- Search the site GO Please fill out this field.
- Newsletters
- Mental Health
- Social and Public Health

What Is Gender Affirmation Surgery?
:max_bytes(150000):strip_icc():format(webp)/KP-Headshot-IMG_1661-0d48c6ea46f14ab19a91e7b121b49f59.jpg)
A gender affirmation surgery allows individuals, such as those who identify as transgender or nonbinary, to change one or more of their sex characteristics. This type of procedure offers a person the opportunity to have features that align with their gender identity.
For example, this type of surgery may be a transgender surgery like a male-to-female or female-to-male surgery. Read on to learn more about what masculinizing, feminizing, and gender-nullification surgeries may involve, including potential risks and complications.
Why Is Gender Affirmation Surgery Performed?
A person may have gender affirmation surgery for different reasons. They may choose to have the surgery so their physical features and functional ability align more closely with their gender identity.
For example, one study found that 48,019 people underwent gender affirmation surgeries between 2016 and 2020. Most procedures were breast- and chest-related, while the remaining procedures concerned genital reconstruction or facial and cosmetic procedures.
In some cases, surgery may be medically necessary to treat dysphoria. Dysphoria refers to the distress that transgender people may experience when their gender identity doesn't match their sex assigned at birth. One study found that people with gender dysphoria who had gender affirmation surgeries experienced:
- Decreased antidepressant use
- Decreased anxiety, depression, and suicidal ideation
- Decreased alcohol and drug abuse
However, these surgeries are only performed if appropriate for a person's case. The appropriateness comes about as a result of consultations with mental health professionals and healthcare providers.
Transgender vs Nonbinary
Transgender and nonbinary people can get gender affirmation surgeries. However, there are some key ways that these gender identities differ.
Transgender is a term that refers to people who have gender identities that aren't the same as their assigned sex at birth. Identifying as nonbinary means that a person doesn't identify only as a man or a woman. A nonbinary individual may consider themselves to be:
- Both a man and a woman
- Neither a man nor a woman
- An identity between or beyond a man or a woman
Hormone Therapy
Gender-affirming hormone therapy uses sex hormones and hormone blockers to help align the person's physical appearance with their gender identity. For example, some people may take masculinizing hormones.
"They start growing hair, their voice deepens, they get more muscle mass," Heidi Wittenberg, MD , medical director of the Gender Institute at Saint Francis Memorial Hospital in San Francisco and director of MoZaic Care Inc., which specializes in gender-related genital, urinary, and pelvic surgeries, told Health .
Types of hormone therapy include:
- Masculinizing hormone therapy uses testosterone. This helps to suppress the menstrual cycle, grow facial and body hair, increase muscle mass, and promote other male secondary sex characteristics.
- Feminizing hormone therapy includes estrogens and testosterone blockers. These medications promote breast growth, slow the growth of body and facial hair, increase body fat, shrink the testicles, and decrease erectile function.
- Non-binary hormone therapy is typically tailored to the individual and may include female or male sex hormones and/or hormone blockers.
It can include oral or topical medications, injections, a patch you wear on your skin, or a drug implant. The therapy is also typically recommended before gender affirmation surgery unless hormone therapy is medically contraindicated or not desired by the individual.
Masculinizing Surgeries
Masculinizing surgeries can include top surgery, bottom surgery, or both. Common trans male surgeries include:
- Chest masculinization (breast tissue removal and areola and nipple repositioning/reshaping)
- Hysterectomy (uterus removal)
- Metoidioplasty (lengthening the clitoris and possibly extending the urethra)
- Oophorectomy (ovary removal)
- Phalloplasty (surgery to create a penis)
- Scrotoplasty (surgery to create a scrotum)
Top Surgery
Chest masculinization surgery, or top surgery, often involves removing breast tissue and reshaping the areola and nipple. There are two main types of chest masculinization surgeries:
- Double-incision approach : Used to remove moderate to large amounts of breast tissue, this surgery involves two horizontal incisions below the breast to remove breast tissue and accentuate the contours of pectoral muscles. The nipples and areolas are removed and, in many cases, resized, reshaped, and replaced.
- Short scar top surgery : For people with smaller breasts and firm skin, the procedure involves a small incision along the lower half of the areola to remove breast tissue. The nipple and areola may be resized before closing the incision.
Metoidioplasty
Some trans men elect to do metoidioplasty, also called a meta, which involves lengthening the clitoris to create a small penis. Both a penis and a clitoris are made of the same type of tissue and experience similar sensations.
Before metoidioplasty, testosterone therapy may be used to enlarge the clitoris. The procedure can be completed in one surgery, which may also include:
- Constructing a glans (head) to look more like a penis
- Extending the urethra (the tube urine passes through), which allows the person to urinate while standing
- Creating a scrotum (scrotoplasty) from labia majora tissue
Phalloplasty
Other trans men opt for phalloplasty to give them a phallic structure (penis) with sensation. Phalloplasty typically requires several procedures but results in a larger penis than metoidioplasty.
The first and most challenging step is to harvest tissue from another part of the body, often the forearm or back, along with an artery and vein or two, to create the phallus, Nicholas Kim, MD, assistant professor in the division of plastic and reconstructive surgery in the department of surgery at the University of Minnesota Medical School in Minneapolis, told Health .
Those structures are reconnected under an operative microscope using very fine sutures—"thinner than our hair," said Dr. Kim. That surgery alone can take six to eight hours, he added.
In a separate operation, called urethral reconstruction, the surgeons connect the urinary system to the new structure so that urine can pass through it, said Dr. Kim. Urethral reconstruction, however, has a high rate of complications, which include fistulas or strictures.
According to Dr. Kim, some trans men prefer to skip that step, especially if standing to urinate is not a priority. People who want to have penetrative sex will also need prosthesis implant surgery.
Hysterectomy and Oophorectomy
Masculinizing surgery often includes the removal of the uterus (hysterectomy) and ovaries (oophorectomy). People may want a hysterectomy to address their dysphoria, said Dr. Wittenberg, and it may be necessary if their gender-affirming surgery involves removing the vagina.
Many also opt for an oophorectomy to remove the ovaries, almond-shaped organs on either side of the uterus that contain eggs and produce female sex hormones. In this case, oocytes (eggs) can be extracted and stored for a future surrogate pregnancy, if desired. However, this is a highly personal decision, and some trans men choose to keep their uterus to preserve fertility.
Feminizing Surgeries
Surgeries are often used to feminize facial features, enhance breast size and shape, reduce the size of an Adam’s apple , and reconstruct genitals. Feminizing surgeries can include:
- Breast augmentation
- Facial feminization surgery
- Penis removal (penectomy)
- Scrotum removal (scrotectomy)
- Testicle removal (orchiectomy)
- Tracheal shave (chondrolaryngoplasty) to reduce an Adam's apple
- Vaginoplasty
- Voice feminization
Breast Augmentation
Top surgery, also known as breast augmentation or breast mammoplasty, is often used to increase breast size for a more feminine appearance. The procedure can involve placing breast implants, tissue expanders, or fat from other parts of the body under the chest tissue.
Breast augmentation can significantly improve gender dysphoria. Studies show most people who undergo top surgery are happier, more satisfied with their chest, and would undergo the surgery again.
Most surgeons recommend 12 months of feminizing hormone therapy before breast augmentation. Since hormone therapy itself can lead to breast tissue development, transgender women may or may not decide to have surgical breast augmentation.
Facial Feminization and Adam's Apple Removal
Facial feminization surgery (FFS) is a series of plastic surgery procedures that reshape the forehead, hairline, eyebrows, nose, cheeks, and jawline. Nonsurgical treatments like cosmetic fillers, botox, fat grafting, and liposuction may also be used to create a more feminine appearance.
Some trans women opt for chondrolaryngoplasty, also known as a tracheal shave. The procedure reduces the size of the Adam's apple, an area of cartilage around the larynx (voice box) that tends to be larger in people assigned male at birth.
Vulvoplasty and Vaginoplasty
As for bottom surgery, there are various feminizing procedures from which to choose. Vulvoplasty (to create external genitalia without a vagina) or vaginoplasty (to create a vulva and vaginal canal) are two of the most common procedures.
Dr. Wittenberg noted that people might undergo six to 12 months of electrolysis or laser hair removal before surgery to remove pubic hair from the skin that will be used for the vaginal lining.
Surgeons have different techniques for creating a vaginal canal. A common one is a penile inversion, where the masculine structures are emptied and inverted into a created cavity, explained Dr. Kim. Vaginoplasty may be done in one or two stages, said Dr. Wittenberg, and the initial recovery is three months—but it will be a full year until people see results.
Surgical removal of the penis or penectomy is sometimes used in feminization treatment. This can be performed along with an orchiectomy and scrotectomy.
However, a total penectomy is not commonly used in feminizing surgeries . Instead, many people opt for penile-inversion surgery, a technique that hollows out the penis and repurposes the tissue to create a vagina during vaginoplasty.
Orchiectomy and Scrotectomy
An orchiectomy is a surgery to remove the testicles —male reproductive organs that produce sperm. Scrotectomy is surgery to remove the scrotum, that sac just below the penis that holds the testicles.
However, some people opt to retain the scrotum. Scrotum skin can be used in vulvoplasty or vaginoplasty, surgeries to construct a vulva or vagina.
Other Surgical Options
Some gender non-conforming people opt for other types of surgeries. This can include:
- Gender nullification procedures
- Penile preservation vaginoplasty
- Vaginal preservation phalloplasty
Gender Nullification
People who are agender or asexual may opt for gender nullification, sometimes called nullo. This involves the removal of all sex organs. The external genitalia is removed, leaving an opening for urine to pass and creating a smooth transition from the abdomen to the groin.
Depending on the person's sex assigned at birth, nullification surgeries can include:
- Breast tissue removal
- Nipple and areola augmentation or removal
Penile Preservation Vaginoplasty
Some gender non-conforming people assigned male at birth want a vagina but also want to preserve their penis, said Dr. Wittenberg. Often, that involves taking skin from the lining of the abdomen to create a vagina with full depth.
Vaginal Preservation Phalloplasty
Alternatively, a patient assigned female at birth can undergo phalloplasty (surgery to create a penis) and retain the vaginal opening. Known as vaginal preservation phalloplasty, it is often used as a way to resolve gender dysphoria while retaining fertility.
The recovery time for a gender affirmation surgery will depend on the type of surgery performed. For example, healing for facial surgeries may last for weeks, while transmasculine bottom surgery healing may take months.
Your recovery process may also include additional treatments or therapies. Mental health support and pelvic floor physiotherapy are a few options that may be needed or desired during recovery.
Risks and Complications
The risk and complications of gender affirmation surgeries will vary depending on which surgeries you have. Common risks across procedures could include:
- Anesthesia risks
- Hematoma, which is bad bruising
- Poor incision healing
Complications from these procedures may be:
- Acute kidney injury
- Blood transfusion
- Deep vein thrombosis, which is blood clot formation
- Pulmonary embolism, blood vessel blockage for vessels going to the lung
- Rectovaginal fistula, which is a connection between two body parts—in this case, the rectum and vagina
- Surgical site infection
- Urethral stricture or stenosis, which is when the urethra narrows
- Urinary tract infection (UTI)
- Wound disruption
What To Consider
It's important to note that an individual does not need surgery to transition. If the person has surgery, it is usually only one part of the transition process.
There's also psychotherapy . People may find it helpful to work through the negative mental health effects of dysphoria. Typically, people seeking gender affirmation surgery must be evaluated by a qualified mental health professional to obtain a referral.
Some people may find that living in their preferred gender is all that's needed to ease their dysphoria. Doing so for one full year prior is a prerequisite for many surgeries.
All in all, the entire transition process—living as your identified gender, obtaining mental health referrals, getting insurance approvals, taking hormones, going through hair removal, and having various surgeries—can take years, healthcare providers explained.
A Quick Review
Whether you're in the process of transitioning or supporting someone who is, it's important to be informed about gender affirmation surgeries. Gender affirmation procedures often involve multiple surgeries, which can be masculinizing, feminizing, or gender-nullifying in nature.
It is a highly personalized process that looks different for each person and can often take several months or years. The procedures also vary regarding risks and complications, so consultations with healthcare providers and mental health professionals are essential before having these procedures.
American Society of Plastic Surgeons. Gender affirmation surgeries .
Wright JD, Chen L, Suzuki Y, Matsuo K, Hershman DL. National estimates of gender-affirming surgery in the US . JAMA Netw Open . 2023;6(8):e2330348-e2330348. doi:10.1001/jamanetworkopen.2023.30348
Coleman E, Radix AE, Bouman WP, et al. Standards of care for the health of transgender and gender diverse people, version 8 . Int J Transgend Health . 2022;23(S1):S1-S260. doi:10.1080/26895269.2022.2100644
Chou J, Kilmer LH, Campbell CA, DeGeorge BR, Stranix JY. Gender-affirming surgery improves mental health outcomes and decreases anti-depressant use in patients with gender dysphoria . Plast Reconstr Surg Glob Open . 2023;11(6 Suppl):1. doi:10.1097/01.GOX.0000944280.62632.8c
Human Rights Campaign. Get the facts on gender-affirming care .
Human Rights Campaign. Transgender and non-binary people FAQ .
Unger CA. Hormone therapy for transgender patients . Transl Androl Urol . 2016;5(6):877–84. doi:10.21037/tau.2016.09.04
Richards JE, Hawley RS. Chapter 8: Sex Determination: How Genes Determine a Developmental Choice . In: Richards JE, Hawley RS, eds. The Human Genome . 3rd ed. Academic Press; 2011: 273-298.
Randolph JF Jr. Gender-affirming hormone therapy for transgender females . Clin Obstet Gynecol . 2018;61(4):705-721. doi:10.1097/GRF.0000000000000396
Cocchetti C, Ristori J, Romani A, Maggi M, Fisher AD. Hormonal treatment strategies tailored to non-binary transgender individuals . J Clin Med . 2020;9(6):1609. doi:10.3390/jcm9061609
Van Boerum MS, Salibian AA, Bluebond-Langner R, Agarwal C. Chest and facial surgery for the transgender patient . Transl Androl Urol . 2019;8(3):219-227. doi:10.21037/tau.2019.06.18
Djordjevic ML, Stojanovic B, Bizic M. Metoidioplasty: techniques and outcomes . Transl Androl Urol . 2019;8(3):248–53. doi:10.21037/tau.2019.06.12
Bordas N, Stojanovic B, Bizic M, Szanto A, Djordjevic ML. Metoidioplasty: surgical options and outcomes in 813 cases . Front Endocrinol . 2021;12:760284. doi:10.3389/fendo.2021.760284
Al-Tamimi M, Pigot GL, van der Sluis WB, et al. The surgical techniques and outcomes of secondary phalloplasty after metoidioplasty in transgender men: an international, multi-center case series . The Journal of Sexual Medicine . 2019;16(11):1849-1859. doi:10.1016/j.jsxm.2019.07.027
Waterschoot M, Hoebeke P, Verla W, et al. Urethral complications after metoidioplasty for genital gender affirming surgery . J Sex Med . 2021;18(7):1271–9. doi:10.1016/j.jsxm.2020.06.023
Nikolavsky D, Hughes M, Zhao LC. Urologic complications after phalloplasty or metoidioplasty . Clin Plast Surg . 2018;45(3):425–35. doi:10.1016/j.cps.2018.03.013
Nota NM, den Heijer M, Gooren LJ. Evaluation and treatment of gender-dysphoric/gender incongruent adults . In: Feingold KR, Anawalt B, Boyce A, et al., eds. Endotext . MDText.com, Inc.; 2000.
Carbonnel M, Karpel L, Cordier B, Pirtea P, Ayoubi JM. The uterus in transgender men . Fertil Steril . 2021;116(4):931–5. doi:10.1016/j.fertnstert.2021.07.005
Miller TJ, Wilson SC, Massie JP, Morrison SD, Satterwhite T. Breast augmentation in male-to-female transgender patients: Technical considerations and outcomes . JPRAS Open . 2019;21:63-74. doi:10.1016/j.jpra.2019.03.003
Claes KEY, D'Arpa S, Monstrey SJ. Chest surgery for transgender and gender nonconforming individuals . Clin Plast Surg . 2018;45(3):369–80. doi:10.1016/j.cps.2018.03.010
De Boulle K, Furuyama N, Heydenrych I, et al. Considerations for the use of minimally invasive aesthetic procedures for facial remodeling in transgender individuals . Clin Cosmet Investig Dermatol . 2021;14:513-525. doi:10.2147/CCID.S304032
Asokan A, Sudheendran MK. Gender affirming body contouring and physical transformation in transgender individuals . Indian J Plast Surg . 2022;55(2):179-187. doi:10.1055/s-0042-1749099
Sturm A, Chaiet SR. Chondrolaryngoplasty-thyroid cartilage reduction . Facial Plast Surg Clin North Am . 2019;27(2):267–72. doi:10.1016/j.fsc.2019.01.005
Chen ML, Reyblat P, Poh MM, Chi AC. Overview of surgical techniques in gender-affirming genital surgery . Transl Androl Urol . 2019;8(3):191-208. doi:10.21037/tau.2019.06.19
Wangjiraniran B, Selvaggi G, Chokrungvaranont P, Jindarak S, Khobunsongserm S, Tiewtranon P. Male-to-female vaginoplasty: Preecha's surgical technique . J Plast Surg Hand Surg . 2015;49(3):153-9. doi:10.3109/2000656X.2014.967253
Okoye E, Saikali SW. Orchiectomy . In: StatPearls [Internet] . Treasure Island (FL): StatPearls Publishing; 2022.
Salgado CJ, Yu K, Lalama MJ. Vaginal and reproductive organ preservation in trans men undergoing gender-affirming phalloplasty: technical considerations . J Surg Case Rep . 2021;2021(12):rjab553. doi:10.1093/jscr/rjab553
American Society of Plastic Surgeons. What should I expect during my recovery after facial feminization surgery?
American Society of Plastic Surgeons. What should I expect during my recovery after transmasculine bottom surgery?
de Brouwer IJ, Elaut E, Becker-Hebly I, et al. Aftercare needs following gender-affirming surgeries: findings from the ENIGI multicenter European follow-up study . The Journal of Sexual Medicine . 2021;18(11):1921-1932. doi:10.1016/j.jsxm.2021.08.005
American Society of Plastic Surgeons. What are the risks of transfeminine bottom surgery?
American Society of Plastic Surgeons. What are the risks of transmasculine top surgery?
Khusid E, Sturgis MR, Dorafshar AH, et al. Association between mental health conditions and postoperative complications after gender-affirming surgery . JAMA Surg . 2022;157(12):1159-1162. doi:10.1001/jamasurg.2022.3917
Related Articles
Do I need a referral to see a specialist? Learn more here . Explore the Department Directory Learn more about Telehealth Appointments Protect Yourself from West Nile Virus
How to schedule your APPOINTMENT at Denver Health: CURRENT PATIENTS: Login to MyChart to schedule appointments or call 303-436-4949 . NEW PATIENTS: Schedule an appointment online or call 303-436-4949 . NEED CARE? Schedule a Virtual Urgent Care appointment or click here to find an Urgent Care clinic .
MyChart Login
Login to MyChart
MyChart for Mobile
Download the MyChart mobile app for access to your healthcare information. Managing your healthcare has never been more simple. Download for iPhone and Android .
MyChart Sign Up
Learn about MyChart features , and sign up for an account .
Virtual Urgent Care Now Available for Denver Health MyChart Users
Denver Health MyChart users can now have a virtual urgent care visit with one of our expert providers. It’s easy and convenient to get the urgent care you need from the comfort of your home, using your smartphone, tablet or computer.
Click here for more details

- Departments & Services
- Conditions & Treatments
- Our Locations
- Find a Provider
- Pharmacy / Prescriptions
- Pay my bill
- Main Campus (303) 436-6000
- Appointments (303) 436-4949
- Lean Academy 855-888-5326
- Nurseline (303) 739-1211
- Pharmacy (303) 389-1390
- Telehealth (303) 436-4949
Make an Appointment
Hours of operation, gender affirming surgery (sex reassignment surgery).
Thank you for your interest in gender affirming surgery at Denver Health. There is no one-size-fits-all approach for the gender affirmation process and we are here to support you in your journey. We are proud to offer surgeries with a truly talented multi-disciplinary team of surgeons. Our services are growing as the unique needs of each individual evolve. Currently we offer the following gender affirming surgeries: MTF Top Surgery , FTM Top Surgery , Orchiectomy , FTM Hysterectomy , and Vaginoplasty surgeries.
What is Gender Affirming Surgery?
Gender affirming surgery, also known as sex reassignment surgery (SRS) or confirmation surgery, is the surgical procedure(s) by which a transgender or non-binary person’s physical appearance and functional abilities are changed to align with the gender they know themselves to be.
Complete Our Surgical Interest Form
If you are interested in a gender affirmation surgery at Denver Health, please complete one of the following forms.
Top Surgery and Hysterectomy
For vaginoplasty, breast augmentation and orchiectomy, our approach to surgical assessment.
Denver Health adheres to the guidelines for surgical assessment as described in the World Professional Association for Transgender Health Standards of Care, 8th Version . The standards were created by international agreement using the latest scientific research on transgender health so that doctors can best meet the unique health care needs of transgender and gender-nonconforming people. Most insurance companies also adhere to these guidelines.
Patients may provide referral letters from their own outside mental health providers, or the assessment process via our Behavioral Health team. Patients seeking to undergo the assessment at Denver Health should make an appointment with our Behavioral Health Team .
Read more about common frequently asked general surgery questions:
How long will my hospital stay be.
Hospital stays will vary based on specific patient response.
MTF top surgery, FTM chest surgery, FTM Hysterectomy, and orchiectomy surgery patients are usually released from the hospital the same day of surgery. Vaginoplasty patients typically spend 3 days in the hospital during recovery.
What medications will I be prescribed after surgery?
You will likely receive painkillers and antibiotics to reduce the chance of infection.
- 0 && newsLoaded" class="" data-id="{044698B9-FA04-4636-994D-47662155601F}" ref="news"> News
- 0 && blogLoaded" class="" data-id="{9AB9C6CB-06BD-4D71-867F-FAB69D88F93C}" ref="blog"> Blog Articles
- 0 && storiesLoaded" class="" data-id="{71E64EA2-1956-4F7C-A67D-579E0BB54378}" ref="stories"> Patient Stories
- May 15 Labor and Delivery Tour for Expectant Families
- May 18 Boot Camp for New Dads ®
- May 22 Labor and Delivery Tour for Expectant Families
- May 29 Labor and Delivery Tour for Expectant Families
- To save this word, you'll need to log in. Log In
gender reassignment surgery
Definition of gender reassignment surgery
Note: This term is sometimes considered to be offensive in its implication that a transgender or nonbinary person takes on a different gender through surgery, rather than using surgery to align their outward appearance with their gender identity. Gender confirmation surgery and gender-affirming surgery are the preferred terms in the medical and LGBTQ+ communities, and surgery is seen as one of many possible ways to affirm one's gender identity, rather than as an essential part of transitioning (see transition entry 2 sense 2 )
Examples of gender reassignment surgery in a Sentence
These examples are programmatically compiled from various online sources to illustrate current usage of the word 'gender reassignment surgery.' Any opinions expressed in the examples do not represent those of Merriam-Webster or its editors. Send us feedback about these examples.
Word History
1969, in the meaning defined above
Articles Related to gender reassignment surgery

Merriam-Webster's Short List of Gender...
Merriam-Webster's Short List of Gender and Identity Terms
In case you (or someone you know) has questions about what they mean
Dictionary Entries Near gender reassignment surgery
gender reassignment
gender-specific
Cite this Entry
“Gender reassignment surgery.” Merriam-Webster.com Dictionary , Merriam-Webster, https://www.merriam-webster.com/dictionary/gender%20reassignment%20surgery. Accessed 13 May. 2024.
Medical Definition
Medical definition of gender reassignment surgery.
Note: This term is sometimes considered to be offensive in its implication that a transgender or nonbinary person takes on a different gender through surgery, rather than using surgery to align their outward appearance with their gender identity. Gender confirmation surgery and gender-affirming surgery are the preferred terms in the medical and LGBTQ+ communities, and surgery is seen as one of many possible ways to affirm one's gender identity, rather than as an essential part of transitioning (see transition entry 2 ).
Subscribe to America's largest dictionary and get thousands more definitions and advanced search—ad free!

Can you solve 4 words at once?
Word of the day.
See Definitions and Examples »
Get Word of the Day daily email!
Popular in Grammar & Usage
More commonly misspelled words, your vs. you're: how to use them correctly, every letter is silent, sometimes: a-z list of examples, more commonly mispronounced words, how to use em dashes (—), en dashes (–) , and hyphens (-), popular in wordplay, the words of the week - may 10, a great big list of bread words, 10 scrabble words without any vowels, 8 uncommon words related to love, 9 superb owl words, games & quizzes.

Masks Strongly Recommended but Not Required in Maryland, Starting Immediately
Due to the downward trend in respiratory viruses in Maryland, masking is no longer required but remains strongly recommended in Johns Hopkins Medicine clinical locations in Maryland. Read more .
- Vaccines
- Masking Guidelines
- Visitor Guidelines

Vaginoplasty for Gender Affirmation
Featured Experts:

Fan Liang, M.D.

Andrew Jason Cohen, M.D.
Vaginoplasty is a surgical procedure for feminizing gender affirmation. Fan Liang, M.D. , medical director of the Johns Hopkins Center for Transgender and Gender Expansive Health , and Andrew Cohen, M.D. , director of benign urology at Johns Hopkins' Brady Urological Institute , review the options for surgery.
What is vaginoplasty?
Gender affirming surgery can be used to create a vulva and vagina. It involves removing the penis, testicles and scrotum.
During a vaginoplasty procedure, tissue in the genital area is rearranged to create a vaginal canal (or opening) and vulva (external genitalia), including the labia. A version of vaginoplasty called vulvoplasty can create a feminine-appearing outer genital area with a shallow vaginal canal.
What are the different types of vaginoplasty?
There are two main surgical approaches for this gender affirming surgery.
Vaginoplasty with Canal
This surgery is also known as full depth vaginoplasty. Vaginoplasty with canal creates not only the outer vulva but also a complete vaginal canal that makes it possible for the person to have receptive vaginal intercourse.
Vaginoplasty with canal requires dilation as part of the recovery process in order to ensure a functioning vagina suitable for penetrative sex. There are two approaches to full depth vaginoplasty.
For penile inversion vaginoplasty , surgeons create the vaginal canal using a combination of the skin surrounding the existing penis along with the scrotal skin. Depending on how much skin is available in the genital area, the surgeon may need to use a skin graft from the abdomen or thigh to construct a full vaginal canal.
Robotic-assisted peritoneal flap vaginoplasty , also called a robotic Davydov peritoneal vaginoplasty or a robotic peritoneal gender affirming vaginoplasty, is a newer approach that creates the vaginal canal with the help of a single port robotic surgical system.
The robotic system enables surgeons to reach deep into the body through a small incision by the belly button. It helps surgeons visualize the inside of the person’s pelvis more clearly and, for this procedure, creates a vaginal canal.
There are several advantages to this surgical technique. Because using the robotic system makes the surgery shorter and more precise, with a smaller incision, it can lower risk of complications. Also, the robotic vaginoplasty approach can create a full-depth vaginal canal regardless of how much preexisting (natal) tissue the person has for the surgeon to use in making the canal.
Not every surgical center has access to a single port robotic system, and getting this procedure may involve travel.
Vulvoplasty
This procedure may be called shallow depth vaginoplasty, zero depth vaginoplasty or vaginoplasty without canal. The surgeons create feminine external genitalia (vulva) with a very shallow canal. The procedure includes the creation of the labia (outer and inner lips), clitoris and vaginal opening (introitus).
The main drawback to this approach is the person cannot have receptive vaginal intercourse because no canal is created.
There are advantages, however. Because this is a much less complicated approach than vaginoplasty with canal, vulvoplasty can mean a much shorter operation, with less time in the hospital and a faster recovery. Vulvoplasty also involves less risk of complications, and does not require hair removal or postoperative dilation.
Do I need to have hair removal before vaginoplasty? When should I start?
Permanent hair removal (to remove the hair follicles to prevent regrowth) before surgery is recommended for optimal results. Patients are advised to start hair removal as soon as possible in advance of vaginoplasty, since it can take three to six months to complete the process. The hair removal process readies the tissue that will be used to create the internal vaginal canal. For people who are not able to complete the hair removal in advance, there may be residual hair in the canal after surgery.
How long is vaginoplasty surgery?
Most vaginoplasty surgeries last between four and six hours. Recovery in the hospital takes three to five days.
Illustrated Vaginoplasty Surgery
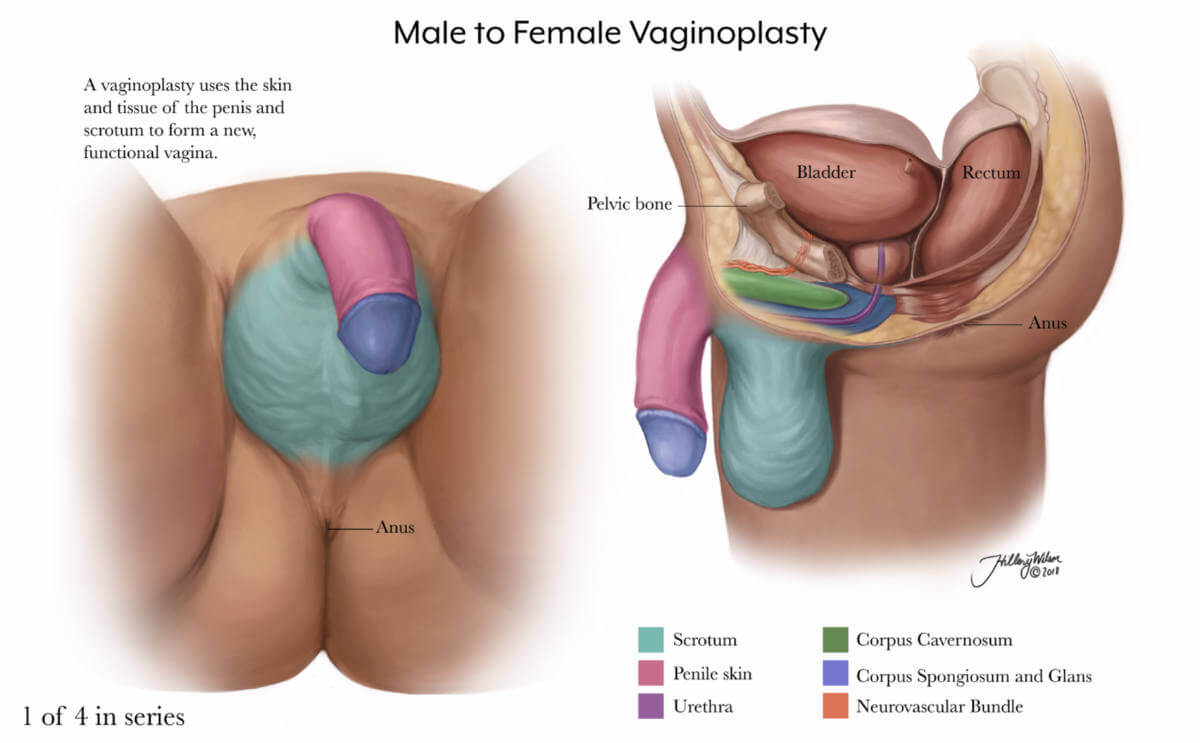
Vaginoplasty.
1 of 4 in series. Enlarged image .
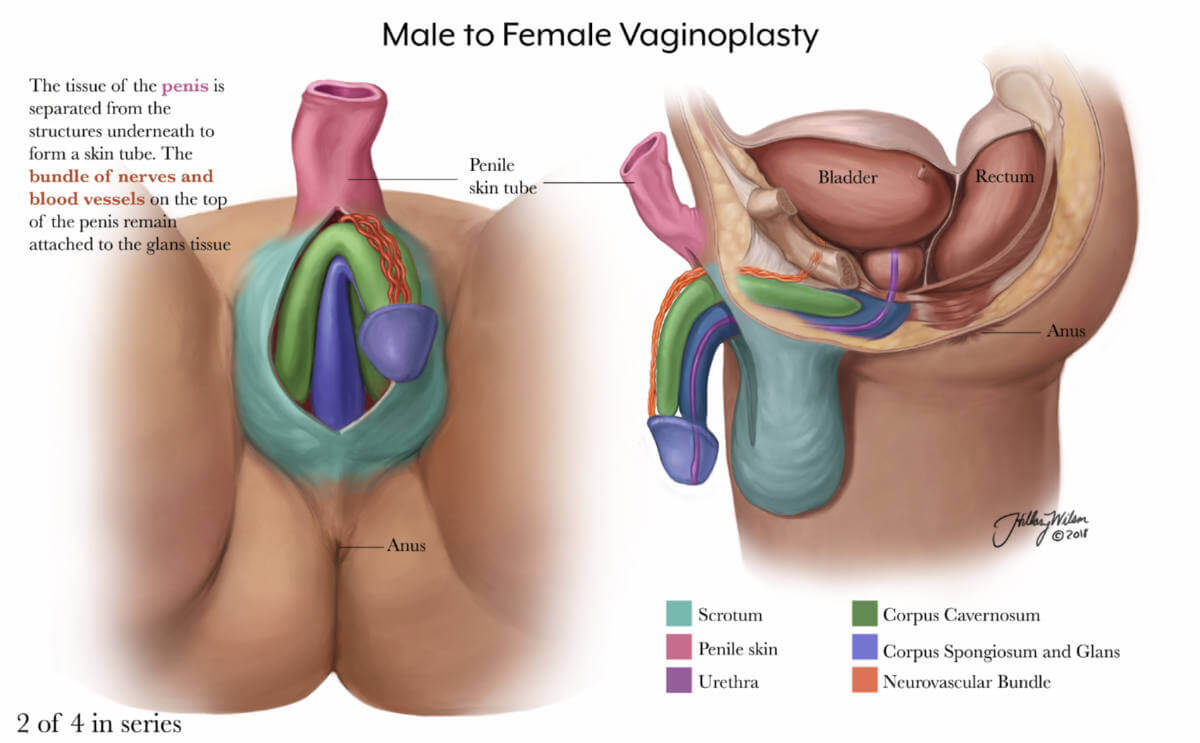
2 of 4 in series. Enlarged image .
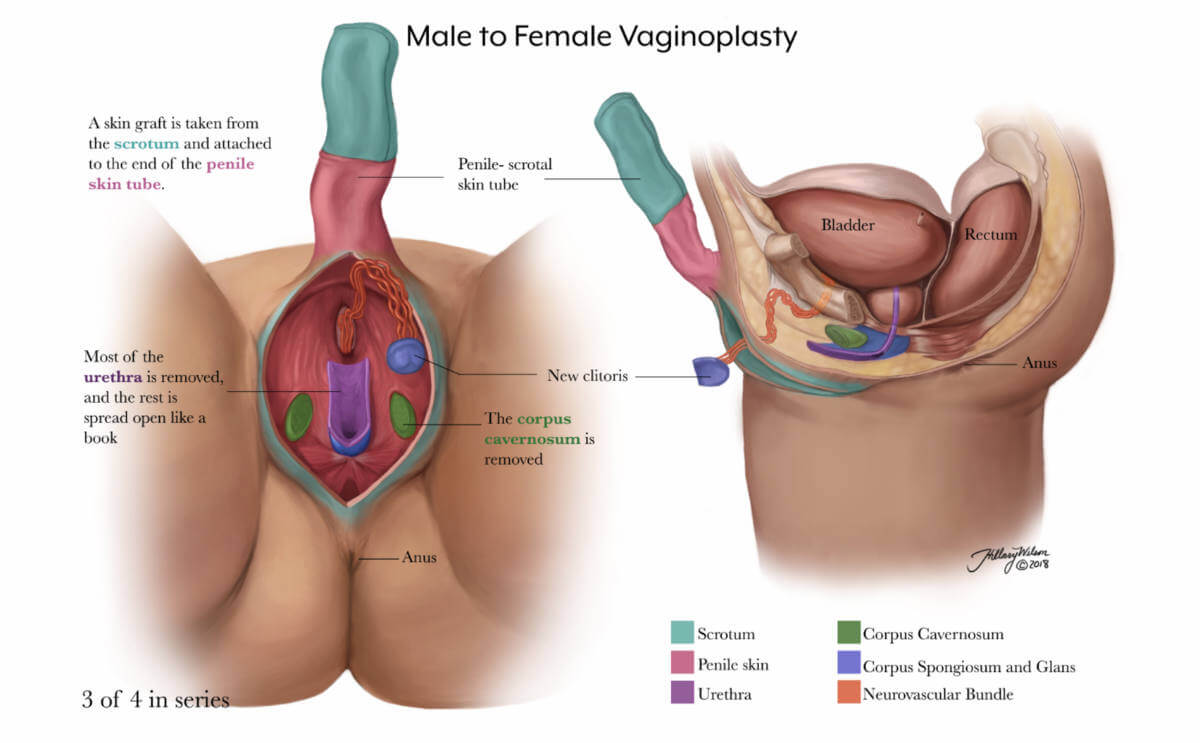
3 of 4 in series. Enlarged image .
4 of 4 in series. Enlarged image .
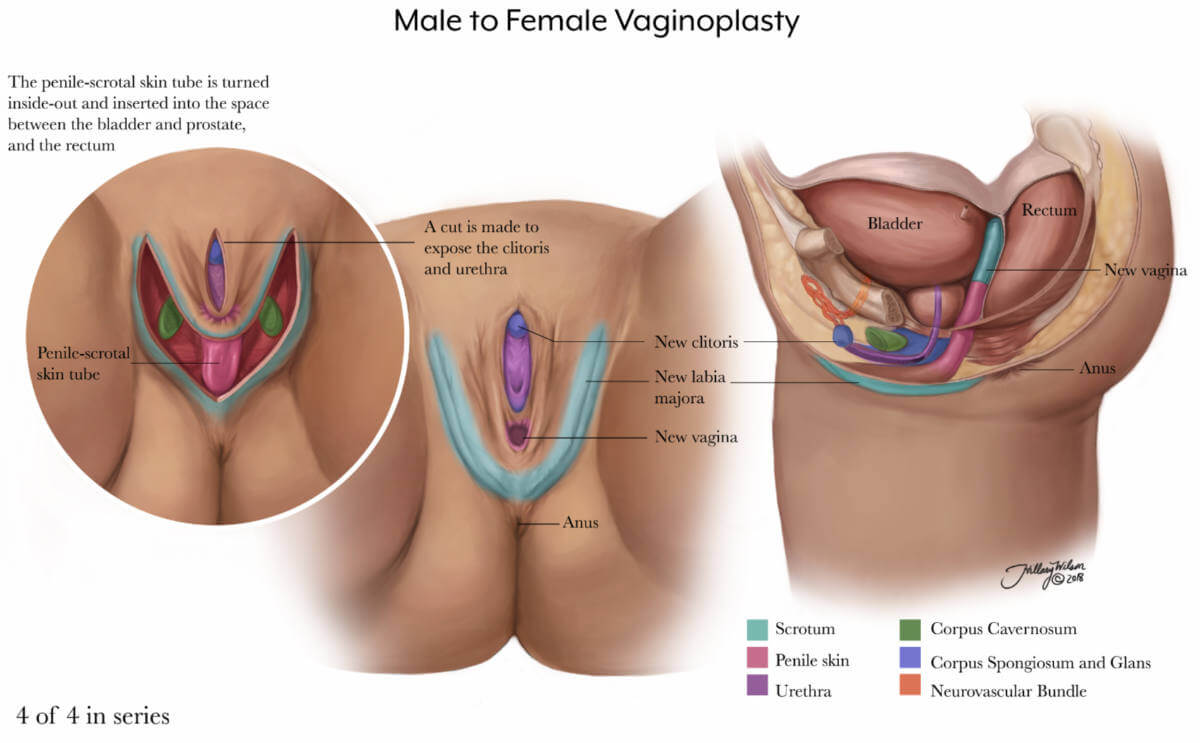
Recovery After Vaginoplasty
After surgery, you will be admitted to the hospital for one to five days. You will spend most of this time in bed recovering. Your care team will monitor your pain, and make sure you are healing appropriately and are able to go to the bathroom and walk.
On average, it can take six to eight weeks to recover from a vaginoplasty. Every person’s recovery is different, but proper home hygiene and postoperative care will give you the best chance for a faster recovery. Patients who have had vaginoplasties need to stay within a 90-minute drive of the hospital for four weeks after surgery so doctors can follow up and address any issues.
Consistent daily dilation for the first three months is essential for best outcome. Before you go home, you will be taught how to dilate if you have a vaginoplasty with canal. You will be given dilators before discharge to use at home.
What is dilation after vaginoplasty?
Part of the healing process after vaginoplasty involves dilation — inserting a medical grade dilator into the vagina to keep your vaginal canal open as it heals. The hospital may provide you with a set of different sized dilators to use.
A doctor or therapist from your care team will show you how to dilate. This can be difficult at first, but professionals will work with you and your comfort level to help you get accustomed to this aspect of your healing process. You will begin dilating with the smallest dilator in the dilator pack. You continue to use this dilator until cleared to advance to the next size by your care team.
During the first few weeks after surgery, you must dilate three times a day for at least 20 minutes. It is very important that you continue dilating, especially during your immediate postoperative period, to prevent losing vaginal depth and width. Patients continue to use a dilator for as long as the care team recommends. Some patients may need to dilate their whole lives.
Is dilation after vaginoplasty painful?
Dilation should not be a painful process. At first, you may feel discomfort as you learn the easiest angles and techniques for your body. If you feel severe pain at any time during dilation, it is important to stop, adjust the dilator, and reposition your body so you are more comfortable. It is also important to use lubricant when you dilate. A pelvic floor therapist can work with you to help you get used to this aspect of recovery.
Will I have a catheter?
Yes. While you are in the hospital, you will have a Foley catheter in the urethra that will be taken out before you go home.
Will I have surgical drains?
Yes, your surgeon will place a drain while you are in the operating room, which will be removed before you leave.
Can I shower after vaginoplasty surgery?
Yes. It is very important to clean the area to prevent infections. You can gently wash the area with soap and water. Never scrub or allow water to be sprayed directly at the surgical site.
Is going to the bathroom different?
It is important to remember for the rest of your life that when wiping with toilet paper or washing the genital area, always wipe front to back. This helps keep your vagina clean and prevents infection from the anal region.
You may notice some spraying when you urinate. This is common, and can be addressed with physical therapy to help strengthen the pelvic floor. A physical therapist can help you with exercises, which may help improve urination over time.
Is the vagina created by vaginoplasty sexually functional?
Yes. After vaginoplasty that includes creation of a vaginal canal, a person can have receptive, penetrative sex.
You must avoid any form of sexual activity for 12 weeks after surgery to allow your body to recover and avoid complications. After 12 weeks, the vagina is healed enough for receptive intercourse.
What will my vagina look like?
Vulvas and vaginas are as unique as a fingerprint, and there are many anatomic variations from person to person. Surgical results vary, also. You can expect that the surgery will recreate the labia minora and majora, a clitoral hood and the clitoris will be under the hood. Make sure you discuss your concerns with your surgeon, who can help you understand what to expect from your individual surgical results.

What is the average depth of a vagina after vaginoplasty?
The depth of a fully constructed vaginal canal depends on patient preferences and anatomy. On average, the constructed vaginal canal is between 5 and 7 inches deep. Vaginal depth may depend on the amount of skin available in the genital area before your vaginoplasty. This varies among individuals, and some patients may need skin grafts.
Newer robotic techniques may be able to increase the vaginal depth for those people with less existing tissue for the surgeon to work with.
Will I need any additional surgery after vaginoplasty?
You may need additional surgical procedures to revise the appearance of the new vagina and vulva. Later revisions can improve aesthetic appearance, but these are not typically covered by insurance.
Vaginoplasty Complications
Vaginoplasty is safe, overall, and newer techniques are reducing the risks of problems even further. But sometimes, patients experience complications related to the procedure. These can include:
- Slow wound healing
- Narrowing of the vaginal canal (regular dilating as prescribed can lower this risk)
Some rare complications may require further surgery to repair:
- A fistula (an abnormal connection between the new vagina and the rectum or bladder)
- Injury to the urethra, which may require surgery or a suprapubic catheter
- Rectal injury (very rare) may require a low-fiber diet, a colostomy or additional surgery.
Be sure to discuss your concerns with your surgeon, who will work with you for optimal results.
Find a Doctor
Specializing In:
- Gender Affirmation Surgery
- Transgender Health
At Another Johns Hopkins Member Hospital:
- Howard County Medical Center
- Sibley Memorial Hospital
- Suburban Hospital
Find a Treatment Center
- Center for Transgender and Gender Expansive Health
- Plastic and Reconstructive Surgery
Find Additional Treatment Centers at:

Request an Appointment

Phalloplasty for Gender Affirmation

Top Surgery

Facial Feminization Surgery (FFS)
Related Topics
Thank you for visiting nature.com. You are using a browser version with limited support for CSS. To obtain the best experience, we recommend you use a more up to date browser (or turn off compatibility mode in Internet Explorer). In the meantime, to ensure continued support, we are displaying the site without styles and JavaScript.
- View all journals
- Explore content
- About the journal
- Publish with us
- Sign up for alerts
- Review Article
- Published: 12 April 2011
Gender reassignment surgery: an overview
- Gennaro Selvaggi 1 &
- James Bellringer 1
Nature Reviews Urology volume 8 , pages 274–282 ( 2011 ) Cite this article
3962 Accesses
152 Citations
43 Altmetric
Metrics details
- Pathogenesis
- Reconstruction
- Urogenital diseases
This article has been updated
Gender reassignment (which includes psychotherapy, hormonal therapy and surgery) has been demonstrated as the most effective treatment for patients affected by gender dysphoria (or gender identity disorder), in which patients do not recognize their gender (sexual identity) as matching their genetic and sexual characteristics. Gender reassignment surgery is a series of complex surgical procedures (genital and nongenital) performed for the treatment of gender dysphoria. Genital procedures performed for gender dysphoria, such as vaginoplasty, clitorolabioplasty, penectomy and orchidectomy in male-to-female transsexuals, and penile and scrotal reconstruction in female-to-male transsexuals, are the core procedures in gender reassignment surgery. Nongenital procedures, such as breast enlargement, mastectomy, facial feminization surgery, voice surgery, and other masculinization and feminization procedures complete the surgical treatment available. The World Professional Association for Transgender Health currently publishes and reviews guidelines and standards of care for patients affected by gender dysphoria, such as eligibility criteria for surgery. This article presents an overview of the genital and nongenital procedures available for both male-to-female and female-to-male gender reassignment.
The management of gender dysphoria consists of a combination of psychotherapy, hormonal therapy, and surgery
Psychiatric evaluation is essential before gender reassignment surgical procedures are undertaken
Gender reassignment surgery refers to the whole genital, facial and body procedures required to create a feminine or a masculine appearance
Sex reassignment surgery refers to genital procedures, namely vaginoplasty, clitoroplasty, labioplasty, and penile–scrotal reconstruction
In male-to-female gender dysphoria, skin tubes formed from penile or scrotal skin are the standard technique for vaginal construction
In female-to-male gender dysphoria, no technique is recognized as the standard for penile reconstruction; different techniques fulfill patients' requests at different levels, with a variable number of surgical technique-related drawbacks
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
195,33 € per year
only 16,28 € per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
Male delayed orgasm and anorgasmia: a practical guide for sexual medicine providers

Polycystic ovary syndrome
Biological sex classification with structural MRI data shows increased misclassification in transgender women
Change history, 26 april 2011.
In the version of this article initially published online, the statement regarding the frequency of male-to-female transsexuals was incorrect. The error has been corrected for the print, HTML and PDF versions of the article.
Meyer, W. 3rd. et al . The Harry Benjamin International Gender Dysphoria Association's standards of care for gender identity disorders, sixth version. World Professional Association for Transgender Health [online] , (2001).
Google Scholar
Bakker, A., Van Kesteren, P., Gooren, L. & Bezemer, P. The prevalence of transsexualism in The Netherlands. Acta Psychiatr. Scand. 87 , 237–238 (1993).
Article CAS Google Scholar
Selvaggi, G. et al . Gender identity disorder: general overview and surgical treatment for vaginoplasty in male-to-female transsexuals. Plast. Reconstr. Surg. 116 , 135e–145e (2005).
Article Google Scholar
Benjamin, H. (ed.) The Transsexual Phenomenon (Julian Press Inc., New York, 1966).
World Professional Association for Transgender Health [online] , (2010).
Zhou, J. N., Hofman, M. A., Gooren, L. J. & Swaab, D. F. A sex difference in the human brain and its relation to transsexuality. Nature 378 , 68–70 (1995).
Kruijver, F. P. et al . Male-to-female transsexuals have female neuron numbers in a limbic nucleus. J. Clin. Endocrinol. Metab. 85 , 2034–2041 (2000).
Swaab, D. F., Chun, W. C., Kruijver, F. P., Hofman, M. A. & Ishuina, T. A. Sexual differentiation of the human hypothalamus. Adv. Exp. Med. Biol. 511 , 75–105 (2002).
Garcia-Falgueras, A. & Swaab, D. F. A sex difference in the hypothalamic uncinate nucleus: relationship to gender identity. Brain 131 , 3115–3117 (2008).
Cohen-Kettenis, P. & Kuiper, B. Transseksualiteit en psychotherapie [Dutch]. Tijdschr. Psychoth. 3 , 153–166 (1984).
Kuiper, B. & Cohen-Kettenis, P. Sex reassignment surgery: a study of 141 Dutch transsexuals. Arch. Sex. Behav. 17 , 439–457 (1988).
Kanhai, R. C., Hage, J. J., Karim, R. B. & Mulder, J. W. Exceptional presenting conditions and outcome of augmentation mammoplasty in male-to female transsexuals. Ann. Plast. Surg. 43 , 476–483 (1999).
Kanagalingm, J. et al . Cricothyroid approximation and subluxation in 21 male-to-female transsexuals. Laryngoscope 115 , 611–618 (2005).
Bouman, M. Laparoscopic assisted colovaginoplasty. Presented at the 2009 biennial World Professional Association for Transgender Health meeting, Oslo.
Rubin, S. O. Sex-reassignment surgery male-to-female. Review, own results and report of a new technique using the glans penis as a pseudoclitoris. Scand. J. Urol. Nephrol. Suppl. 154 , 1–28 (1993).
CAS PubMed Google Scholar
Fang, R. H., Chen, C. F. & Ma, S. A new method for clitoroplasty in male-to-female sex reassignment surgery. Plast. Reconstr. Surg. 89 , 679–682 (1992).
Selvaggi, G. et al . Genital sensitivity in sex reassignment surgery. Ann. Plast. Surg. 58 , 427–433 (2007).
Watanayusakul, S. SRS procedures. The Suporn Clinic [online] , (2010).
Melzer, T. Managing complications of male to female surgery. Presented at the 2007 World Professional Association for Transgender Health biennial meeting, Chicago.
Gilleard, O., Qureshi, M., Thomas, P. & Bellringer, J. Urethral bleeding following male to female gender reassignmetn surgery. Presented at the 2009 World Professional Association for Transgender Health biennial meeting, Oslo.
Beckley, I., Thomas, P. & Bellringer, J. Aetiology and management of recto-vaginal fistulas following male to female gender reassignment. Presented at 2008 EAU section of genitourinary surgeons and the EAU section of andrological urology meeting, Madrid.
Monstrey, S. et al . Chest wall contouring surgery in female-to-male (FTM) transsexuals: a new algorithm. Plast. Reconstr. Surg. 121 , 849–859 (2008).
Mueller, A. & Gooren, L. Hormone-related tumors in transsexuals receiving treatment with cross-sex hormones. Eur. J. Endocrinol. 159 , 197–202 (2008).
Selvaggi, G., Elander, A. & Branemark, R. Penile epithesis: preliminary study. Plast. Reconstr. Surg. 126 , 265e–266e (2010).
Selvaggi, G. & Elander, A. Penile reconstruction/formation. Curr. Opin. Urol. 18 , 589–597 (2008).
Gilbert, D. A., Jordan, G. H., Devine, C. J. Jr & Winslow, B. H. Microsurgical forearm “cricket bat-transformer” phalloplasty. Plast. Reconstr. Surg. 90 , 711–716 (1992).
Bettocchi, C., Ralph, D. J. & Pryor, J. P. Pedicled pubic phalloplasty in females with gender dysphoria. BJU Int. 95 , 120–124 (2005).
Monstrey, S. et al . Penile reconstruction: is the radial forearm flap really the standard technique? Plast. Reconstr. Surg. 124 , 510–518 (2009).
Selvaggi, G. et al . Donor-site morbidity of the radial forearm free flap after 125 phalloplasties in gender identity disorder. Plast. Reconstr. Surg. 118 , 1171–1177 (2006).
Hoebeke, P. et al . Impact of sex reassignment surgery on lower urinary tract function. Eur. Urol. 47 , 398–402 (2005).
Agrawal, V. & Ralph, D. An audit of implanted penile prosteses in the UK. BJU Int. 98 , 393–395 (2006).
Hoebeke, P. B. et al . Erectile implants in female-to-male transsexuals: our experience in 129 patients. Eur. Urol. 57 , 334–340 (2010).
Vesely, J. et al . New technique of total phalloplasty with reinnervated latissimus dorsi myocutaneous free flap in female-to-male transsexuals. Ann. Plast. Surg. 58 , 544–550 (2007).
Selvaggi, G. et al . Scrotal reconstruction in female-to-male transsexuals: a novel scrotoplasty. Plast. Reconstr. Surg. 123 , 1710–1718 (2009).
Download references
Author information
Authors and affiliations.
Gender Surgery Unit, Charing Cross Hospital, Imperial College NHS Trust, 179–183 Fulham Palace Road, London, W6 8QZ, UK
Gennaro Selvaggi & James Bellringer
You can also search for this author in PubMed Google Scholar
Contributions
G. Selvaggi and J. Bellringer contributed equally to the research, discussions, writing, reviewing, and editing of this article.
Corresponding author
Correspondence to James Bellringer .
Ethics declarations
Competing interests.
The authors declare no competing financial interests.
Rights and permissions
Reprints and permissions
About this article
Cite this article.
Selvaggi, G., Bellringer, J. Gender reassignment surgery: an overview. Nat Rev Urol 8 , 274–282 (2011). https://doi.org/10.1038/nrurol.2011.46
Download citation
Published : 12 April 2011
Issue Date : May 2011
DOI : https://doi.org/10.1038/nrurol.2011.46
Share this article
Anyone you share the following link with will be able to read this content:
Sorry, a shareable link is not currently available for this article.
Provided by the Springer Nature SharedIt content-sharing initiative
This article is cited by
A bibliometric and visualisation analysis on the research of female genital plastic surgery based on the web of science core collection database.
- Xianling Zhang
Aesthetic Plastic Surgery (2024)
Chest Feminization in Transwomen with Subfascial Breast Augmentation—Our Technique and Results
- James Roy Kanjoor
- Temoor Mohammad Khan
Aesthetic Plastic Surgery (2023)
Vaginoplasty in Male to Female transgenders: single center experience and a narrative review
- Luca Ongaro
- Giulio Garaffa
- Giovanni Liguori
International Journal of Impotence Research (2021)
Urethral complications after gender reassignment surgery: a systematic review
- L. R. Doumanian
Overview on metoidioplasty: variants of the technique
- Marta Bizic
- Borko Stojanovic
- Miroslav Djordjevic
Quick links
- Explore articles by subject
- Guide to authors
- Editorial policies
Sign up for the Nature Briefing newsletter — what matters in science, free to your inbox daily.
Appointments at Mayo Clinic
- Dilation after gender-affirming surgery
This material is for your education and information only. This content does not replace medical advice, diagnosis and treatment. If you have questions about a medical condition, always talk with your health care provider.
Narrator: Vaginal dilation is important to your recovery and ongoing care. You have to dilate to maintain the size and shape of your vaginal canal and to keep it open.
Jessi: I think for many trans women, including myself, but especially myself, I looked forward to one day having surgery for a long time. So that meant looking up on the internet what the routines would be, what the surgery entailed. So I knew going into it that dilation was going to be a very big part of my routine post-op, but just going forward, permanently.
Narrator: Vaginal dilation is part of your self-care. You will need to do vaginal dilation for the rest of your life.
Alissa (nurse): If you do not do dilation, your vagina may shrink or close. If that happens, these changes might not be able to be reversed.
Narrator: For the first year after surgery, you will dilate many times a day. After the first year, you may only need to dilate once a week. Most people dilate for the rest of their life.
Jessi: The dilation became easier mostly because I healed the scars, the stitches held up a little bit better, and I knew how to do it better. Each transgender woman's vagina is going to be a little bit different based on anatomy, and I grew to learn mine. I understand, you know, what position I needed to put the dilator in, how much force I needed to use, and once I learned how far I needed to put it in and I didn't force it and I didn't worry so much on oh, did I put it in too far, am I not putting it in far enough, and I have all these worries and then I stress out and then my body tenses up. Once I stopped having those thoughts, I relaxed more and it was a lot easier.
Narrator: You will have dilators of different sizes. Your health care provider will determine which sizes are best for you. Dilation will most likely be painful at first. It's important to dilate even if you have pain.
Alissa (nurse): Learning how to relax the muscles and breathe as you dilate will help. If you wish, you can take the pain medication recommended by your health care team before you dilate.
Narrator: Dilation requires time and privacy. Plan ahead so you have a private area at home or at work. Be sure to have your dilators, a mirror, water-based lubricant and towels available. Wash your hands and the dilators with warm soapy water, rinse well and dry on a clean towel. Use a water-based lubricant to moisten the rounded end of the dilators. Water-based lubricants are available over-the-counter. Do not use oil-based lubricants, such as petroleum jelly or baby oil. These can irritate the vagina. Find a comfortable position in bed or elsewhere. Use pillows to support your back and thighs as you lean back to a 45-degree angle. Start your dilation session with the smallest dilator. Hold a mirror in one hand. Use the other hand to find the opening of your vagina. Separate the skin. Relax through your hips, abdomen and pelvic floor. Take slow, deep breaths. Position the rounded end of the dilator with the lubricant at the opening to your vaginal canal. The rounded end should point toward your back. Insert the dilator. Go slowly and gently. Think of its path as a gentle curving swoop. The dilator doesn't go straight in. It follows the natural curve of the vaginal canal. Keep gentle down and inward pressure on the dilator as you insert it. Stop when the dilator's rounded end reaches the end of your vaginal canal. The dilators have dots or markers that measure depth. Hold the dilator in place in your vaginal canal. Use gentle but constant inward pressure for the correct amount of time at the right depth for you. If you're feeling pain, breathe and relax the muscles. When time is up, slowly remove the dilator, then repeat with the other dilators you need to use. Wash the dilators and your hands. If you have increased discharge following dilation, you may want to wear a pad to protect your clothing.
Jessi: I mean, it's such a strange, unfamiliar feeling to dilate and to have a dilator, you know to insert a dilator into your own vagina. Because it's not a pleasurable experience, and it's quite painful at first when you start to dilate. It feels much like a foreign body entering and it doesn't feel familiar and your body kind of wants to get it out of there. It's really tough at the beginning, but if you can get through the first month, couple months, it's going to be a lot easier and it's not going to be so much of an emotional and uncomfortable experience.
Narrator: You need to stay on schedule even when traveling. Bring your dilators with you. If your schedule at work creates challenges, ask your health care team if some of your dilation sessions can be done overnight.
Alissa (nurse): You can't skip days now and do more dilation later. You must do dilation on schedule to keep vaginal depth and width. It is important to dilate even if you have pain. Dilation should cause less pain over time.
Jessi: I hear that from a lot of other women that it's an overwhelming experience. There's lots of emotions that are coming through all at once. But at the end of the day for me, it was a very happy experience. I was glad to have the opportunity because that meant that while I have a vagina now, at the end of the day I had a vagina. Yes, it hurts, and it's not pleasant to dilate, but I have the vagina and it's worth it. It's a long process and it's not going to be easy. But you can do it.
Narrator: If you feel dilation may not be working or you have any questions about dilation, please talk with a member of your health care team.
Mayo Clinic does not endorse companies or products. Advertising revenue supports our not-for-profit mission.
- Opportunities
Mayo Clinic Press
Check out these best-sellers and special offers on books and newsletters from Mayo Clinic Press .
- Mayo Clinic on Incontinence - Mayo Clinic Press Mayo Clinic on Incontinence
- The Essential Diabetes Book - Mayo Clinic Press The Essential Diabetes Book
- Mayo Clinic on Hearing and Balance - Mayo Clinic Press Mayo Clinic on Hearing and Balance
- FREE Mayo Clinic Diet Assessment - Mayo Clinic Press FREE Mayo Clinic Diet Assessment
- Mayo Clinic Health Letter - FREE book - Mayo Clinic Press Mayo Clinic Health Letter - FREE book
Your gift holds great power – donate today!
Make your tax-deductible gift and be a part of the cutting-edge research and care that's changing medicine.
Medindia » Articles » Procedure » FAQs on Gender-Reassignment Surgery: Everything You Need to Know
Gender-Reassignment Surgery: Everything You Need to Know
- Indications
- Non-Surgical Procedures
- Surgical Procedures
- Risks in Non-Surgical and Surgical Procedures
- Whom to consult?
- Pre-Op Considerations
- Post-Op Considerations
- Impact on Mental Health
- Cost of the Surgery
FAQs on Gender-Reassignment Surgery: Everything You Need to Know
Html.Raw(Model.contents.ToString())
Please use one of the following formats to cite this article in your essay, paper or report:
Dr. Preethi Balasubramanian. (2024, May 08). Gender-Reassignment Surgery: Everything You Need to Know . Medindia. Retrieved on May 13, 2024 from https://www.medindia.net/health/procedure/gender-reassignment-surgery-everything-you-need-to-know-faqs.htm.
Dr. Preethi Balasubramanian. "Gender-Reassignment Surgery: Everything You Need to Know". Medindia . May 13, 2024. <https://www.medindia.net/health/procedure/gender-reassignment-surgery-everything-you-need-to-know-faqs.htm>.
Dr. Preethi Balasubramanian. "Gender-Reassignment Surgery: Everything You Need to Know". Medindia. https://www.medindia.net/health/procedure/gender-reassignment-surgery-everything-you-need-to-know-faqs.htm. (accessed May 13, 2024).
Dr. Preethi Balasubramanian. 2024. Gender-Reassignment Surgery: Everything You Need to Know . Medindia, viewed May 13, 2024, https://www.medindia.net/health/procedure/gender-reassignment-surgery-everything-you-need-to-know-faqs.htm.

ASK A DOCTOR ONLINE

What's New on Medindia

Follow @MedIndia
Gender-Reassignment Surgery: Everything You Need to Know - Related News
- Addressing Mental Health Needs in the Transgender Community
- A Global Comparison: Best Countries for Gender Reassignment Surgery
- Transgender Healthcare Disparities Highlighted
- Why is Thyroid Cancer More Common Among Transgender Female Veterans?
- Is Gender Reassignment Surgery Against Nature?
- Consult Online Doctor
- Take Telemedicine course
- Health Centers
- Health Tools
- Health info by Speciality
- Know Your Body
- Health and Wellness
- Web Stories
- Health Tips
- Nutrition Facts
- Lifestyle & Wellness
- Beauty Tips
- Diet & Nutrition
- Home Remedies
- Obesity & Weight Loss
- Complementary Medicine
- Special Reports
- Press Releases
- Health Guide
- Health articles
- Health Quiz
- Health Facts
- Travel Health
- Medicine and Movies
- Symptom Articles
- Diabetes Tools
- Pediatric Calculators
- Men's Health
- Women's Health
- Height Weight Tools
- Cardiac Tools
- Pharma Tools
- Wellness Interactive Tools
- Drug Information
- Drugs by Condition
- Drug Price List - Brand Names
- Drug Interaction with Food
- Drug Price List - Generic Names
- Drugs - Side Effects
- Drug Videos
- Drug Database
- Doctor Directory
- Diagnostic Lab Directory
- Hospital Directory
- Pharmacy or Chemist
- Medical Equipment Suppliers
- Pharma Directory
- Emergency Services
- PG Education
- Family Medicine
- Other Resources
- Medical Aphorism
- Health Acts in India
- Health Quotations
- Medical Conference
- Amazing Body Facts
- Health poll

- Editorial Team
- Exclusive Interviews
- In the News
- Partners & Affiliates
- Advertise With Us
- हिन्दी
- français
- Español
- 中文
- Cambridge Dictionary +Plus
Meaning of reassignment in English
Your browser doesn't support HTML5 audio
- accommodate
- accommodate someone with something
- administration
- arm someone with something
- hand something down
- hand something in
- hand something out
- hand something over
reassignment | Business English
Examples of reassignment, translations of reassignment.
Get a quick, free translation!

Word of the Day
call centre
a large office in which a company's employees provide information to its customers, or sell or advertise its goods or services, by phone

Varied and diverse (Talking about differences, Part 1)

Learn more with +Plus
- Recent and Recommended {{#preferredDictionaries}} {{name}} {{/preferredDictionaries}}
- Definitions Clear explanations of natural written and spoken English English Learner’s Dictionary Essential British English Essential American English
- Grammar and thesaurus Usage explanations of natural written and spoken English Grammar Thesaurus
- Pronunciation British and American pronunciations with audio English Pronunciation
- English–Chinese (Simplified) Chinese (Simplified)–English
- English–Chinese (Traditional) Chinese (Traditional)–English
- English–Dutch Dutch–English
- English–French French–English
- English–German German–English
- English–Indonesian Indonesian–English
- English–Italian Italian–English
- English–Japanese Japanese–English
- English–Norwegian Norwegian–English
- English–Polish Polish–English
- English–Portuguese Portuguese–English
- English–Spanish Spanish–English
- English–Swedish Swedish–English
- Dictionary +Plus Word Lists
- English Noun
- Business Noun
- Translations
- All translations
To add reassignment to a word list please sign up or log in.
Add reassignment to one of your lists below, or create a new one.
{{message}}
Something went wrong.
There was a problem sending your report.
- Type 2 Diabetes
- Heart Disease
- Digestive Health
- Multiple Sclerosis
- Diet & Nutrition
- Supplements
- Health Insurance
- Public Health
- Patient Rights
- Caregivers & Loved Ones
- End of Life Concerns
- Health News
- Thyroid Test Analyzer
- Doctor Discussion Guides
- Hemoglobin A1c Test Analyzer
- Lipid Test Analyzer
- Complete Blood Count (CBC) Analyzer
- What to Buy
- Editorial Process
- Meet Our Medical Expert Board
- What to Eat After
- Foods to Eat and Avoid
Colectomy (Colon Resection Surgery): What You Need to Know
- Is It Major Surgery?
- Reasons for It
- Preparation
- Day of Surgery
- When to Call a Provider
- Next in Colectomy Surgery Guide What Is a Partial or Total Colectomy?
A colectomy is a type of surgery that removes part or all of the colon. The colon is part of the large intestine that connects the small intestine to the rectum. The colon is removed either in whole or in part to treat or prevent a disease or condition.
Some of the more common reasons for a colectomy are inflammatory bowel disease (IBD) , colon cancer, or diverticular disease .
This article will discuss the types of colectomy, reasons for this surgery, what to expect, recovery, and outlook.
HRAUN / Getty Images
Is Colectomy a Major Surgery?
A colectomy is a major surgery requiring general anesthesia and a hospital stay of a few days to over a week before going home to continue your recovery.
Many variables affect how a colectomy is performed and how much recovery time is needed. However, in general, this surgery will require several weeks of healing before you can return to regular activities.
If a colectomy is done laparascopically, using specialized surgical tools that are passed through small incisions, the recovery time may be shorter than if the surgery is performed using a large incision.
Types of Colectomy
A colectomy is not one type of surgery; it includes several different types. In some cases, the surgeons may not know exactly what needs to be done until they get inside the abdomen.
If a colectomy is recommended, you should ask questions about the surgery to find out what is expected with each type of colectomy that may be needed.
Partial Colectomy
In a partial colectomy, a section of the colon to include any part is removed. After the part of the colon that is injured or diseased is removed, the two healthy ends are reattached. This type of surgery may be used to treat Crohn's disease (a form of IBD, which also includes ulcerative colitis ), colon cancer , or diverticular disease.
Hemicolectomy
A hemicolectomy is when the colon's left or right side is removed. A left hemicolectomy removes the descending colon (located on the left side of the abdomen). When the ascending colon , which runs along the right side of the abdomen, is removed, it is known as a right hemicolectomy.
This type of colectomy might be done most commonly for colon cancer. However, it could also be used to treat:
- IBD (Crohn's disease or ulcerative colitis )
- Bowel blockage
- Diverticular disease
- Trauma to the colon
- Ischemic colitis
Total Colectomy
In a total colectomy, the entire colon is removed. However, either part or all of the rectum is left intact. The outcome of this surgery could take one of a few forms.
An ileostomy may be performed, in which the end of the small intestine is brought through the abdominal wall to make a stoma (a surgical hole made in the body). The stoma is where stool exits the body. An appliance is worn over it and emptied as needed.
In other cases, the healthy end of the small intestine might be connected to the rectum, and stool leaves the body through the anus. A total colectomy might be used for:
- Severe constipation
- Colon cancer
Proctocolectomy
In this form of surgery, the rectum is removed along with the colon. With this surgery, a permanent ileostomy will also need to be placed.
This surgery may be used to treat:
- Colon and rectal cancer
- Congenital (present at birth) problems affecting the rectum or anus
Reasons for Colectomy Surgery
A colectomy may be used to treat several diseases or conditions affecting the colon and/or rectum.
One common reason for a colectomy is to treat IBD. In Crohn's disease, part or all of the colon may be removed. If all of the colon is removed, an ileostomy will be placed.
In ulcerative colitis, a total colectomy is always used. Either an ileostomy is placed, or additional surgeries will create a rectum from the last section of the small intestine.
Diverticular disease is another reason for colectomy surgery. Inflamed diverticula (outpouchings of the colon) cause diverticulitis . In most cases, it can be treated without surgery. When surgery is used, the affected section of the colon is removed.
Ischemic colitis is a condition in which blood flow to the colon is cut off or restricted for some reason. It is usually treated medically in the hospital.
However, there are cases of ischemic colitis in which parts of the colon's tissues have begun to die. In that instance, those sections of the colon would be removed with a partial or a hemicolectomy. If there are complications, a total colectomy with an ileostomy might be necessary.
Colon cancer is another reason that a colectomy may be needed. In most cases, only the section of the colon that is affected by colon cancer is removed.
A total colectomy and an ileostomy are rarely used, such as in the case of colon cancer in a person with familial adenomatous polyposis, a hereditary condition that causes hundreds of polyps (growths in the colon lining) that begin as benign but become cancerous.
Preparing for Colectomy Surgery: What Happens Before?
Several things must be done before colectomy surgery. The surgical team will give instructions on what tests and preparations are needed before the procedure. You should ask as many questions as needed to be sure you understand what will happen before, during, and after the surgery.
Blood tests may be done prior to a colectomy to understand a person's readiness for surgery and to look for any other issues that may be present or could lead to complications. Lung X-rays and other tests may also be done to ensure there are no problems with breathing.
Medications
Some medications may need to be stopped in the days before surgery. This includes any drugs that could increase the risk of bleeding or infection after surgery.
Plan Your Hospital Stay
After colectomy surgery, you may be in the hospital for several days. You will need to plan to be away from home and bring comfort items such as mobile devices, toiletries, and slippers to the hospital.
Preoperative Counseling
The surgical team will be available to answer questions about the surgery. If there will be an ileostomy placed, you will meet with an enterostomal therapy (ET) nurse .
An ET nurse will explain what to expect in the first days and weeks with a new stoma, including how ostomy pouches work. They will also help determine the best location for the stoma based on your lifestyle and the type of clothing you like to wear.
Before colectomy surgery, you must drink a special solution or take a series of tablets that help clear all the stool from the colon and rectum. There are several types of preparations , and surgeons will choose the ones they prefer.
Preparation may take place in the day or two before surgery. Usually, nothing to eat or drink is allowed on the morning of surgery or a few hours before the surgery.
What Happens on the Day of Your Colectomy?
On the day of the colectomy, you will go to the hospital at the time requested by the surgical team. It's important to bring a photo ID and your insurance information. The hospital staff will provide several forms for you to review and sign.
You will change into a surgical gown and be prepped for surgery. An intravenous (IV) line will be placed for the administration of fluids as well as medications. Some medications may be given before going into the operating room. Your temperature, blood pressure, and heart rate will all be taken.
Once in the operating room, you will receive general anesthesia to ensure you are not awake during the surgery. The surgical team will then prepare the patient for surgery and monitor breathing, blood pressure, and heart rate throughout the surgery.
What Happens During a Colectomy Procedure?
You will be under general anesthesia for a colectomy and will be asleep the entire time. The surgery may be done laparoscopically or with an open incision. The surgery will take several hours, potentially four or more. Recovery in the hospital will take place over several days.
Laparoscopic Surgery
When possible, laparoscopic surgery (considered minimally invasive surgery) will be used. Several small incisions are made in the abdomen. Specialized tools are passed through those incisions to complete the procedure.
The surgeon will use surgical tools to cut sections of the colon or the entire colon for removal. Healthy colon tissue will be attached back together, called an anastomosis . Or, a stoma will be created for a colostomy or an ileostomy.
Open Surgery
In open surgery, one large incision will be created in the abdomen. The surgeon will complete the colectomy through this incision. The incision will be closed up after the surgery.
Procedure Types
There are many different types of colectomy procedures. Which one is chosen will depend on the reason for the colectomy, the person's health, and the potential for complications or continuation of the condition in the future.
In some cases, an ostomy may be needed temporarily. The ostomy could be reversed later. In others, a colostomy or ileostomy is placed.
The surgeon can tell you which type of procedure you will have. Sometimes, this plan must change or be adjusted during the surgery. Here is some of the terminology that may be used:
- Resection : A portion of the colon is removed, and the healthy tissue is reattached together.
- Right hemicolectomy : The ascending colon, on the right side of the body, is removed.
- Left hemicolectomy : The descending colon, on the left side of the body, is removed.
- Subtotal colectomy : The ascending and descending colon are removed, and the sigmoid colon (the last section) is left.
When Is a Stoma Necessary?
A stoma may be necessary if the colon needs time to heal or if the rectum and anus need to be removed. In colon cancer, a permanent stoma isn't usually required. For ulcerative colitis or Crohn's disease, a permanent stoma might be needed and may be planned from the outset of the surgery.
For ulcerative colitis, the ileostomy may be permanent, or there is an option to reverse it after having more specialized surgery to create a J-pouch from the terminal ileum. This procedure creates an artificial pathway for passing stool.
What Are the Risks of Colectomy?
As with any type of surgery, there is the potential for complications with colectomy surgery. One serious complication is bleeding. It is not a common occurrence, but bleeding has the potential to be serious.
Another potential complication during surgery is damage to surrounding organs and tissue. If this damage is found during the surgery, another procedure will be used to repair it.
After surgery, complications that may occur include infections and a leak at the site where the two healthy parts of the intestine were attached (anastomosis).
For a leak at the anastomosis site, more surgery may be needed to repair it. In some cases, a temporary ostomy may be used to allow the bowel to heal.
To avoid infections , antibiotics might be given before or during surgery. You will get instructions and assistance while in the hospital in using breathing treatments to prevent a lung infection and wound care to avoid an infection at the incision site.
Care will be taken to avoid infection, but if one does occur, treatment with antibiotics may be started.
How Long Does Recovery Take?
A colectomy is a major surgery. Recovery may take up to six weeks. Activity is usually ramped up slowly, such as returning to driving, household tasks, and work or school, as recovery continues.
Immediately after surgery, you will spend several days in the hospital receiving pain management and getting started on eating solid foods. You will also be shown how to care for incisions, especially when they are left open to heal. Those incisions will need to be packed with gauze and changed regularly.
Diet may initially consist of liquids and then move to solids as the bowel returns to normal functioning. You will be given directions on diet when you return home. The goal is to return to a regular, healthful diet as soon as possible.
Pain management in the hospital may be given intravenously. At home, oral pain medications, both prescription and over-the-counter (OTC), may be used until they are no longer needed.
What’s the Long-Term Outlook After a Colectomy?
Most people recover well from the surgery itself and won't experience any complications.
For the long-term outlook, the reason that the surgery is done in the first place may be the more important factor. Some conditions may require more treatment after surgery.
For example, Crohn's disease and ulcerative colitis will need to be managed even after surgery. This will mean regular appointments with healthcare providers, prescription or OTC medication, and monitoring for inflammation through endoscopic procedures and blood and stool tests.
Surgery for colon cancer may be followed by radiation and/or chemotherapy . You will need to follow up with your healthcare providers to monitor for recurrence of the cancer or other complications.
When to Contact a Healthcare Provider
After coming home from colectomy surgery, you should contact a healthcare provider if you experience any signs of a complication, such as:
- Redness, swelling, heat, or oozing of pus or other fluid at the incision site or sites
- Not having any bowel movements (constipation)
- Pain in the abdomen, especially if it becomes severe
- Fever, vomiting, or other signs of being unwell
A colectomy is a major abdominal surgery. It will require a stay of several days in the hospital and then several weeks of recovery at home. There is the potential for infection, bleeding, and damage to other organs, but the healthcare team will take steps to make the recovery process as event-free as possible.
Most people recover and return to work or school several weeks after the surgery. However, some people may need ongoing monitoring and care for any underlying conditions.
Meima-van Praag EM, Buskens CJ, Hompes R, Bemelman WA. Surgical management of Crohn's disease: a state of the art review . Int J Colorectal Dis . 2021;36(6):1133-1145. doi:10.1007/s00384-021-03857-2
MedlinePlus. Large bowel resection .
Misiakos EP, Tsapralis D, Karatzas T, et al. Advents in the diagnosis and management of ischemic colitis . Front Surg . 2017;4:47. doi:10.3389/fsurg.2017.00047
MedlinePlus. Total abdominal colectomy .
MedlinePlus. Total proctocolectomy with ileostomy .
National Institute of Diabetes and Digestive and Kidney Diseases. Treatment for diverticular disease .
American Cancer Society. Surgery for colon cancer .
National Institute of Diabetes and Digestive and Kidney Diseases. What to expect before and during ostomy surgery on the bowel.
Cancer Research UK. Surgery to remove all or part of your bowel (colectomy) .
National Institute of Diabetes and Digestive and Kidney Diseases. Types of ostomy surgery of the bowel .
National Institute of Diabetes and Digestive and Kidney Diseases. Treatment for Crohn’s disease .
National Cancer Institute. Do frequent follow-up tests benefit colorectal cancer survivors?
By Amber J. Tresca Tresca is a freelance writer and speaker who covers digestive conditions, including IBD. She was diagnosed with ulcerative colitis at age 16.
The Federal Register
The daily journal of the united states government, request access.
Due to aggressive automated scraping of FederalRegister.gov and eCFR.gov, programmatic access to these sites is limited to access to our extensive developer APIs.
If you are human user receiving this message, we can add your IP address to a set of IPs that can access FederalRegister.gov & eCFR.gov; complete the CAPTCHA (bot test) below and click "Request Access". This process will be necessary for each IP address you wish to access the site from, requests are valid for approximately one quarter (three months) after which the process may need to be repeated.
An official website of the United States government.
If you want to request a wider IP range, first request access for your current IP, and then use the "Site Feedback" button found in the lower left-hand side to make the request.

IMAGES
VIDEO
COMMENTS
This may mean asking friends or family to help during recovery. After surgery, you'll need to: Care for wounds, ... reassignment surgery? Gender reassignment is an outdated term for gender affirmation surgery. The new language, "gender affirmation," is more accurate in terms of what the surgery does (and doesn't) do. No surgery can ...
Transfeminine top surgery: Ranges from $3,000 to $11,000, depending on surgeon and location. Transfeminine bottom surgery: Starts around $4,000 for orchiectomy and goes up to $20,000 for vaginoplasty.
The cost of transitioning can often exceed $100,000 in the United States, depending upon the procedures needed. A typical genitoplasty alone averages about $18,000. Rhinoplasty, or a nose job, averaged $5,409 in 2019. Insurance Coverage for Sex Reassignment Surgery.
Gender-affirming surgery is a surgical procedure, or series of procedures, that alters a person's physical appearance and sexual characteristics to resemble those associated with their identified gender.The phrase is most often associated with transgender health care and intersex medical interventions, although many such treatments are also pursued by cisgender and non-intersex individuals.
Gender-affirming surgery for male-to-female transgender women or transfeminine non-binary people describes a variety of surgical procedures that alter the body to provide physical traits more comfortable and affirming to an individual's gender identity and overall functioning.. Often used to refer to vaginoplasty, sex reassignment surgery can also more broadly refer to other gender-affirming ...
Gender affirmation surgery, also known as gender confirmation surgery, is performed to align or transition individuals with gender dysphoria to their true gender. A transgender woman, man, or non-binary person may choose to undergo gender affirmation surgery. The term "transexual" was previously used by the medical community to describe people ...
Facial feminization surgery (FFS) is a series of plastic surgery procedures that reshape the forehead, hairline, eyebrows, nose, cheeks, and jawline. Nonsurgical treatments like cosmetic fillers ...
Surgery to change the appearance of your body is a common choice for all kinds of people. There are many reasons that people might want to alter their appearance.
By Kelly Bilodeau, Former Executive Editor, Harvard Women's Health Watch. Research we're watching. Gender-affirming surgery produces numerous benefits, according to a study by researchers from the Harvard T.H. Chan School of Public Health. These include better mental health, a reduction in suicidal thoughts, and reduced rates of smoking.
Overview. Feminizing surgery, also called gender-affirming surgery or gender-confirmation surgery, involves procedures that help better align the body with a person's gender identity. Feminizing surgery includes several options, such as top surgery to increase the size of the breasts. That procedure also is called breast augmentation.
Gender affirming surgery, also known as sex reassignment surgery (SRS) or confirmation surgery, is the surgical procedure(s) by which a transgender or non-binary person&rsquo;s physical appearance and functional abilities are changed to align with the gender they know themselves to be.
The meaning of GENDER REASSIGNMENT SURGERY is any of several surgical procedures that a transgender or nonbinary person may choose to undergo in order to obtain physical characteristics that align with their gender identity : gender confirmation surgery, gender-affirming surgery. How to use gender reassignment surgery in a sentence.
Definition of SRS. Sex Reassignment Surgery (SRS), also known as gender affirmation surgery or gender-confirming surgery, is a medical procedure that alters an individual's physical characteristics to align with their gender identity. In other words, it's a way to help transgender people feel more comfortable in their bodies.
Transgender people may seek any one of a number of gender-affirming interventions, including hormone therapy, surgery, facial hair removal, interventions for the modification of speech and communication, and behavioral adaptations such as genital tucking or packing, or chest binding. All of these procedures have been defined as medically ...
Risks and complications. There are always risks associated with surgery, but vaginoplasty complications are rare. Infections can usually be cleared up with antibiotics. Some immediate postsurgical ...
Gender affirming surgery can be used to create a vulva and vagina. It involves removing the penis, testicles and scrotum. During a vaginoplasty procedure, tissue in the genital area is rearranged to create a vaginal canal (or opening) and vulva (external genitalia), including the labia. A version of vaginoplasty called vulvoplasty can create a ...
Gender reassignment surgery is a series of complex surgical procedures (genital and nongenital) performed for the treatment of gender dysphoria. Genital procedures performed for gender dysphoria ...
Female-to-male surgery is a type of gender-affirmation or gender-affirming surgery. There are multiple forms of gender-affirming surgery, including altering the genital region, known as "bottom ...
You will need to do vaginal dilation for the rest of your life. Alissa (nurse): If you do not do dilation, your vagina may shrink or close. If that happens, these changes might not be able to be reversed. Narrator: For the first year after surgery, you will dilate many times a day. After the first year, you may only need to dilate once a week.
Sex and sexual health tips for transgender women after gender-affirming surgery. Sex after surgery. Achieving orgasm. Libido. Vaginal depth and lubrication. Aftercare. Contraceptions and STIs ...
Introduction. Discordance or misalignment between gender identity and sex assigned at birth can translate into disproportionate discomfort, configuring the definition of gender dysphoria. 1-3 This population has increased risk of psychiatric conditions, including depression, substance abuse disorders, self-injury, and suicide, compared with cis-gender individuals. 4,5 Approximately 0.6% of ...
It's essential to carefully consider all options and potential outcomes before undergoing surgery. 5. How long does it take to complete gender reassignment surgery? The duration of surgery varies ...
REASSIGNMENT meaning: 1. a process, including medical operations, by which someone's body is changed to match their…. Learn more.
Now, the Fourth Circuit Court of Appeals has decided that the amendment's "equal protection" clause means that state Medicaid programs have to cover gender reassignment surgeries. The appeals ...
As with any type of surgery, there is the potential for complications with colectomy surgery. One serious complication is bleeding. It is not a common occurrence, but bleeding has the potential to be serious. Another potential complication during surgery is damage to surrounding organs and tissue.
The definition of Federal financial assistance in this regulation does not constrain or otherwise limit the definition of Federal financial assistance under the Department's section 1557 regulations. ... including reassignment of services to already accessible facilities, redesign of equipment, delivery of services at alternate accessible sites ...
The definition of ``direct threat'' set forth in proposed paragraph (1) was added to be consistent with the ADA title II regulation and with the Supreme Court case of School Board of Nassau County v. ... Access to a program may be achieved by a number of means, including reassignment of services to already accessible facilities, redesign of ...