and hanging intravenous lines all while trying to assess your patient’s mental and emotional status can affect your focus and how you manage stress as a nurse .
Staying present helps you to be proactive in your thinking and anticipate what might happen, such as bringing extra lubricant for a catheterization or extra gloves for a dressing change.
By staying present, you are also better able to practice active listening. This raises your assessment skills and gives you more information as a basis for your interventions and decisions.
Use a Process
As you are developing critical thinking skills, it can be helpful to use a process. For example:
- Ask questions.
- Gather information.
- Implement a strategy.
- Evaluate the results.
- Consider another point of view.
These are the fundamental steps of the nursing process (assess, diagnose, plan, implement, evaluate). The last step will help you overcome one of the common problems of critical thinking in nursing — personal bias.
Common Critical Thinking Pitfalls in Nursing
Your brain uses a set of processes to make inferences about what’s happening around you. In some cases, your unreliable biases can lead you down the wrong path. McGowan places personal biases at the top of his list of common pitfalls to critical thinking in nursing.
“We all form biases based on our own experiences. However, nurses have to learn to separate their own biases from each patient encounter to avoid making false assumptions that may interfere with their care,” he says. Successful critical thinkers accept they have personal biases and learn to look out for them. Awareness of your biases is the first step to understanding if your personal bias is contributing to the wrong decision.
New nurses may be overwhelmed by the transition from academics to clinical practice, leading to a task-oriented mindset and a common new nurse mistake ; this conflicts with critical thinking skills.
“Consider a patient whose blood pressure is low but who also needs to take a blood pressure medication at a scheduled time. A task-oriented nurse may provide the medication without regard for the patient’s blood pressure because medication administration is a task that must be completed,” Slaughter says. “A nurse employing critical thinking skills would address the low blood pressure, review the patient’s blood pressure history and trends, and potentially call the physician to discuss whether medication should be withheld.”
Fear and pride may also stand in the way of developing critical thinking skills. Your belief system and worldview provide comfort and guidance, but this can impede your judgment when you are faced with an individual whose belief system or cultural practices are not the same as yours. Fear or pride may prevent you from pursuing a line of questioning that would benefit the patient. Nurses with strong critical thinking skills exhibit:
- Learn from their mistakes and the mistakes of other nurses
- Look forward to integrating changes that improve patient care
- Treat each patient interaction as a part of a whole
- Evaluate new events based on past knowledge and adjust decision-making as needed
- Solve problems with their colleagues
- Are self-confident
- Acknowledge biases and seek to ensure these do not impact patient care
An Essential Skill for All Nurses
Critical thinking in nursing protects patient health and contributes to professional development and career advancement. Administrative and clinical nursing leaders are required to have strong critical thinking skills to be successful in their positions.
By using the strategies in this guide during your daily life and in your nursing role, you can intentionally improve your critical thinking abilities and be rewarded with better patient outcomes and potential career advancement.
Frequently Asked Questions About Critical Thinking in Nursing
How are critical thinking skills utilized in nursing practice.
Nursing practice utilizes critical thinking skills to provide the best care for patients. Often, the patient’s cause of pain or health issue is not immediately clear. Nursing professionals need to use their knowledge to determine what might be causing distress, collect vital information, and make quick decisions on how best to handle the situation.
How does nursing school develop critical thinking skills?
Nursing school gives students the knowledge professional nurses use to make important healthcare decisions for their patients. Students learn about diseases, anatomy, and physiology, and how to improve the patient’s overall well-being. Learners also participate in supervised clinical experiences, where they practice using their critical thinking skills to make decisions in professional settings.
Do only nurse managers use critical thinking?
Nurse managers certainly use critical thinking skills in their daily duties. But when working in a health setting, anyone giving care to patients uses their critical thinking skills. Everyone — including licensed practical nurses, registered nurses, and advanced nurse practitioners —needs to flex their critical thinking skills to make potentially life-saving decisions.
Meet Our Contributors

Crystal Slaughter, DNP, APRN, ACNS-BC, CNE
Crystal Slaughter is a core faculty member in Walden University’s RN-to-BSN program. She has worked as an advanced practice registered nurse with an intensivist/pulmonary service to provide care to hospitalized ICU patients and in inpatient palliative care. Slaughter’s clinical interests lie in nursing education and evidence-based practice initiatives to promote improving patient care.

Jenna Liphart Rhoads, Ph.D., RN
Jenna Liphart Rhoads is a nurse educator and freelance author and editor. She earned a BSN from Saint Francis Medical Center College of Nursing and an MS in nursing education from Northern Illinois University. Rhoads earned a Ph.D. in education with a concentration in nursing education from Capella University where she researched the moderation effects of emotional intelligence on the relationship of stress and GPA in military veteran nursing students. Her clinical background includes surgical-trauma adult critical care, interventional radiology procedures, and conscious sedation in adult and pediatric populations.

Nicholas McGowan, BSN, RN, CCRN
Nicholas McGowan is a critical care nurse with 10 years of experience in cardiovascular, surgical intensive care, and neurological trauma nursing. McGowan also has a background in education, leadership, and public speaking. He is an online learner who builds on his foundation of critical care nursing, which he uses directly at the bedside where he still practices. In addition, McGowan hosts an online course at Critical Care Academy where he helps nurses achieve critical care (CCRN) certification.
What is Critical Thinking in Nursing? (With Examples, Importance, & How to Improve)

Successful nursing requires learning several skills used to communicate with patients, families, and healthcare teams. One of the most essential skills nurses must develop is the ability to demonstrate critical thinking. If you are a nurse, perhaps you have asked if there is a way to know how to improve critical thinking in nursing? As you read this article, you will learn what critical thinking in nursing is and why it is important. You will also find 18 simple tips to improve critical thinking in nursing and sample scenarios about how to apply critical thinking in your nursing career.
What Is Critical Thinking In Nursing?
4 reasons why critical thinking is so important in nursing, 1. critical thinking skills will help you anticipate and understand changes in your patient’s condition., 2. with strong critical thinking skills, you can make decisions about patient care that is most favorable for the patient and intended outcomes., 3. strong critical thinking skills in nursing can contribute to innovative improvements and professional development., 4. critical thinking skills in nursing contribute to rational decision-making, which improves patient outcomes., what are the 8 important attributes of excellent critical thinking in nursing, 1. the ability to interpret information:, 2. independent thought:, 3. impartiality:, 4. intuition:, 5. problem solving:, 6. flexibility:, 7. perseverance:, 8. integrity:, examples of poor critical thinking vs excellent critical thinking in nursing, 1. scenario: patient/caregiver interactions, poor critical thinking:, excellent critical thinking:, 2. scenario: improving patient care quality, 3. scenario: interdisciplinary collaboration, 4. scenario: precepting nursing students and other nurses, how to improve critical thinking in nursing, 1. demonstrate open-mindedness., 2. practice self-awareness., 3. avoid judgment., 4. eliminate personal biases., 5. do not be afraid to ask questions., 6. find an experienced mentor., 7. join professional nursing organizations., 8. establish a routine of self-reflection., 9. utilize the chain of command., 10. determine the significance of data and decide if it is sufficient for decision-making., 11. volunteer for leadership positions or opportunities., 12. use previous facts and experiences to help develop stronger critical thinking skills in nursing., 13. establish priorities., 14. trust your knowledge and be confident in your abilities., 15. be curious about everything., 16. practice fair-mindedness., 17. learn the value of intellectual humility., 18. never stop learning., 4 consequences of poor critical thinking in nursing, 1. the most significant risk associated with poor critical thinking in nursing is inadequate patient care., 2. failure to recognize changes in patient status:, 3. lack of effective critical thinking in nursing can impact the cost of healthcare., 4. lack of critical thinking skills in nursing can cause a breakdown in communication within the interdisciplinary team., useful resources to improve critical thinking in nursing, youtube videos, my final thoughts, frequently asked questions answered by our expert, 1. will lack of critical thinking impact my nursing career, 2. usually, how long does it take for a nurse to improve their critical thinking skills, 3. do all types of nurses require excellent critical thinking skills, 4. how can i assess my critical thinking skills in nursing.
• Ask relevant questions • Justify opinions • Address and evaluate multiple points of view • Explain assumptions and reasons related to your choice of patient care options
5. Can I Be a Nurse If I Cannot Think Critically?

- Login / Register

‘These three individuals will leave very big shoes to fill’
STEVE FORD, EDITOR
- You are here: Archive
Thinking your way to successful problem-solving
13 September, 2001 By NT Contributor
VOL: 97, ISSUE: 37, PAGE NO: 36
Jacqueline Wheeler, DMS, MSc, RGN, is a lecturer at Buckinghamshire Chilterns University College
Problems - some people like them, some do not think they have any, while others shy away from them as if they were the plague. Opportunities, in the form of problems, are part of your life.
The most difficult decision is deciding to tackle a problem and implement a solution, especially as it is sometimes easier to ignore its existence. Problem-solving takes time and effort, but once a problem has been addressed the nurse can feel satisfied that the issue has been resolved and is therefore less likely to re-emerge.
Nurses make clinical decisions using two different approaches. The first is the rationalist approach, which involves an analysis of a situation so that subsequent actions are rational, logical and based on knowledge and judgement. The second approach is based on a phenomenological perspective, where a fluid, flexible and dynamic approach to decision-making is required, such as when dealing with an acutely ill patient.
Types of problems
Problems come in different guises and the solver can perceive them either as a challenge or a threat. One of the most common types of problem is when the unexpected happens. As a nurse you plan and implement care for a patient based on your knowledge and experience, only to find that the patient’s reaction is totally different from that expected but without any apparent reason.
Another type of problem is an assignment where others set a goal or task. Throughout your working life you will be required to undertake duties on behalf of other people. For some this is difficult as they feel unable to control their workload. Others see it as an opportunity to develop new skills or take on additional responsibilities. Opportunities can be perceived as problems by those who fear failure.
A third type of problem is when a dilemma arises. This is when it is difficult to choose the best solution to a problem because the nurse is confronted with something that challenges his or her personal and/or professional values.
Diagnosing problems
The sooner a problem is identified and solutions devised, the better for all involved. So try to anticipate or identify problems when they occur through continuously monitoring staff performance and patient outcomes.
Listening to and observing junior staff will help you to detect work or organisational concerns, because when there are problems staff are likely to behave in an unusual or inconsistent manner.
Initial analysis
Remember that people view things differently, so what you perceive as a problem may not be one to anyone else. So before you begin thinking about what to do - whether to keep it under surveillance, contain it or find a solution - you should undertake an initial analysis. This will help you to understand the problem more clearly.
An analysis will also enable you to prioritise its importance in relation to other problems as problems do not occur one at a time.
Routine problems often need little clarification, so an initial analysis is recommended for non-routine problems only. Even then, not all problems justify the same degree of analysis. But where it is appropriate, an initial analysis will provide a basis from which to generate solutions.
Perception is also important when dealing with patients’ problems. For example, if a patient gives up reading because he or she cannot hold the book (objective), the nurse may assume it is because the patient has lost interest (subjective, one’s own view).
Generating solutions
It is essential for the problem-solver to remember that, where possible, solutions must come from those connected with the problem. If it is to be resolved, agreement must be owned by those involved as they are probably the best and only people who can resolve their differences. The manager should never feel that he or she must be on hand to deal with all disputes.
To solve a problem you need to generate solutions. However, the obvious solution may not necessarily be the best. To generate solutions, a mixture of creative and analytical thinking is needed (Bransford, 1993).
Creativity is about escaping from preconceived ideas that block the way to finding an innovative solution to a problem. An effective tool for assisting in this process is the technique of lateral thinking, which is based largely on the work of Edward de Bono, who regards thinking as a skill.
There are several ways to encourage creative decision-making. One method that works best for specific or simple problems is brainstorming. If the ground rules of confidentiality and being non-judgemental are applied, it will produce a free flow of ideas generated without fear of criticism (Rawlinson, 1986).
Time constraints and staff availability may make it difficult for all those involved in a problem to meet. In such cases an adaptation of brainstorming - where a blank piece of paper is given to those involved and each writes down four solutions to the problem - may be the answer. A similar technique is the collective notebook, where people are asked to record their thoughts and ideas about a problem for a specified period.
An alternative is where one person writes down a list of solutions in order of priority, which is then added to by others. This helps to prioritise the ideas generated. All these methods produce data that can then be analysed by the problem-solver.
When the problem affects people in different geographical areas, solutions can be generated by obtaining the opinion of experts through the use of a questionnaire, which is known as the Delphi technique (McKenna, 1994).
When an apparently insurmountable problem presents itself, it is often useful to divide it into smaller pieces. This is known as convergent thinking. Using divergent thinking - where you consider a problem in different ways to expand your view - may also help.
A final alternative is the stepladder technique, which is time-consuming but effective if the issue is stirring up strong feelings. This requires the people involved in the problem to be organised into groups. First, two people try to solve the problem, then a third member is drawn in, to whom the solution reached by the first two is presented. All three then try to agree a solution. More people are added to the group, if necessary, in a similar way, until there is agreement of all involved. Provided the individuals are motivated to solve the problem, this technique creates ownership and commitment to implementing the agreed solution.
Analytical thinking, which follows a logical process of eliminating ideas, will enable you to narrow the range down to one feasible solution.
Although someone has to make the ultimate decision on which solution to implement, there are advantages to group decision-making: a greater number of possible solutions are generated and conflicts are resolved, resulting in decisions being reached through rational discussion.
This does, however, require the group to be functioning well or the individuals involved may feel inhibited in contributing to the decision-making. One individual may dominate the group or competition between individuals may result in the need to win taking precedence over deciding on an agreed practical solution.
As nursing becomes less bureaucratic individuals are being encouraged to put forward their own ideas, but social pressures to conform may inhibit the group. We do not solve problems and make decisions in isolation, but are influenced by the environment in which we work and the role we fulfil in that environment. If group members lack commitment and/or motivation, they may accept the first solution and pay little attention to other solutions offered.
Making a decision
There are three types of decision-making environments: certain, risk and uncertain. The certain environment, where we have sufficient information to allow us to select the best solution, is the most comfortable within which to make a decision, but it is the least often encountered.
We usually encounter the risk environment, where we lack complete certainty about the outcomes of various courses of action.
Finally, the uncertain environment is the least comfortable within which to make decisions as we are almost forced to do this blind. We are unable to forecast the possible outcomes of alternative courses of action and, therefore, have to rely heavily on creative intuition and the educated guess.
Taking this into consideration, you should not contemplate making a decision until you have all the information needed. Before you make your decision, remind yourself of the objective, reassess the priorities, consider the options and weigh up the strengths, weaknesses, opportunities and threats of each solution.
An alternative is to use the method that Thomas Edison used to solve the problem of the electric light bulb. Simply focus on your problem as you drift off to sleep, and when you wake up your subconscious mind will have presented you with the answer. But bear in mind that this is not a scientific way of solving problems - your subconscious can be unreliable.
If you are not sure about your decision, test the solution out on others who do not own the problem but may have encountered a similar dilemma. Once you have made your choice stick to it, or you may find it difficult to implement because those involved will never be sure which solution is current. They will also be reluctant to become involved in any future decision-making because of your uncertainty.
The next step is to ensure that all the people involved know what decision has been made. Where possible, brief the group and follow this up with written communication to ensure everyone knows what is expected of them. You may need to sell the decision to some, especially if they were not involved in the decision-making process or the solution chosen is not theirs.
Implementing the solution
Finally, to ensure the solution is implemented, check that the people involved know who is to do what, by when and that it has happened. Review the results of implementing your solution (see Box) and praise and thank all those involved.
- Part 1 of this series was published in last week’s issue: Wheeler, J. (2001) How to delegate your way to a better working life. Nursing Times; 97: 36, 34-35.
Next week. Part three: a step-by-step guide to effective report writing.
- Add to Bookmarks
Have your say
Sign in or Register a new account to join the discussion.
Problem solving in nursing practice: application, process, skill acquisition and measurement
Affiliation.
- 1 King's College, University of London, England.
- PMID: 8320382
- DOI: 10.1046/j.1365-2648.1993.18060886.x
This paper analyses the role of problem solving in nursing practice including the process, acquisition and measurement of problem-solving skills. It is argued that while problem-solving ability is acknowledged as critical if today's nurse practitioner is to maintain effective clinical practice, to date it retains a marginal place in nurse education curricula. Further, it has attracted limited empirical study. Such an omission, it is argued, requires urgent redress if the nursing profession is to meet effectively the challenges of the next decade and beyond.
Publication types
- Research Support, Non-U.S. Gov't
- Education, Nursing
- Educational Measurement
- Nurses / psychology*
- Problem Solving*

Two Examples of How I Used Critical Thinking to Care for my Patient (Real Life Nursing Stories) | NURSING.com

What are you struggling with in nursing school?
NURSING.com is the BEST place to learn nursing. With over 2,000+ clear, concise, and visual lessons, there is something for you!
Critical Thinking on the Nursing Floor
Critical thinking can seem like such an abstract term that you don’t practically use. However, this could not be farther from the truth. Critical thinking is frequently used in nursing. Let me give you a few examples from my career in which critical thinking helped me take better care of my patient.
The truth is, that as nurses we can’t escape critical thinking . . . I know you hate the word . . . but let me show you how it actually works!
Critical Thinking in Nursing: Example 1
I had a patient that was scheduled to go to get a pacemaker placed at 0900. The physician wanted the patient to get 2 units of blood before going downstairs for the procedure. I administered it per protocol. About 30 minutes after that second unit got started, I noticed his oxygen went from 95% down to 92% down to 90%. I put 2L of O2 on him and it came up to 91%. But it just sort of hung around the low 90s on oxygen.
I stopped. And thought. What the heck is going on?
I looked at his history. Congestive heart failure.
I looked at his intake and output. He was positive 1.5 liters.
I thought about how he’s got extra fluid in general, and because of his CHF, he can’t really pump out the fluid he already has, let alone this additional fluid. Maybe I should listen to his lungs..
His lungs were clear earlier. I heard crackles throughout both lungs.
OK, so he’s got extra fluid that he can’t get out of his body. What do I know that will get rid of extra fluid and make him pee? Maybe some Lasix?
I ran over my thought process with a coworker before calling the doc. They agreed. I called the doc and before I could suggest anything, he said “Give him 20 mg IV Lasix one time, and I’ll put the order in.” CLICK.
I gave the Lasix. He peed like a racehorse (and was NOT happy with me for making that happen!). And he was off of oxygen before he went down to get his pacemaker.
Badda Bing Bada Boom!
Critical Thinking in Nursing: Example 2
My patient just had her right leg amputated above her knee. She was on a Dilaudid PCA and still complaining of awful pain. She maxed it out every time, still saying she was in horrible pain. She told the doctor when he rounded that morning that the meds weren’t doing anything. He added some oral opioids as well and wrote an order that it was okay for me to give both the oral and PCA dosings, with the goal of weaning off PCA.
“How am I going to do that?” I thought. She kept requiring more and more meds and I’m supposed to someone wean her off?
I asked her to describe her pain. She said it felt like nerve pain. Deep burning and tingling. She said the pain meds would just knock her out and she’d sleep for a little while but wake up in even worse pain. She was at the end of her rope.
I thought about nerve pain. I thought about other patients that report similar pain. Diabetics with neuropathy would talk about similar pain… “What did they do for it? ” I thought. Then I remembered that many of my patients with diabetic neuropathy were taking gabapentin daily for pain.
“So if this works for their nerve pain, could it work for a patient who has had an amputation?” I thought.
I called the PA for the surgeon and asked them what they thought about trying something like gabapentin for her pain after I described my patient’s type of pain and thought process.
“That’s a really good idea, Kati. I’ll write for it and we’ll see if we can get her off the opioids sooner. ”
She wrote for it. I gave it. It takes a few days to really kick in and once it did, the patient’s pain and discomfort were significantly reduced. She said to get rid of those other pain meds because they “didn’t do a damn thing,” and to “just give her that nerve pain pill because it’s the only thing that works”.
And that we did!
She was able to work with therapy more because her pain was tolerable and was finally able to get rest.
What the HELL is Critical Thinking . . . and Why Should I Care?
What your nursing professor won’t tell you about critical thinking .
by Ashely Adkins RN BSN
When I started nursing school, I remember thinking, “how in the world am I going to remember all of this information, let alone be able to apply it and critically think?” You are not alone if you feel like your critical thinking skills need a little bit of polishing.
Let’s step back for a moment, and take a walk down memory lane. It was my first semester of nursing school and I was sitting in my Fundamentals of Nursing course. We were learning about vital signs, assessments, labs, etc. Feeling overwhelmed with all of this new information (when are you not overwhelmed in nursing school?), I let my mind wonder to a low place…
Am I really cut out for this? Can I really do this? How can I possibly retain all of this information? Do they really expect me to remember everything AND critically think at the same time?
One of my first-semester nursing professors said something to me that has stuck with me throughout my nursing years. It went a little something like this:
“Critical thinking does not develop overnight . It takes time. You don’t learn to talk overnight or walk overnight. You don’t learn to critically think overnight .”
My professor was absolutely right.
As my journey throughout nursing school, and eventually on to being a “real nurse” continued, my critical thinking skills began to BLOSSOM. With every class, lecture, clinical shift, lab, and simulation, my critical thinking skills grew.
You may ask…how?
Well, let me tell you…
- Questioning
These are the key ingredients to growing your critical thinking skills.
Time. Critical thinking takes time. As I mentioned before, you do not learn how to critically think overnight. It is important to set realistic expectations for yourself both in nursing school and in other aspects of your life.
Exposure. It is next to impossible to critically think if you have never been exposed to something. How would you ever learn to talk if no one ever talked to you? The same thing applies to nursing and critical thinking.
Over time, your exposure to new materials and situations will cause you to think and ask yourself, “why?”
This leads me to my next point. Questioning. Do not be afraid to ask yourself…
“Why is this happening?”
“Why do I take a blood pressure and heart rate before I give a beta-blocker?”
“Why is it important to listen to a patient’s lung sounds before and after they receive a blood transfusion?”
It is important to constantly question yourself. Let your mind process your questions, and discover answers.
Confidence. We always hear the phrase, “confidence is key!” And as cheesy as that phrase may be, it really holds true. So many times, we often times sell ourselves short.
YOU KNOW MORE THAN YOU THINK YOU KNOW.
In case you did not catch it the first time…
Be confident in your knowledge, because trust me, it is there. It may be hiding in one single neuron in the back of your brain, but it is there.
It is impossible to know everything. Even experienced nurses do not know everything.
And if they tell you that they do…they are wrong!
The key to critical thinking is not about knowing everything ; It is about how you respond when you do not know something .
How do you reason through a problem you do not know the answer to? Do you give up? Or do you persevere until you discover the answer?
If you are a nursing student preparing for the NCLEX, you know that the NCLEX loves critical thinking questions. NRSNG has some great tips and advice on critical thinking when it comes to taking the NCLEX .
There are so many pieces to the puzzle when it comes to nursing, and it is normal to feel overwhelmed. The beauty of nursing is when all of those puzzle pieces come together to form a beautiful picture.
That is critical thinking.
Critical thinking is something you’ll do every day as a nurse and honestly, you probably do it in your regular non-nurse life as well. It’s basically stopping, looking at a situation, identifying a solution, and trying it out. Critical thinking in nursing is just that but in a clinical setting.
We’ve written a MASSIVE lesson on Care Plans and Critical Thinking :
Mastering The COPD Nursing Care Plan in Just 10 Minutes!
Renal Failure Pt Care
4 "real world" examples of using clinical judgement to figure out what to do first as a nurse | nursing.com, 12 study tips for how to study for pharmacology in nursing school | nursing.com, similar blog posts.

Critical Thinking and Nursing Care Plans Go Together Like Chicken and Waffles | NURSING.com

Patients We Will Never Forget | NURSING.com

The Ultimate Guide to Creating an ICU Report Sheet (for new Critical Care Nurses and RN Students) | NURSING.com
An official website of the United States government
The .gov means it’s official. Federal government websites often end in .gov or .mil. Before sharing sensitive information, make sure you’re on a federal government site.
The site is secure. The https:// ensures that you are connecting to the official website and that any information you provide is encrypted and transmitted securely.
- Publications
- Account settings
Preview improvements coming to the PMC website in October 2024. Learn More or Try it out now .
- Advanced Search
- Journal List
- Int J Environ Res Public Health

Communication Skills, Problem-Solving Ability, Understanding of Patients’ Conditions, and Nurse’s Perception of Professionalism among Clinical Nurses: A Structural Equation Model Analysis
This study was intended to confirm the structural relationship between clinical nurse communication skills, problem-solving ability, understanding of patients’ conditions, and nurse’s perception of professionalism. Due to changes in the healthcare environment, it is becoming difficult to meet the needs of patients, and it is becoming very important to improve the ability to perform professional nursing jobs to meet expectations. In this study method, structural model analysis was applied to identify factors influencing the perception of professionalism in nurses. The subjects of this study were 171 nurses working at general hospitals in city of Se, Ga, and Geu. Data analysis included frequency analysis, identification factor analysis, reliability analysis, measurement model analysis, model fit, and intervention effects. In the results of the study, nurse’s perception of professionalism was influenced by factors of communication skills and understanding of the patient’s condition, but not by their ability to solve problems. Understanding of patient’s condition had a mediating effect on communication skills and nursing awareness. Communication skills and understanding of the patient’s condition greatly influenced the nurse’s perception of professionalism. To improve the professionalism of clinical nurses, nursing managers need to emphasize communication skills and understanding of the patient’s condition. The purpose of this study was to provide a rationale for developing a program to improve job skills by strengthening the awareness of professional positions of clinical nurses to develop nursing quality of community.
1. Introduction
Changes in the environment related to climate and pollution are causing health problems and various diseases such as respiratory and circulatory problems, metabolic disorders, and chronic diseases. Moreover, access to modern healthcare facilities has created greater expectations among patients receiving personalized healthcare and high-quality healthcare. As the difficulty of satisfying the demands of patients increases, enhancing nursing capabilities has become increasingly important [ 1 ]. To improve this, hospitals are making efforts to change the internal and external environments so as to increase the number of nurses, reduce the length of hospital stays, and enable efficient nursing practice. Despite these efforts, the workloads of nurses and the demand for clinical nurses are continuously increasing [ 2 , 3 ]. As a result, nurses are developing negative attitudes and prejudices toward patients, as well as negative perceptions of professionalism. To address this, the cultivation and strengthening of nursing professionals’ capabilities is essential.
Nurses’ perception of professionalism is an important element influencing their ability to perform independent nursing, and a good perception of their profession results in a positive approach to solving patients’ problems [ 4 , 5 ]. In addition, the characteristics and abilities of individual nurses can influence the level of care and enable them to understand patients, solve problems, and provide holistic care, which is the ultimate goal of the nursing process [ 6 , 7 ]. Thus, patients expect nurses to not only have medical knowledge of the disease but to also be able to comprehensively assess the patient’s problems and be independent and creative in nursing [ 8 ]. This attitude can have a major impact on the quality of nursing services and can inspire pride in the nursing occupation and professional achievement. These findings can also be used by nurses to prevent burnout and maintain professionalism [ 9 , 10 ].
To respond to the increasing demands for diverse qualitative and quantitative nursing services and to strengthen the capabilities of nursing professionals, efforts have been made to move nursing education toward scientific and creative education. However, in point-of-care environments, not only are nurses prevented from making independent decisions regarding nursing, but also the diverse personal capabilities necessary for such independent behavior are not sufficiently developed [ 11 ]. Therefore, it is important to enhance clinical nurses’ perceptions of the nursing profession; maintain a balance of nursing capabilities; provide novel, high-quality nursing services; and identify assistive nursing education methods and obstructive environmental factors [ 10 ].
Communication skills involve a person’s ability to accurately understand (through both verbal and non-verbal indications) another person, and sufficiently deliver what the person desires [ 12 , 13 ]. Good communication skills are a primary requirement for providing professional nursing services because they enable an in-depth understanding of patients, solving of complicated problems, and reasonable and logical analysis of situations [ 14 , 15 , 16 ]. When effective communication takes place, nurses’ problem-solving abilities and perceived professionalism strengthen [ 17 , 18 ].
According to Park [ 19 ], nurses have difficulties in interpersonal relationships when social tension and interaction skills are low and communication is poor. In addition, these factors are negatively affected not only in the work of the nurse but also in the perception of the profession. Communication skills are associated with both the formation of relationships with patients and the ability to perform holistic nursing [ 20 ]. In order to improve and develop the overall nursing function of a clinical nurse like this, it is important to complement the relevant integrated nursing abilities [ 21 , 22 ].
Previous studies have investigated the importance of communication skills for nurses, and the relationships between nurses’ problem-solving ability and their understanding of the patients’ conditions. Nonetheless, data that can comprehensively explain the structural relationships between these qualities and how they affect the job perception of nurses remains insufficient.
Therefore, the present study aims to identify the structural model for the relationships between nurses’ communication skills, problem-solving ability, understanding of patients’ conditions, and nurse’s perception of professionalism. Additionally, the study provides basic data necessary for developing programs for improving nursing abilities.
The purpose of this study is to construct a theoretical model that explains the structural relationships among nurses’ communication skills, problem-solving ability, understanding of patients’ conditions, and nurse’s perception of professionalism. In addition, the study aimed to verify this model using empirical data.
2. Materials and Methods
2.1. study design.
To create and analyze the structural model for clinical nurses’ communication skills, problem-solving ability, understanding of patients’ conditions, and nurse’s perception of professionalism, the theoretical relationships among the variables were developed based on related theories.
In this study, communication skills were set as the exogenous variables, whereas problem-solving ability, understanding of patients’ conditions, and perception of the nursing occupation were set as the endogenous variables. In addition, communication skills were set as the independent variables and nursing job perceptions as the dependent variable. This is because the ability of communication helps to maintain an intimate relationship with the patient and to assess the patient’s condition through each other’s relationship and to solve problems and develop correct understanding. Communication skills, problem-solving ability, and understanding of patients’ conditions were set as the parameters for determining causality. The research model is shown in Figure 1 .

Study model.
2.2. Study Participants
The structural equation model has less than 12 measurement variables. The sample size usually requires 200 to 400 participants [ 23 ]. A total of 250 participants were selected for the study. In line with ethical standards and practices, participants received a full explanation on the purpose of the study. They were briefed that the information collected would be used for research purposes only. Furthermore, they were informed that they could withdraw from the study at any time.
2.3. Data Collection Method
Data collection for this study was performed by two researchers unrelated to the hospital from April 20 to May 1, 2019. A questionnaire was used to collect data from clinical nurses working in five hospitals in Seoul, Gyeonggi, and Gangwon provinces. Of the 250 questionnaires disseminated, we received 225 completed returns. However, 54 were considered inaccurate, inconsistent, or unsatisfactory for coding purposes. Thus, 171 fully completed valid questionnaires comprised the final dataset for analysis.
2.4. Research Instruments
2.4.1. communication skills.
In this study, the communication skill instrument developed by Lee and Jang [ 24 ] was used. Its contents were modified and supplemented to clearly understand the communication skills of nurses. Our questionnaire comprised 20 questions with five questions each concerning “interpretation ability,” “self-reveal,” “leading communication,” and “understanding others’ perspectives.” The answers were rated on a five-point Likert scale ranging from 0 = “strongly disagree” to 4 = “strongly agree.” For this study, the Cronbach’s alpha value was 0.81.
2.4.2. Problem-Solving Ability
The tool developed by Lee [ 25 ] was used to measure the problem-solving ability of clinical nurses. The survey comprised 25 questions, with five questions each concerning “problem recognition,” “information-gathering,” “divergent thinking,” “planning power,” and “evaluation.” Items were scored on a five-point Likert scale ranging from 0 = “strongly disagree” to 4 = “strongly agree.” The internal consistency confidence value Cronbach’s alpha was 0.79.
2.4.3. Understanding Patients’ Condition
To measure nurses’ understanding of patients’ conditions, we developed 10 questions by revising and supplementing items from an existing understanding-measurement tool [ 26 ]. With a total of ten questions, we measured “diagnostic name,” “patient-treatment planning,” and “nursing intervention processes.” Items were scored using a five-point Likert scale ranging from 0 = “strongly disagree” to 4 = “strongly agree.” The internal consistency confidence value Cronbach’s alpha was 0.81.
2.4.4. Nurse’s Perception of Professionalism
Nurse’s perception of professionalism was measured using a tool developed by revising the 25 questions created by Kang et al. [ 1 ]. With a total of ten questions, we measured “vocation” and “autonomy.” Items were scored using a five-point Likert scale. The internal consistency confidence value Cronbach’s alpha was 0.81.
2.5. Data Analysis
To identify the relationships among the set variables, the data were computed statistically using the program included in IBM SPSS 24.0 and AMOS 23.0. (IBM Corp., Armonk, NY, USA). The analysis methods were as follows:
- Frequency analysis was conducted to identify the subjects’ demographic and general characteristics.
- The reliability of the questionnaire was verified using Cronbach’s α coefficients.
- Confirmatory factor analysis (CFA) was performed to verify the convergent validity of the selected measurement tool.
- The normality of the data was determined through analyzing the skewness and kurtosis of the measurement variables.
- The fitness of the model was verified using structural equation modeling (SEM).
- Bootstrapping was utilized to verify the mediating effect in the set study model, as well as the mediating effects of the nurses’ problem-solving ability and understanding of patients’ conditions.
3.1. Demographic Characteristics
The demographic and general characteristics of the study subjects are shown in Table 1 . Overall, 71 respondents were aged 25–29 years (41.5%), representing the most numerous age group. University graduates comprised 113 (66.1%) of the sample, while 50 (29.2%) held graduate degrees, with eight (4.7%) holding master’s degrees. Fifty-three respondents (31.0%) had over seven years of clinical experience, 43 (25.1%) had two to three years of experience, 42 (24.6%) had four to six years of experience, and 33 (19.3%) had less than two years of experience. Additionally, 121 respondents (70.8%) worked at secondary hospitals, while 50 (29.2%) worked at tertiary hospitals; 159 respondents (93.0%) reported that they were general nurses.
Participants’ general characteristics ( N = 171, %).
3.2. Technical Metrics of the Measurement Variables
The multivariate normality of the findings related to the factors of the latent variables was verified through standard deviations, skewness, and kurtosis. The present study meets the criteria for the skewness and kurtosis values mentioned by Hu and Bentler [ 27 ].
All sub-factors of the latent variables secured normality.
In this study, a normal distribution was obtained for each of the four sub-factors of communication skills, five sub-factors of problem-solving ability, three sub-factors for understanding the patient’s condition, and two sub-factors of the nurse’s perception of professionalism as shown in Table 2 .
Technical metrics of the measurement variables ( N = 171).
3.3. Correlations between the Measured Variables
The correlations between the measurement variables were analyzed using Pearson’s product–moment correlation coefficient analysis ( Table 3 ). The correlations among all individual measurement variables were found to show a positive correlation.
Correlations between the observed variables.
3.4. Confirmatory Factor Analysis of the Measurement Model
This study examined how well the measurement variables represented the latent variables in the measurement model. Each set path coefficient was evaluated using non-standardization factors, standardization factors, and standard errors. The path coefficients refer to the factor loadings in CFA. The standardization factors of the individual paths were shown to be at least 0.50 (except for vocation: 0.36), and the critical ratio (CR) was at least 1.96. This indicated that the measurement tool had good convergent validity ( Table 4 ).
Confirmatory factor analysis of the measurement model.
*** p < 0.001; CR: critical ratio.
3.5. Verification of the Structural Model
The structural model for relationships among clinical nurses’ communication skills, problem-solving ability, understanding of patients’ condition, and nurse’s perception of professionalism that would be suitable for predicting the influencing relationships was verified. Since the fitness index of the modified model was shown to be higher than that of the initial model, the final model for this study was set as shown in Figure 2 .

Final model. * χ 2 = 124.074 (df = 61, p <0.001), GFI(Goodness of Fit Index)= 0.90, RMSEA(Root Mean Square Error Approximation)=0.07, NFI(Normed Fit Index)=0.87, IFI(Incremental Fit Index)= 0.93, TLI(Tucker-Lewis Index)= 0.91, CFI(Comparative Fit Index)= 0.92.

3.6. Influencing Relationships between Variables of the Study Model
The standardization factors and CR values of the final model were examined to determine whether there were direct relationships between communication skills, problem-solving ability, understanding of patients’ conditions, and nurse’s perception of professionalism. The results are shown
For the relationship between communication ski in Table 5 .lls and problem-solving ability, the standardization factor was 0.85 and the CR value was 7.37; communication skills showed a statistically significant effect. Consequently. The relationship between communication skills and understanding of patients’ conditions also showed a statistically significant effect. Consequently, Hypothesis 1 was supported.
The relationships between the human effects of the measurement model.
* p < 0.05, *** p < 0.001; CR: critical ratio.
For the relationship between communication skills and nurse’s perception of professionalism, the standardization factor was 0.54, and the CR value was 2.02. Communication skills showed a statistically significant effect. Consequently. For the relationship between problem-solving ability and nurse’s perception of professionalism, the standardization factor was −0.056, and the CR value was −0.39. Problem-solving ability had no statistically significant effect. Consequently.
The relationship between nurses’ understanding of patients’ conditions and nurse’s perception of professionalism had a statistically significant effect. Consequently Figure 2 shows the influencing relationships between the study variables of the final study model, considering non-standardization and standardization factors of the relationships between the study variables.
3.7. Direct and Indirect Effects of the Variables
To grasp the significance of the mediating effect in the final study model, the direct and indirect effects of each variable were examined. To examine the mediating effect of the problem-solving ability and understanding of patients’ conditions variables, the bootstrapping method provided by the AMOS 23.0 program included in IBM was utilized. The results are shown in Table 6 .
Mediating effect analysis.
* p < 0.05, *** p < 0.001
The indirect effect of communication skills on nurse’s perception of professionalism through nurses’ understanding of patients’ conditions was statistically significant. That is, clinical nurses’ communication skills have an indirect positive effect on their nurse’s perception of professionalism, with nurses’ understanding of patients’ conditions acting as a parameter. We also found that the effect of communication skills on nurse’s perception of professionalism was statistically significant. Therefore, communication skills have a partially mediated effect on nurse’s perception of professionalism, with understanding of patients’ conditions acting as a parameter. However, communication skills were found to have no indirect positive effect on nurse’s perception of professionalism when problem-solving ability was set as a parameter.
4. Discussion
In this study, we developed and analyzed a hypothetical model regarding clinical nurses’ communication skills, problem-solving ability, and understanding of patients’ conditions, and how these factors influence their nurse’s perception of professionalism.
4.1. Effect of Communication Skills on Nurses’ Perception of Professionalism
Communication skills were found to have statistically significant effects on their relationship with nurses’ problem-solving ability, understanding of patients’ conditions, and nurse’s perception of professionalism. Nurses’ communication skills not only affected their problem-solving ability but also their understanding of patients’ conditions and nurse’s perception of professionalism. Good communication among nurses can reduce uncomfortable situations and improve interactions with patients, which can consequently enhance problem-solving [ 28 ]. Supporting our findings, Ancel [ 17 ] reported that communication skills afford the maintenance of amicable cooperative relationships with patients across diverse medical classes, thereby enhancing the efficiency of nursing-related problem-solving.
Nurses’ communication is also closely related to their understanding of patients’ conditions, particularly regarding the treatment processes. Nurses frequently experience difficulties as a result of poor communication with not only patients and their family members but also other medical personnel. Further, poor delivery of explanations and questions affects nurses’ understanding of patients’ situations and problems, and patients can also feel concern regarding whether nurses accurately understand their problems [ 29 ]. Nurses frequently experience psychological abuse when communicating with patients and develop stress or discomfort [ 30 ]; this can lead to distrustful relationships with and inhibited understanding of patients [ 31 , 32 ]. Vermeir et al. [ 18 ] reported that scientific approaches are required to understand patients in-depth. To accurately understand both oneself and others, the most important method is successful communication. Such findings support the present study’s indication that nurses’ communication is a basic means of solving nursing problems, with both actions being interrelated.
Our finding that nurses’ communication skills are structurally related to their nurse’s perception of professionalism supports the findings of many previous studies. Regarding nurse’s perception of professionalism, Adams et al. [ 33 ] as well as Lee and Kim [ 34 ] explained that a good perception leads to higher-level capabilities, fostering high-level nursing of patients and the development of autonomous vocation. The above studies reported that, since nurses’ communication skills are related to their nurse’s perception of professionalism, communication skills should be considered a predictor of success. Further, McGlynn et al. [ 35 ] recommended positively reinforcing communication skills to improve nurse’s perception of professionalism. This supports the findings of the present study, indicating that communication and nursing professional perception are interrelated.
Thus, communication skills are important for nursing patients. They enable nurses to accurately understand patients’ problems, serve (by forming patient trust) an important function in the process of administering nursing interventions, and positively affect nurses’ perception of their profession. As such, each concept is important. However, nurses working in the clinic are critically aware of their professionalism. In order to reinforce this, communication skills are required, and the emphasis is placed on strengthening the nurses’ ability to solve problems as well as assess and understand patients. As a result, communication skills play an important role in helping nurses understand patients’ problems accurately, build patient trust in nursing interventions, and create structural relationships that have a positive impact on the perception of nursing occupations. Therefore, efforts to improve nurses’ communication skills not only improve their problem-solving abilities and understanding of patients’ conditions but also improve their nurse’s perception of professionalism. To maintain the professionalism of nurses, “competency development programs” would be helpful, thereby emphasizing the need for their application in nursing colleges and clinical practice.
4.2. Relationship between Nurses’ Problem-Solving Ability and Nurse’s Perception of Professionalism
We found clinical nurses’ problem-solving ability to have no positive effect on their perception of professionalism. This contrasts with previous studies, which reported that problem-solving ability is helpful for such perception of professionalism [ 36 ]. We also found that problem-solving ability does not affect nursing professional perception through a mediating effect.
The present findings indicate that the distinctiveness of the fields of nursing should not be overlooked. In nursing organizations that have a culture of discouraging diversity, when negative results are obtained from attempts to solve nursing problems, confusion regarding the identity of nursing professionals means perception of the profession is not reinforced; in many cases, the opposite perception is formed. Furthermore, for those in lower-level positions, nurse’s perception of professionalism is thought to be low because they cannot voice their opinions and have difficulties such as excessive workloads. Although few previous studies have directly examined this, Vermeir et al. [ 18 ] explained that, as the role expectation for nurses increases, factors for job turnover increase as a result of a sense of confusion regarding the nurses’ role and increases in stress. These findings indicate that factors that degrade nurses’ problem-solving ability induce skepticism regarding nursing and possibly career change, thereby supporting the findings of this study.
However, in the present study, positive results with low levels of relevancy in the structural model but high correlations were found. It is expected that, if nurses’ environmental conditions are improved and their nursing capabilities are developed so that they can solve nursing problems with confidence, their nursing professional perception will improve.
4.3. Relationship between Nurses’ Understanding of Patients’ Conditions and Nurse’s Perception of Professionalism
Our findings indicated that the relationship between nurses’ understanding of patients’ conditions and nurse’s perception of professionalism was statistically significant. This supports Nilsson et al. [ 21 ] and Philip et al. [ 29 ], who reported that, in the fields of nursing, when patients accurately understand nurses’ instructions or explanations and health information, they can participate in, independently adjust, and engage in creative decision-making related to self-nursing.
McGlynn et al. [ 35 ] suggested that understanding patient problems is an important element in resolving negative situations; meanwhile, Heo and Lim [ 37 ] indicated that clinical nurses provide high-quality nursing services and develop self-efficacy when they apply professional knowledge and a desire to understand patients’ problems. These study findings accord with our own findings.
The aforementioned findings suggest that the development and application of programs that can enhance nurses’ understanding of patients’ conditions should be emphasized, and that studies of various patient types, the characteristics of patients by age group and hospital areas, as well as the introduction of simulation education programs to improve nurses’ understanding of patients’ conditions should be continuously implemented.
5. Conclusions
This study aimed to verify the structural relationships between clinical nurses’ communication skills and their problem-solving ability, understanding of patients’ conditions, and nurse’s perception of professionalism. We also aimed to identify, through a structural model, the mediating effects of nurses’ problem-solving ability and understanding of patients’ conditions in the relationship between communication skills and nurse’s perception of professionalism.
The findings of this study are as follows (all significance levels = 0.05). In the relationship between communication skills and problem-solving ability, the value of the standardization factor was 0.85 and the CR value was 7.37, indicating that communication skills had a statistically significant effect. In the relationship between nurses’ communication skills and understanding of patients’ conditions, the value of the standardization factor was 0.61 and the CR value was 6.35, indicating that communication skills had a statistically significant effect. In the relationship between communication skills and nurse’s perception of professionalism, the value of the standardization factor was 0.54 and the CR value was 2.02, indicating that communication skills had a statistically significant effect. However, in the relationship between problem-solving ability and nurse’s perception of professionalism, the value of the standardization factor was −0.05 and the CR value was −0.39, indicating that problem-solving ability has no statistically significant effect. Finally, in the relationship between nurses’ understanding of patients’ conditions and nurse’s perception of professionalism, the value of the standardization factor was 0.56, and the CR value was 2.14, indicating that nurses’ understanding of patients’ conditions has a statistically significant effect.
There are some limitations to this study. First, as we only examined nurses at secondary and tertiary university hospitals, our findings may not be generalizable to all clinical nurses. Replication studies examining a range of levels of medical institutions and associated workers are necessary. Second, the structural relationship between problem-solving ability and the nurse’s perception of professionalism turned out to be insignificant or mediated. Subsequent studies on the various approaches to revisit this structural relationship should be performed. Third, theories should be systematically developed to establish the values of the nursing profession, and additional studies are necessary to explore other variables.
Acknowledgments
We would like to thank the staff nurses who participated in the survey and took the time to complete the initial assessment.
Author Contributions
Conceptualization, A.Y.K. and I.O.S.; methodology, A.Y.K.; software, I.O.S.; validation, A.Y.K. and I.O.S.; formal analysis, A.Y.K. and I.O.S.; investigation, A.Y.K.; resources, A.Y.K.; data curation, A.Y.K.; writing—original draft preparation, A.Y.K.; writing—review and editing, A.Y.K. and I.O.S.; visualization, A.Y.K. and I.O.S.; supervision, I.O.S.; project administration, I.O.S. All authors have read and agreed to the published version of the manuscript.
This research received no external funding.
Conflicts of Interest
The authors declare no conflict of interest.
Find Study Materials for
- Explanations
- Business Studies
- Combined Science
- Computer Science
- Engineering
- English Literature
- Environmental Science
- Human Geography
- Macroeconomics
- Microeconomics
- Social Studies
- Browse all subjects
- Read our Magazine
Create Study Materials
- Flashcards Create and find the best flashcards.
- Notes Create notes faster than ever before.
- Study Sets Everything you need for your studies in one place.
- Study Plans Stop procrastinating with our smart planner features.
- Problem Solving in Nursing Management
Dive deep into the multifaceted world of nursing management with a special focus on problem-solving. This comprehensive guide presents a detailed look at the process, importance, and challenges of problem-solving in nursing management. By highlighting essential skills, neurologically based frameworks, and the relationship with decision-making, it offers both theoretical understanding and practical solutions. Explore real-life case studies, leadership's role, and the link with critical thinking. This is an enriching journey towards developing strategic competencies and achieving effective problem-solving in a vital healthcare sector.
Create learning materials about Problem Solving in Nursing Management with our free learning app!
- Instand access to millions of learning materials
- Flashcards, notes, mock-exams and more
- Everything you need to ace your exams
- Clinical Placement
- Human Anatomy
- Intensive Care Nursing
- Mental Health Nursing
- Nursing Management
- Antimicrobial Stewardship
- Audit Compliance Nursing
- Billing Practices for Hospitals
- Biohazard Management
- Budget Management
- Budget Planning
- Capital Resources
- Care Evaluation
- Clinical Pathways
- Communication Skills
- Crisis Management
- Customer Service in Nursing
- Delegation of Nurses
- Disinfection Techniques
- Emergency Drills
- Emergency Preparedness
- Expense Management
- Financial Management in Nursing
- Fiscal Responsibility
- HIPAA Compliance
- Hazard Identification
- Healthcare Technology
- Hospital Asset Management
- Hospital Contract Negotiation
- Hospital Funding Sources
- Hospital Revenue Cycle
- Hygiene Protocols
- Insurance Relations Hospitals
- Interdisciplinary Team
- Labor Relations
- Nurse Staff Training
- Nursing Data Analysis
- Nursing Grant Writing
- Nursing Scheduling
- Operational Efficiency
- Patient Flow
- Patient Loyalty
- Reimbursement Strategies
- Retention Strategies
- Revenue Generation
- Sanitation Practices
- Staff Development
- Staffing Models
- Staffing in Nursing
- Stakeholder Engagement
- Strategic Planning in Nursing
- Time Management
- Waste Disposal in Hospital
- Worker Safety
- Workforce Planning
- Workplace Harmony
- Nursing Theories
- Types of Nursing
Understanding Problem Solving in Nursing Management
Problem solving in nursing management is a crucial process that you need to grasp as a prospective or current nurse. This involves using a logical, systematic approach to resolving issues encountered in a nursing environment, focusing on maintaining quality patient care .
Problem Solving: This is identifying and overcoming obstacles to achieving a goal. In nursing, this generally revolves around improving patient health outcomes and ensuring efficient healthcare facility operations.
Importance of Problem Solving in Nursing Management
Nursing professionals are constantly faced with intricate issues that require decisive and effective solutions. The ability to implement problem-solving is crucial in maintaining optimal patient care , operational efficiency , and fostering team collaboration.
For instance, suppose a sudden shortage of resources like catheters or syringes is experienced in a healthcare facility. In such a case, the nursing manager will need to swiftly solve the problem either by reallocating resources, timely ordering supplies, or finding a temporary alternative, ensuring the patients' needs are continually met.
Key Skills Required for Problem Solving in Nursing Management
Effective problem-solving in nursing management is anchored on a set of key skills. These abilities equip you to navigate complex situations and formulate impactful solutions. They include:
- Critical Thinking: This is your ability to analyse situations in detail and understand their implications.
- Decisiveness: The readiness to make important decisions swiftly and confidently.
- Communication: Sharing and receiving information clearly and effectively.
- Collaboration: Working effectively as part of a team.
These skills are interconnected. For example, your ability to think critically informs your decisiveness. Your decisions are then made clear to your team through effective communication, and together, through collaboration, the problem is solved.
Common Challenges in Problem Solving in Nursing Management
In your nursing management journey, you will come across multiple challenges when attempting to solve problems. These obstacles might occur due to several factors, such as resource limitations, personnel issues, and complex patient needs .
While these challenges can be daunting, equipping yourself with robust problem-solving skills will help you navigate these complications and maintain high standards of patient care.
Scrutinising the Problem Solving Process in Nursing Management
Delving deeper into the problem-solving process in nursing management, you get to navigate its intricacies and mechanisms. This exploration can bolster your abilities to resolve complex situations in your nursing career.
Steps involved in the Problem Solving Process
Problem-solving in nursing management is a multifaceted task that often involves several steps. To understand how to tackle issues expertly, you will need a clear understanding of each stage.
Problem-Solving Process: A systematic approach used to address complications and make decisions. In nursing, it’s composed of several steps, each essential to the resolution of issues.
Here are the key steps:
- Identification: In this stage, you recognise the existence of a problem. It is essential to understand the barriers to your goals and spotlight areas that require improvement.
- Definition: You clearly articulate the problem. By understanding its nuances, magnitude, and implications, you can efficiently tailor a solution.
- Analysis: This involves examining the problem closely from different perspectives, which includes understanding the cause and effect, stakeholders involved, and potential impacts.
- Development of Solutions: Here you brainstorm possible solutions. It's essential to contemplate multiple alternatives to ensure the most effective resolution is chosen.
- Decision Making: In this step, you select the best solution based on the gathered information and analysis. Considerations may include effectiveness, resources needed, and potential side effects.
- Implementation: You put the chosen solution into action, carefully monitoring its effectiveness and making necessary adjustments.
- Evaluation: Finally, you assess the outcome. This helps to determine the effectiveness of your solution and informs future problem-solving efforts.
Neurological Framework for Problem Solving in Nursing Management
Many problem-solving methods exist, but one valuable perspective is through understanding the neurological framework in nursing management. This biological approach delves into how your brain processes information and develops solutions.
Neurological Framework: A biological perspective that explains how a nurse's brain processes, analyses, and responds to problems encountered in the nursing environment.
This framework refers to cognitive processes which involve:
- Critical thinking: This involves actively and skillfully conceptualising, applying, analysing, and evaluating information gathered from observation, experience, reflection, or communication.
- Decision making: This is the cognitive process of selecting a course of action from multiple possibilities. It's based on both intuition and logical reasoning.
- Problem-solving: This involves overcoming hurdles and finding a conclusion, and it usually includes decision-making. It involves creativity and critical thinking to arrive at effective solutions.
Role of Creativity in the Problem Solving Process
Nursing management often involves complex and unique problems. To effectively tackle these challenges, it's crucial to breed creativity in the problem-solving process.
Imagine there's a sudden surge in patient intake due to a local health crisis, resulting in a bed shortage. A creative solution might be to convert other non-critical spaces such as conference rooms temporarily into patient monitoring units, thereby managing the surge effectively.
Importance of Team Collaboration in the Problem Solving Process
In a nursing environment, you are not working in isolation. Collaboration is a critical aspect of problem-solving in nursing management, as diverse insights can lead to innovative and effective solutions.
Consider a scenario where there's a need to implement a new system for managing patient records. To effectively solve potential issues in system implementation, you might need input from various team members including nursing staff, IT specialists, and data management experts. Each member's contribution, based on their expertise and perspective, is crucial in charting a comprehensive problem-solving strategy, ensuring the successful implementation and integration of the new system.
Decision Making and Problem Solving in Nursing Management
Decision making and problem-solving are two interconnected aspects in the realm of nursing management. Understanding their correlation and distinctiveness is key to effectively managing issues and improving patient outcomes in a healthcare setting.
The Interplay between Decision Making and Problem Solving
The connection between decision making and problem solving in nursing management is truly significant. In almost every situation where a problem arises, decision making is an inseparable component of the problem-solving process.
Decision Making in Nursing: This involves selecting a course of action from different alternatives. It is the bridge connecting problem analysis with implementing solutions, and it requires evaluation of information, predicaments, and possible outcomes.
Once you have identified and defined a problem, analysed it, and developed potential solutions, the next step involves decision making. This is where you select the most suitable solution among the alternatives.
For instance, if you are dealing with a bed shortage problem in your healthcare facility, some possible solutions could be outsourcing to other healthcare facilities, using other spaces such as conference rooms as makeshift wards, or deploying portable hospital beds.
Each of these solutions has its pros and cons, and it's here that decision-making skills come into play. You'll need to compare and contrast each option, considering factors like cost, time, resources available, and the overall impact on patient care. The chosen solution is then implemented, and the effects are evaluated for future reference.
Distinguishing Decision Making from Problem Solving in Nursing Management
Though inherently connected, problem solving and decision making are distinct processes within nursing management. Where problem-solving is a comprehensive process that entails identifying, analysing, and solving issues, decision making is a component nested within this process, acting as the transition point from analysis to action.
Problem Solving in Nursing: This is a broader process involving the identification of an issue or obstacle, systematic analysis to understand it, devising potential solutions, choosing the most suitable through decision making, implementing it, and finally reviewing the effectiveness of the implemented solution.
Consider a real-life scenario such as medication errors. If these errors are occurring frequently in your healthcare setup, the problem-solving process will involve identifying the issue (increased medication errors), defining and analysing it (finding the root causes, such as miscommunication or system glitches). This would then lead to brainstorming potential solutions, like improved communication systems or enhanced employee training. The decision-making process would then come into play when choosing the best solution to implement.
Techniques for Effective Decision Making in Problem Solving Scenarios
Effective decision making underpins successful problem solving in nursing management. Implementing the right techniques can enhance your decision-making process, thus leading to more effective problem resolution.
Some proven techniques include:
- Pros and Cons Analysis: List the advantages and disadvantages of each solution to help you visualise the impacts of each decision.
- Decision Matrix: Establish criteria and rate potential solutions. The choice with the highest score is then considered the best decision.
- Cost-Benefit Analysis: Determine the financial implication of each decision and compare it to the benefits. Solutions with a high benefit-cost ratio are preferred.
Working collaboratively to brainstorm and analyse solutions promotes critical thinking and creativity, ensuring that the chosen solution maximises the use of resources and improves patient outcomes .
In unavoidable circumstances where decisions have to be made rapidly and with limited information, using intuition, a nurse's experience, and insights combined with analytical thinking can be beneficial. This is where the balanced blend of clinical expertise and effective risk-taking come into play.
Decision making is never static in nursing management. The cyclic nature of the decision-making process, where outcomes of decisions are continually assessed and feedback is used to improve future decision making, showcases its dynamic and iterative nature. This reinforces the vital role decision making plays in the problem-solving process.
Unpacking Examples of Problem Solving in Nursing Management
By exploring various examples and case studies, you gain a practical view of problem-solving in nursing management. These insights can better equip you to tackle real-life challenges in a healthcare setting.
Case Study Analysis of Problem Solving Scenarios
Case studies provide a thorough view of how problem-solving strategies are applied in various nursing management scenarios. Analysing such cases exposes you to diverse methods and solutions and encourages you to think critically and innovatively.
Case Study Analysis: A detailed examination of a particular instance or event to draw conclusions, develop solutions, or learn from the situation.
Let's investigate a case concerning patient waiting times. In a healthcare facility, it is observed that patients often have to wait for prolonged periods to receive care, leading to dissatisfaction and affecting the overall quality of service. The problem-solving steps might look like this:
- Identification and Definition: The problem is identified as long patient waiting times. It is defined as patients waiting more than 45 minutes to receive care.
- Analysis: The cause of the problem is found to be a shortage of nursing staff during peak hours.
- Development of Solutions: Several possible solutions emerge, such as recruiting additional staff, offering overtime to existing staff, or streamlining operational processes to reduce inefficiencies.
- Decision Making: After careful analysis, it is decided to hire additional part-time staff to handle peak hours.
- Implementation: The recruitment process is initiated and new members integrated into the team.
- Evaluation: After a few months, waiting times are reassessed. A significant reduction is observed, confirming the effectiveness of the solution.
Case study analysis provides a rich source of knowledge and transferable insights that can be helpful in similar or entirely different scenarios. Drawing parallels from varying contexts and understanding how solutions are adapted to unique situations helps bolster your problem-solving skills and adaptability in nursing management.
Varied Approaches to Problem Solving in Different Nursing Scenarios
Different nursing scenarios call for diverse problem-solving strategies. Understanding the varying approaches, from algorithm-based to intuition-driven, equips you to manage multidimensional and intricate issues effectively.
Algorithm-based Approach: This involves following a clearly defined set of rules or procedures to solve a problem. It can be applicable in situations with defined parameters and scope, such as diagnosing a health condition based on a specific set of symptoms.
Intuition-driven Approach: This combines a nurse's experience, knowledge, and instinct to solve a problem. It applies to ambiguous scenarios where conventional rules may not be applicable, such as managing a patient's fear or anxiety.
Problem-solving in nursing management is all about adapting to the environment and the situation. The right approach may vary, calling for flexibility, creativity, critical thinking, and a deep understanding of the issue for successful resolution.
Real Life Applications of Problem Solving Strategies in Nursing Management
The real world of nursing is complex and dynamic, and various problem-solving strategies can apply on any given day. To navigate smoothly, you need to understand how the various approaches can be adapted to specific situations.
Consider solving a recurrent communication issue within your nursing team. The algorithmic approach might involve establishing clear communication protocols or using digital tools to streamline interaction. However, the intuition-driven approach might involve informal team-building meetings to foster better personal connections. In this situation, the best solution might be a blend of the two approaches to ensure both procedural clarity and improved team relationships.
The key takeaway here is that there is no "one-size-fits-all" solution in nursing management. Problem-solving requires flexibility, openness, and the ability to judge which strategy will perform best in a particular scenario.
Exploring Nursing Management Problem-Solving Strategies
Problem-solving strategies in nursing management form the backbone of effective healthcare services. By ensuring that nursing personnel can tackle issues with aplomb and proficiency, these strategies contribute significantly to patient satisfaction and positive outcomes.
Development of Strategic Problem-Solving Competencies
The first step towards demystifying problem-solving processes in nursing management is the development of strategic problem-solving competencies. The journey from novice to expert involves honing these skills and integrating them into your practical work.
Strategic Problem-Solving Competencies: These are a set of core skills that facilitate effective problem-solving in nursing management, including critical thinking, innovative thinking, collaboration, adaptability, leadership, and decision-making.
Acquiring these skills involves both academic learning and practical experiences. Gaining theoretical knowledge lays the foundation, while integrating this knowledge within a clinical context enriches and refines these competencies.
- Critical Thinking: This involves analysing situations from multiple perspectives, evaluating different solutions, and making informed decisions.
- Innovative Thinking: Innovative thinking pertains to thinking outside the box, especially when conventional solutions are inadequate.
- Collaboration: In nursing, effective problem-solving often requires collaborative efforts, valuing diverse ideas and working towards common goals.
- Adaptability: Healthcare settings are continually changing, and the ability to swiftly adapt to new situations is crucial.
- Leadership: Good leadership skills facilitate effective management of teams and ensuring that everyone is following the established problem-solving process.
- Decision Making: Ability to implement effective decisions is vital for successful problem solving.
Role of Leadership in Implementing Problem Solving Strategies
The role of leadership in implementing problem-solving strategies must not be understated. Effective leadership not only guides teams through problem-solving processes but also fosters a supportive environment where team members feel safe to contribute ideas and question assumptions.
Leadership in Nursing: This involves guiding, motivating, and supporting nursing staff to deliver quality healthcare services. Also, it encompasses enhancing team cooperation, improving communication, and fostering a culture of continuous learning.
Leadership employs a variety of approaches in implementing problem-solving strategies. Different leadership styles can be applied based on the nature of the problem and the team dynamics. Transformational leadership, for instance, inspires others to exceed their personal goals and work for a collective purpose. On the other hand, participative leadership encourages open discussions and collective decision-making, promoting a more inclusive and democratic problem-solving process.
Leadership is also instrumental in creating an environment that encourages the sharing of problems openly, without fear of judgment, hence facilitating early identification and efficient resolution of issues. By also ensuring that learning opportunities are provided to enhance team problem-solving capabilities, leadership positively influences problem-solving outcomes.
Use of Resources in Problem Solving Strategies
Effective resource utilization is a critical component of successful problem-solving strategies in nursing management. The term 'resources' in this context includes human resources such as nursing staff and doctors, as well as material resources like medical supplies, equipment, and facilities.
Resource Utilisation: This refers to the efficient and effective use of available resources to achieve desired outcomes. In nursing, it involves ensuring that staff, equipment, and supplies are optimally used to deliver quality healthcare services and solve arising problems.
Problem-solving often necessitates the optimal use of available resources. For example, if there is an issue of high patient-to-nurse ratio, one of the possible solutions could be redistributing nursing staff according to workload and patient needs, or hiring additional staff if finances permit.
Every solution should be weighed based on its resource implications. The best solution is often the one that optimally utilises available resources to provide the maximum benefit. For example, while hiring additional staff might solve the problem, it might not be the best solution if the budget is very limited. In such a case, reallocation of existing staff may be a more practical solution.
Similarly, if there is a shortage of a particular supply, then alternatives may need to be sought, or rationing implemented. A critical analysis of such situations is necessary to ensure that the solutions proposed and implemented do not create other problems related to resource allocation and use.
It's also important to remember to continuously evaluate the impact of your solutions on resource utilisation. This will not only help you ensure sustainable use of resources but also contribute to continuous improvement in problem-solving strategies.
Understanding the stages of problem-solving in nursing practice is fundamental to addressing various challenges that arise in the healthcare sector. These problem-solving stages enable you to identify issues, create and implement solutions, and review the outcomes for improvement purposes.
Initial Assessment and Identification: The First Stage of Problem Solving
The initial phase of problem-solving in nursing management involves the assessment and identification of the issue at hand. This stage is critical as the correct identification of the problem lays the foundation for effective solution design and implementation.
Initial Assessment: This is the preliminary evaluation of the situation, leading to the recognition of existing problems. This stage involves observation, questioning, and data gathering to understand the issue better.
This initial step requires keen observation skills and critical thinking. While observation helps in gathering relevant details, critical thinking enables you to scrutinize this information and identify potential problems. You could also use feedback from your team and other relevant stakeholders to gain a comprehensive understanding of the issue.
For instance, suppose you discover unusually high levels of patient discomfort during specific hours. The initial assessment might involve examining patient records during these hours, observing nursing practices in these time frames, and seeking feedback from both patients and nursing staff. This comprehensive approach could potentially reveal the issue, like a shortage of staff during peak hours, leading to delayed or inefficient care.
Formulating Actionable Solutions: The Mid Stages of the Problem-solving Process
Once the problem is identified, the next phase is generating actionable solutions. The validity and effectiveness of these solutions significantly influence the problem-solving process's success, thus necessitating careful deliberation and thorough evaluation.
Actionable Solution: A practical, feasible strategy that can be implemented to resolve the problem. It's typically developed through brainstorming, analysis, and evaluation of various alternatives.
The process of formulating actionable solutions involves brainstorming potential remedies, evaluating these against a set criteria, and choosing the most viable option. Ideally, this should be a collaborative effort involving all relevant stakeholders. Collaborative problem-solving encourages diversity in ideas and promotes inclusivity.
Innovation is a key driver in formulating actionable solutions. Traditional problem-solving methods might fail in the face of complex or unique problems, necessitating innovative ideas. Remember, the most effective solutions often result from 'thinking outside the box'.
Evaluation and Reflection: The Final Stage of Problem Solving
The final stage of problem-solving is evaluation and reflection. After implementing the chosen solution, it is essential to assess its effectiveness in solving the identified problem. This stage offers an opportunity to learn from the implemented action and make necessary adjustments for future improvement.
Evaluation and Reflection: This stage involves reviewing the implemented solution to assess its effectiveness. Reflection involves learning from the process and experiences to ensure continuous improvement.
To achieve meaningful evaluation and reflection, a systematic approach must be adopted. Begin with the assessment of the effect of the solution on the original problem. Have the waiting times reduced following the staff adjustments? Is there an improved level of patient comfort? These are the kind of questions you need to address.
Following the evaluation, it's crucial to reflect on the entire process. Consider what worked well and what didn't. Reflecting on these experiences offers valuable insights that can be used to improve future problem-solving processes.
Take the earlier example of high levels of patient discomfort due to staff shortage during peak hours. Suppose, after implementing the solution of adjusting staff schedules, you find that there's a significant improvement in patient comfort levels. This shows that your solution worked. However, during reflection, you realise that the process took more time than necessary due to delayed decision-making. For future improvement, you could consider setting specific timelines for each stage of the problem-solving process.
In conclusion, problem-solving is a cyclical process. It doesn't end with implementing a solution; instead, it opens doors for continuous learning and improvement. Adapting to this cycle is key to honing your problem-solving proficiency in nursing management.
Critical Thinking and Problem Solving in Nursing
Problem solving in nursing management is underpinned by the practice of critical thinking. An understanding of the delicate interplay between these two capabilities is central to the enhancement of nursing management and the ultimate delivery of efficient patient care.
The Connection Between Critical Thinking and Problem Solving in Nursing
There is a strong relationship between critical thinking and problem solving in nursing, evidenced by the significant role each plays in the healthcare sector. Critical thinking provides the foundation upon which problem-solving strategies are built.
Critical Thinking: This is the disciplined process of analysing, interpreting, evaluating, and drawing conclusions from varying levels of data, information or experiences. It involves a deeper level of thinking to understand, evaluate and resolve complex issues or situations.
The process of problem-solving often begins with an evaluation of the situation, gathering data, appraising the data, and coming with strategic solutions. By applying critical thinking, you can get a clear understanding of the problem, which helps devise more effective solutions.
For example, in implementing new protocols in a nursing unit, critical thinking may involve evaluating the necessity of the change, the potential effect on the nursing staff’s workflow, and patient care. The ability to think critically facilitates well-informed decisions, thereby enhancing the problem-solving process.
Beyond problem identification and solution generation, critical thinking is also instrumental in the review phase of the problem-solving process. It allows you to reflect on the effectiveness of implemented solutions, the overall process, and areas that could be improved. Therefore, the integration of critical thinking not only enriches problem-solving but also contributes to continuous learning and improvement in nursing management.
Enhancing Critical Thinking for Effective Problem Solving in Nursing Management
Enhancing critical thinking skills in the nursing workforce enriches problem-solving efforts and ultimately results in improved patient outcomes and service delivery. This strengthening could be achieved through several strategies.
Enhancing Critical Thinking: The process of improving critical thinking skills to enhance one's ability to evaluate complex situations effectively and make informed decisions.
Firstly, continuous learning and professional development activities such as workshops, seminars, and online courses can provide essential tools for sharpening critical thinking skills.
Secondly, fostering a culture of open communication and collaborative problem-solving offers great benefits. These platforms facilitate the sharing of diverse perspectives, promoting deep analyses, and enriching the problem-solving process.
Lastly, reflective practice can also positively impact critical thinking abilities. Regular reflection on your practice, experiences, and learnings enables you to identify gaps in your thinking and areas of improvement. It encourages a deeper level of thinking that enriches the problem-solving process.
- Continuous learning and participation in professional development activities.
- Fostering a culture of open communication and collaborative problem-solving.
- Engaging in reflective practice regularly.
Examples of Critical Thinking Leading to Effective Problem Solving
The application of critical thinking skills often results in improved problem-solving outcomes in nursing management. Several instances illustrate this relationship.
For instance, consider a situation where a nursing unit has seen a significant increase in medication errors. The nursing manager applies critical thinking to evaluate the situation, identify potential causes, and devise solutions. Through an in-depth review of pharmaceutical administration procedures, team collaboration, discussion, and data evaluation, the nursing manager identifies the root cause - an overly complicated method of logging medication.
Armed with this information, they innovate a simpler, more effective system. By cutting down on needless complexity, the nursing unit sees a drastic decrease in medication errors. This example shows how the application of critical thinking streamlined a complex process, providing an effective solution to the problem at hand.
Another instance could be changing patient demographics, with more elderly patients requiring care. A nursing manager applies critical thinking to understand the unique needs of these patients and the potential challenges that might arise in catering to these needs. As a result, they develop tailored care plans and training programmes for the nursing staff to better care for elderly patients, resulting in improved patient satisfaction.
These examples highlight how critical thinking can lead to effective problem solving in nursing management, ultimately resulting in better service delivery and patient care. Therefore, enhancing critical thinking should be seen as a vital strategy for improving problem-solving proficiency in nursing management.
Problem Solving in Nursing Management - Key takeaways
- Problem Solving in Nursing Management: It is a thorough process involving the identification, analysis, and (de)cision-making to solve issues in nursing management. It also includes implementation and review of the effectiveness of the solutions.
- Decision Making Techniques: Different techniques such as Pros and Cons Analysis, Decision Matrix, and Cost-Benefit Analysis can enhance the decision-making process in problem-solving scenarios.
- Case Study Analysis: It involves the detailed examination of various scenarios to inform problem-solving strategies and practice.
- Approaches to Problem-Solving: Different approaches may apply in different nursing scenarios, such as the algorithm-based approach for well-defined scenarios and the intuition-driven approach for ambiguous situations.
- Strategic Problem-Solving Competencies: These are essential skills including critical thinking, innovative thinking, collaboration, adaptability, leadership, and decision-making, crucial in effective problem-solving.
- Leadership in Nursing: Leadership plays a key role in guiding, motivating, and supporting nursing staff. It influences the successful implementation of problem-solving strategies.
- Resource Utilisation: Efficient and effective use of available resources, such as nursing staff, equipment, and supplies, is vital in problem-solving in nursing management.
- Stages of Problem Solving in Nursing Practice: The stages include the identification, analysis, and resolution of problems, which are crucial in responding to challenges in the healthcare sector.
Flashcards inProblem Solving in Nursing Management 14
What is the significance of problem-solving in nursing management?
Problem-solving in nursing management is crucial in maintaining optimal patient care, operational efficiency, and fostering team collaboration by resolving intricate issues with decisive and effective solutions.
What are the key skills required for effective problem-solving in nursing management?
The key skills required are critical thinking, decisiveness, communication, and collaboration. Each skill is interconnected and helps in formulating impactful solutions.
What are the key steps involved in the problem-solving process in nursing management?
The key steps are identification, definition, analysis, development of solutions, decision making, implementation, and evaluation.
What does the neurological framework in nursing management involve?
This framework involves cognitive processes such as critical thinking, decision making, and problem-solving.
What is decision making in nursing management?
This involves selecting a course of action from different alternatives. It acts as a bridge, connecting problem analysis with implementing solutions and requires evaluation of information, predicaments, and possible outcomes.
What is problem solving in nursing management and how is it different from decision making?
Problem solving is a broader process involving the identification of an issue, systematic analysis to understand it, devising potential solutions, choosing the most suitable through decision making, implementing it, and finally reviewing the effectiveness of the implemented solution. Decision making, on the other hand, is a component nested within this process.
Learn with 14 Problem Solving in Nursing Management flashcards in the free StudySmarter app
We have 14,000 flashcards about Dynamic Landscapes.
Already have an account? Log in
Frequently Asked Questions about Problem Solving in Nursing Management
Test your knowledge with multiple choice flashcards.
Join the StudySmarter App and learn efficiently with millions of flashcards and more!
Keep learning, you are doing great.
About StudySmarter
StudySmarter is a globally recognized educational technology company, offering a holistic learning platform designed for students of all ages and educational levels. Our platform provides learning support for a wide range of subjects, including STEM, Social Sciences, and Languages and also helps students to successfully master various tests and exams worldwide, such as GCSE, A Level, SAT, ACT, Abitur, and more. We offer an extensive library of learning materials, including interactive flashcards, comprehensive textbook solutions, and detailed explanations. The cutting-edge technology and tools we provide help students create their own learning materials. StudySmarter’s content is not only expert-verified but also regularly updated to ensure accuracy and relevance.

StudySmarter Editorial Team
Team Problem Solving in Nursing Management Teachers
- 25 minutes reading time
- Checked by StudySmarter Editorial Team
Study anywhere. Anytime.Across all devices.
Create a free account to save this explanation..
Save explanations to your personalised space and access them anytime, anywhere!
By signing up, you agree to the Terms and Conditions and the Privacy Policy of StudySmarter.
Sign up to highlight and take notes. It’s 100% free.
Join over 22 million students in learning with our StudySmarter App
The first learning app that truly has everything you need to ace your exams in one place
- Flashcards & Quizzes
- AI Study Assistant
- Study Planner
- Smart Note-Taking
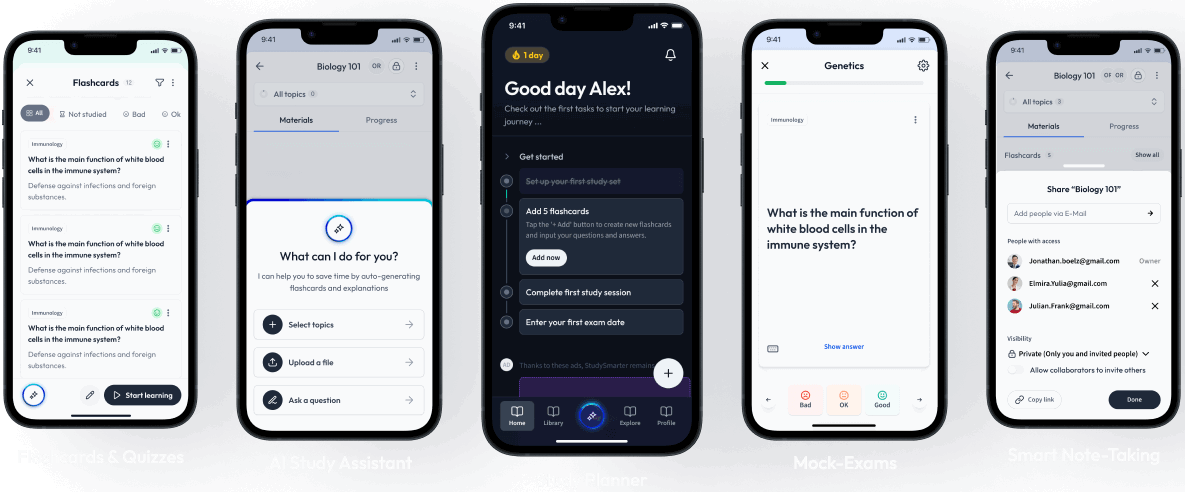
- Number of visits 5856
- Number of saves 32
Applying the Scientific Method to Solve a Nursing Problem (Remix)
- Report this resource
Description

Wyoming Standards for English Language Arts
Learning Domain: Reading for Informational Text
Standard: Integrate and evaluate multiple sources of information presented in different media or formats (e.g., visually, quantitatively) as well as in words in order to address a question or solve a problem.
Degree of Alignment: Not Rated (0 users)
Learning Domain: Reading for Literacy in Science and Technical Subjects
Standard: Follow precisely a complex multistep procedure when carrying out experiments, taking measurements, or performing technical tasks; analyze the specific results based on explanations in the text.
Learning Domain: Speaking and Listening
Standard: Present information, findings, and supporting evidence, conveying a clear and distinct perspective, such that listeners can follow the line of reasoning, alternative or opposing perspectives are addressed, and the organization, development, substance, and style are appropriate to purpose, audience, and a range or formal and informal tasks.
Maryland College and Career Ready English Language Arts Standards
Common core state standards english language arts.
Cluster: Integration of Knowledge and Ideas.
Cluster: Presentation of Knowledge and Ideas.
Cluster: Key Ideas and Details.
Evaluations
No evaluations yet.
- Adult Education
- Applied Science
- Designers for Learning
- Nursing Process
- Scientific Method
- Communication Skills
Review Criteria

IMAGES
VIDEO
COMMENTS
Nurses can implement the original nursing process to guide patient care for problem solving in nursing. These steps include: Assessment. Use critical thinking skills to brainstorm and gather information. Diagnosis. Identify the problem and any triggers or obstacles. Planning. Collaborate to formulate the desired outcome based on proven methods ...
Nicholas McGowan, BSN, RN, CCRN, has been a critical care nurse for 10 years in neurological trauma nursing and cardiovascular and surgical intensive care. He defines critical thinking as "necessary for problem-solving and decision-making by healthcare providers.
Nurse leaders perceive their role as a problem-solver, which is a necessary step in advocacy. 27 Problem-solving is a process that contains the elements of decision-making and critical thinking. 28. The theory that emerged from the core categories explicitly focused on the central phenomenon of LHV in the nursing work environment.
• Discuss 7 steps to problem-solving. Introduction As medicine becomes more and more complex and nursing responsibilities increase, critical thinking—the ability to question and make rational decisions—becomes even more important. Too often, healthcare providers simply follow routines and accept the word of
The following are examples of attributes of excellent critical thinking skills in nursing. 1. The ability to interpret information: In nursing, the interpretation of patient data is an essential part of critical thinking. Nurses must determine the significance of vital signs, lab values, and data associated with physical assessment.
To solve a problem you need to generate solutions. However, the obvious solution may not necessarily be the best. To generate solutions, a mixture of creative and analytical thinking is needed (Bransford, 1993). Creativity is about escaping from preconceived ideas that block the way to finding an innovative solution to a problem.
Conclusion. The influencing factors of clinical nurses' problem-solving dilemma are diverse. Hospital managers and nursing educators should pay attention to the problem-solving of clinical nurses, carry out a series of training and counselling of nurses by using the method of situational simulation, optimize the nursing management mode, learn to use new media technology to improve the ...
Background. Problem solving involves recognizing the difference between the problem solver's current state and the goal state to be reached, and resolving the obstacles that prevent them from achieving the goal [].Acquiring problem-solving ability based on judgment and critical thinking is an important element of nursing education [].Furthermore, the use of effective problem-solving ...
Critical thinking is applied by nurses in the process of solving problems of patients and decision-making process with creativity to enhance the effect. It is an essential process for a safe, efficient and skillful nursing intervention. Critical thinking according to Scriven and Paul is the mental active process and subtle perception, analysis ...
This paper analyses the role of problem solving in nursing practice including the process, acquisition and measurement of problem-solving skills It is argued that while problem-solving ability is acknowledged as critical if today's nurse practitioner is to maintain effective clinical practice, to date it retains a marginal place in nurse education curricula Further, it has attracted limited ...
Abstract. This paper reviews the literature surrounding the research on how individuals solve problems. The purpose of the review is to heighten awareness amongst nurses in general, and nurse academics in particular about the theories developed, approaches taken and conclusions reached on how clinicians problem-solve.
Problem solving for nurses is essential to quality patient care. Explore problem-solving examples in nursing and devise effective strategies.
For example, treating immediate symptoms may temporarily solve a problem, but determining the underlying cause of the symptoms is the key to effective long-term health. 8 Examples of Critical Thinking in Nursing. Here are some real-life examples of how nurses apply critical thinking on the job every day, as told by nurses themselves.
Abstract. Problem solving in clinical nursing practice is the essence of good care delivery. This paper gives an overview of a research study which identified the cognitive problem solving process nurses use while delivering care. The study was conducted in the clinical setting and used a qualitative research methodology of observation ...
Step 2: Analyze the Problem. Break down the problem to get an understanding of the problem. Determine how the problem developed. Determine the impact of the problem. Step 3: Develop Solutions. Brainstorm and list all possible solutions that focus on resolving the identified problem. Do not eliminate any possible solutions at this stage.
A diagram of the clinical reasoning framework is shown in Figure 1. In this diagram the cycle begins at 1200 hours and moves in a clockwise direction. The circle represents the ongoing and cyclical nature of clinical interventions and the importance of evaluation and reflection. There are eight main steps or phases in the clinical reasoning cycle.
Problem solving is a focus of nursing practice and of great importance for raising the quality of patient care. Constructive problem-solving skills affect cognitive empathy skills. Educational level and career length were found to relate negatively and level of self-confidence was found to relate positively with level of cognitive empathy ...
Abstract. This paper analyses the role of problem solving in nursing practice including the process, acquisition and measurement of problem-solving skills. It is argued that while problem-solving ability is acknowledged as critical if today's nurse practitioner is to maintain effective clinical practice, to date it retains a marginal place in ...
Critical Thinking and Nursing Care Plans Go Together Like Chicken and Waffles Critical Thinking in Nursing: Example 1. I had a patient that was scheduled to go to get a pacemaker placed at 0900. The physician wanted the patient to get 2 units of blood before going downstairs for the procedure. I administered it per protocol.
2.1. Study Design. To create and analyze the structural model for clinical nurses' communication skills, problem-solving ability, understanding of patients' conditions, and nurse's perception of professionalism, the theoretical relationships among the variables were developed based on related theories.
We use problem-solving approach in daily activities and nursing practice. For example, you use problem solving in deciding what to wear, when it is raining or while nursing a tracheotomy patient how to communicate. The nursing process is a subset of problem solving process (see Fig. 4.1). You have already
Problem Solving in Nursing: This is a broader process involving the identification of an issue or obstacle, systematic analysis to understand it, devising potential solutions, choosing the most suitable through decision making, implementing it, and finally reviewing the effectiveness of the implemented solution.
The purpose of this lesson is for adult learners to improve their communication skills --- specifically reading, writing, speaking and listening --- by using the Scientific Method to solve a nursing problem. The target audience of this lesson is adults at the 12th grade reading and writing levels. This lesson is designed for a face-to-face ...